The effective management of diabetes requires meticulous glycemic control. The long-term complications resulting from poor glycemic control contribute substantially to the morbidity, mortality, and economic burden of diabetes.
The effective management of diabetes requires meticulous glycemic control. The long-term complications resulting from poor glycemic control contribute substantially to the morbidity, mortality, and economic burden of diabetes. Hyperglycemia in Type 2 diabetes worsens over time as a result of the decline in pancreatic β-cell function, increasing insulin resistance, and the increased hepatic glucose production associated with inappropriately high levels of glucagon and reduced glucagon-like peptide-1 (GLP-1) production.1 Consequently, a substantial number of patients need insulin therapy after nine or more years of disease.2
Advances in insulin therapy and other medications for the management of Type 2 diabetes have resulted in substantial improvements in glycemic control. However, these advances have not eliminated the psychologic and social burdens of the disease, such as fear of future complications and of hypoglycemia.3 While the patient’s attitude toward managing their treatment regimen is crucial to maintaining glycemic control,4,5 adherence to insulin, in particular, is poor in Type 2 diabetes.6 The requirement to inject current formulations of basal insulin analogs at a fixed time each day may negatively affect treatment adherence and patients’ quality of life (QoL) due to the complexity of the insulin regimen, needle phobia, the social stigma of having to inject insulin in public, and the risk for hypoglycemia.7–10 The American Association of Clinical Endocrinologists (AACE)/American College of Endocrinology (ACE) consensus panel has recommended that hypoglycemia be avoided where possible.11 The need remains for advances in current diabetes therapies that provide effective glucose control, maintain a stable glucose profile, and allow for more flexible treatment regimens that minimize side effects, particularly the risk for hypoglycemia.
This article aims to highlight advances in insulin therapy that aim to address the challenge of hypoglycemia in Type 2 diabetes, including combination therapies involving GLP-1 agonists, and two novel insulin analogs in clinical development: insulin degludec (IDeg) (Tresiba®, Novo Nordisk) and PEGylated insulin lispro ([LY2605541], Eli Lilly & Co).
Advances in Basal Insulin Analog Therapy
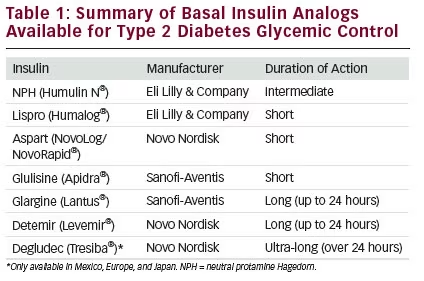
A summary of insulin analogs currently in use for glycemic control in Type 2 diabetes is shown in Table 1. Prior to the development of basal insulin analogs, neutral protamine Hagedorn (NPH), a suspension of crystalline zinc insulin combined with the positively charged polypeptide, protamine, was commonly used to provide basal glucose control. It has an onset of action beginning about 2 hours following injection, with a peak effect 4–6 hours after injection, and a duration of action of more than 12 hours. The resulting ‘dome-shaped’ basal plasma profile confers a risk for hypoglycemia at the peak insulin concentration and hyperglycemia at the trough.12
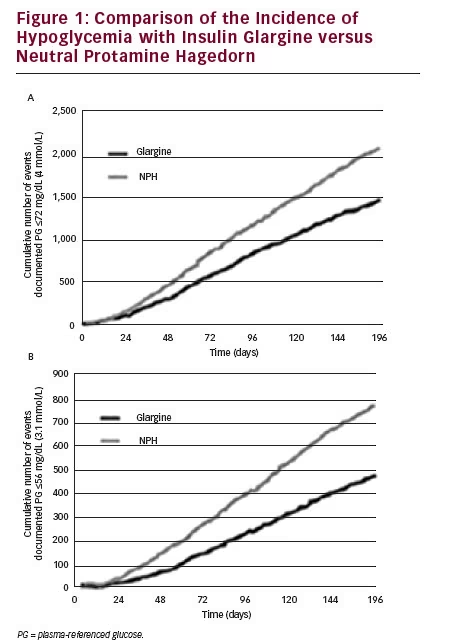
Long-acting basal insulin analogs have become important treatment options in Type 2 diabetes. The aim in developing such analogs has been to prolong the absorption kinetics to produce an absorption profile similar to that of endogenous basal insulin secretion. The flatter pharmacodynamic profile promotes a lower peak, a prolonged duration of action, and a slow and continuous absorption of insulin in the body that results in significant benefits in terms of glycemic control, flexibility of administration, and a reduced incidence of hypoglycemia compared with NPH (see Figure 1).13–15 Long-acting insulin analogs also have the advantage of providing a more consistent glucose-lowering effect throughout the day compared with shorter-acting insulin analogs.
The first long-acting insulin analog, insulin glargine ([IGlar], Lantus®), was introduced in 2002. Several studies have reported similar or slightly improved glycemic control with IGlar compared with once- or twice-daily NPH, with IGlar demonstrating a duration of action of up to 24 hours, and fewer episodes of nocturnal hypoglycemia.16–18 Another long-acting basal insulin analog, insulin detemir (IDet) (Levemir®, Novo Nordisk), was introduced in 2004, and comprises insulin linked to a fatty acid (myristic acid). In clinical studies, IDet provided predictable glycemic control with fewer hypoglycemic events (HEs) than NPH, but similar to glargine, and less weight gain compared with both NPH and glargine.19,20
Other advances include biphasic insulin analogs, which consist of a mixture of a soluble and a protaminated form of the rapid-acting analog, have shown improved postprandial glucose (PPG) control and a reduced risk for hypoglycemia compared with human premix formulations.21
Limitations of Basal Insulin Analog Therapy
Despite the reduced frequency of hypoglycemia associated with long-acting basal insulin analog therapy, hypoglycemia remains the major limiting factor in the treatment of Type 2 diabetes.22 The fear of hypoglycemia can delay the initiation of insulin;23 nocturnal hypoglycemia is of particular concern because many episodes are asymptomatic and may remain undetected until they become severe, which may lead to unconsciousness and even death.24 A recent survey of patients with Type 2 diabetes using basal insulin analogs (n=3,042) found that more than a third (36 %) had experienced HEs during the previous 30 days.25
Nonsevere HEs (NSHEs) may invoke a considerable economic burden for employers and patients, in addition to negatively impacting sleep quality, daytime functioning, and diabetes management among patients.26 A survey conducted in the US, UK, Germany and France (n=1,404) found that NSHEs were responsible for 8.3 to 15.9 hours of lost work time per month. Among respondents reporting an NSHE at work (n=972), 18.3 % missed work for an average of 9.9 hours (standard deviation [SD] 8.4); of those experiencing an NSHE outside working hours (including nocturnal), 22.7 % arrived late for work or missed a full day. Productivity loss was highest for NSHEs occurring during sleep, with an average of 14.7 (SD 11.6) working hours lost.27 Another survey (n=6,756) found that more than a third of respondents (36.1 %) reported a daytime NSHE in the past month. These occurred while active (e.g. running errands [45.1 %]), not active (e.g. watching TV [29.6 %]), and at work [23.8 %]). Patients took an average of half a day to respond to and recover from an NSHE, and monitored their glucose an average 5.7 extra times over the following week.28
In addition to its effect on day-to-day living, hypoglycemia can also have serious health consequences. Acute hypoglycemia causes the brain to become neuroglycopenic and promote secretion of counter-regulatory hormones – primarily adrenaline and norepinephrine. In healthy young adults, these effects are transient and have no obvious detrimental consequences. However, people with endothelial dysfunction are at an increased risk for localized tissue ischemia, which can alter a patient’s

cardiovascular (CV) risk profile.29–31 HEs (identified by the presence of an outpatient medical claim with an International Classification of Diseases, Ninth Revision, Clinical Modification [ICD-9-CM] diagnosis code) have been correlated with an increased risk for acute CV events (ACVEs) in patients with Type 2 diabetes,32 and severe hypoglycemia (defined as a blood glucose concentration of <2.8 mmol/l) was associated with increased mortality in the Action to Control Cardiovascular Risk in Diabetes (ACCORD) trial.33 HEs also result in impaired nutrient delivery to the brain, and may downregulate markers of neuronal plasticity and increase levels of neurotoxic glutamate, increasing the risk for dementia. A history of severe HEs has been associated with an increased risk for dementia in older patients with Type 2 diabetes.34 In summary, it is clear that hypoglycemia remains a serious challenge to patients taking basal insulin analogs, which highlights the need for basal insulin therapies that offer effective glycemic control while minimizing the risk for hypoglycemia.
Recent Advances in Managing Hypoglycemia in Type 2 Diabetes with Combination Regimens Involving Basal Insulin Analogs
Incretin-based therapies offer an effective new approach to the management of diabetes: GLP-1 receptor agonists and dipeptidyl peptidase-4 (DPP-4) inhibitors. Because of their glucose-dependent mechanism of action – they stimulate insulin secretion only during hyperglycemia – incretin-based therapies have a low hypoglycemia risk.
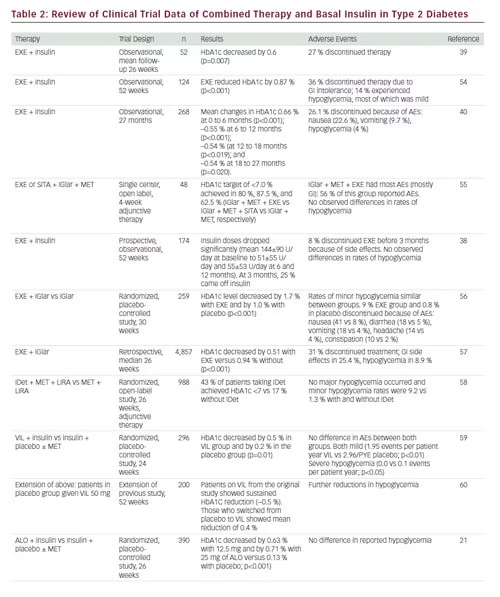
As a result of their complementary mechanisms of action, basal insulin analogs are increasingly used in combination with GLP-1 receptor agonists.35 Two GLP-1 receptor agonists are currently approved by the US Food and Drink Administration (FDA): exenatide (Byetta®, Bydureon®, Amylin Pharmaceuticals),36 and liraglutide, (Victoza®, Novo Nordisk).37 Several studies have investigated the efficacy and safety of the combination of GLP-1 receptor agonists and basal insulin; a summary appears in Table 2. All studies to date have shown that the combination of exenatide and insulin, with or without oral antidiabetes drugs, showed significant improvements in glycemic control with low incidences of hypoglycemia, often leading to dose reduction, or even discontinuation, of insulin. However, it must be noted that most of these studies were small, and most were either observational or retrospective. Increased reports of gastrointestinal (GI) side effects associated with the use of GLP-1 receptor agonists resulted in the discontinuation of a minority of patients in each of the studies.38–40
Although there are limited data comparing the rates of hypoglycemia in combined basal insulin regimens with those in monotherapy, the combination of GLP-1 receptor agonists and basal insulin has been associated with high patient satisfaction and low rates of hypoglycemia.41
Other combined therapeutic regimens that are being studied include the combination of insulin therapy with other incretin-based therapies. DPP-4 inhibitors are oral therapies that improve glycemic control in Type 2 diabetes by blocking the degradation of GLP-1 and glucose-dependent insulinotropic polypeptide (GIP). Several DPP-4 inhibitors have been approved by the FDA for use in Type 2 diabetes, including sitagliptin (Januvia®, Merck & Co, approved in 2006), saxagliptin (Onglyza®, Bristol- Myers Squibb, AstraZeneca, approved in 2009), linagliptin (Trajenta®, Eli Lilly & Co, approved in 2011), and alogliptin (Nesina®, Takeda Pharmaceutical Co., approved in 2013). Vildagliptin (Zomelis®, Abbott India Ltd, Galvus®, Novartis) has been approved in Europe but is not approved in the US.
A number of clinical studies have shown the efficacy and safety of DPP- 4 inhibitors as part of combined treatment regimens with basal insulin analogs, with low levels of hypoglycemia reported (see Table 2).
As a result of these studies, all FDA-approved GLP-1 receptor agonists and DPP-4 inhibitors have been approved for use as add-on therapy to basal insulin. Although incretin therapies are considered safe, there is a lack of long-term safety data relating to their use. Reports of associations between incretin therapies and acute pancreatitis are being investigated.42 While a large body of clinical data has demonstrated that combined regimens involving incretin-based therapies and basal
insulin analogs offer improved glycemic control with low incidence of hypoglycemia, there is a need for long-term data. It is not known how the efficacy of incretin-plus-insulin regimens will change in the course of the Type 2 diabetes disease process, and how and when doses should be adjusted. Therefore, more clinical trials are required to determine the appropriate use of incretin-based therapies combined with basal insulin.
Future Developments in Insulin Therapy
Recent research in insulin therapy has focused on the development of basal insulin analogs with an ultra-long duration of action. IDeg has a Figure 2: Phase III Trial-confirmed Hypoglycemic Events Comparing Insulins Degludec and Glargine A. Overall confirmed glycemic episodes. B. Nocturnal confirmed glycemic episodes. C. Diurnal confirmed hypoglycemic episodes. D. Cumulative number of hypoglycemic episodes per participant during 24 hours. E. Distribution of confirmed hypoglycemic episodes. Adapted from Figure 3, Garber, 2012.46 duration of action of more than 42 hours in adults.43 The basis for IDeg’s long duration of action lies in its structure: IDeg has the same amino acid sequence as human insulin except for the deletion of threonine in the B30 position and the addition of hexadecanedioic acid to lysine at the B29 position.44 This allows for the formation of multihexameric complexes as the additives in the formulation disperse, resulting in a subcutaneous depot from which IDeg monomers are slowly and continuously released into systemic circulation. The resultant smooth and stable pharmacokinetic profile provides an extended duration of action of up to 42 hours, minimizing the risk for hypoglycemia.
Pharmacokinetic and phamacodynamic studies have found that when administered once daily under steady-state conditions, IDeg has a more stable and consistent glucose-lowering effect than IGlar in Type 2 diabetes.45 This has been confirmed in clinical studies: in a phase III, open-label, treat-to-target, noninferiority trial (n=755), the rates of overall confirmed hypoglycemia were lower with IDeg than IGlar (11.1 and 13.6 episodes per patient–year of exposure [PYE], respectively; p=0.0359), as were the rates of nocturnal confirmed hypoglycemia (1.4 and 1.8 episodes per PYE, respectively; p=0.0399) (see Figure 2).46
A meta-analysis of clinical trials in the IDeg development program confirmed that similar levels of glycemic control were achieved with fewer hypoglycemic episodes, particularly nocturnal episodes, with IDeg compared with IGlar, across a broad spectrum of patients with diabetes.47
Since postprandial hyperglycemia contributes substantially to overall glycemia, initiating basal insulin therapy in combination with a rapid-acting insulin in one injection presents a convenient approach to achieving and sustaining optimal glycemic control. IDeg can be co-formulated with the rapid-acting insulin aspart (IAsp), resulting in the first soluble combination of two insulin analogs. IDegAsp, a co-formulation of IDeg (70 %) and IAsp (30 %), provided similar overall glycemic control to biphasic IAsp 30 with a significantly lower rate of hypoglycemia.48
IDeg has the potential to allow for a flexible, once-daily dosing regimen in which the patient can vary the daily injection time from day to day if needed. This flexibility provides convenience while maintaining glycemic control not only for those who self-administer insulin, but also for patients for whom insulin is administered by a caretaker or a third party who may not be able to visit the patient at the same time every day. Two recent studies investigated the efficacy and safety of IDeg in a flexible dosing regimen in patients with Type 1 and 2 diabetes and found that IDeg can be administered at any time of the day, with a varied injection time (8–40 hour intervals between daily injections), without compromising glycemic control or safety compared with same-time-daily IDeg or IGlar.49,50 IDeg has been approved in the EU, Japan and Mexico and is under review for FDA approval pending additional data.
Representing another recent advancement, insulin lispro has undergone PEGylation to produce a novel insulin analog. PEGylated lispro (LY2605541) comprises a 20 kDa polyethylene glycol (PEG) moiety covalently attached to lysine B28. It is designed to have a large hydrodynamic size that slows absorption and reduces clearance, resulting in therapeutically effective basal insulin activity and a longer duration of action.51 The efficacy of PEGylated lispro has been demonstrated in two phase II clinical trials. In a recent study comparing PEGylated lispro with IGlar, patients receiving the two agents had similar overall rates of hypoglycemia; however, fewer cases of nocturnal hypoglycemia were seen in the PEGylated lispro group.52 In a phase II study involving patients with Type 1 diabetes, PEGylated lispro demonstrated greater improvements in glycemic control compared with IGlar, and also caused weight loss. Mealtime insulin dose was decreased with PEGylated lispro, and increased with IGlar. The total rate of hypoglycemia was higher for PEG lispro (p=0.04), and the nocturnal hypoglycemia rate was lower (p=0.01).53 These results were obtained with a prandial dose of PEGylated lispro that was 24 % lower than the IGlar dose. Further research is required to determine the day-to-day variability of PEGylated lispro at doses relevant to clinical practice.
Summary and Concluding Remarks
Hypoglycemia remains the primary challenge in achieving and maintaining glycemic control with insulin therapy. The development of the long-acting analogs, IDet and IGlar, has resulted in improvements in the overall management of Type 2 diabetes, and specifically in reducing the rates of hypoglycemia, However, hypoglycemia remains a limiting factor in the intensification of insulin therapy.
Recent advances in the treatment of Type 2 diabetes include the combined use of incretin-based therapies with basal insulin analogs, a combination that has demonstrated improved glycemic control with the potential for reduced insulin dosing. Future advances are aimed at further reducing the risk for hypoglycemia through such novel insulin analogs as IDeg and PEGylated lispro, with studies showing that both agents have the potential to offer better glycemic control with less risk for nocturnal hypoglycemia compared with currently available basal insulin analogs. Moreover, IDeg offers patients the flexibility to vary the time of day at which the basal insulin can be administered when consistent timing of insulin administration is not possible or is impractical. The potential for fewer hypoglycemic episodes offered by combined regimens and new agents may bolster patients’ confidence in their ability to improve adherence to insulin regimens and maintain tighter glycemic control.







