Despite the introduction of newer and faster acting insulin analogues along with advances in glucose monitoring and insulin delivery technology, the majority of patients with type 1 diabetes (T1D) fail to achieve target glycemic control. There still remains a high burden of long term endorgan complications of T1D. Consequently, researchers continue to search for treatment modalities that not only preserve residual β-cell function, but also halt disease progression or even reverse the disease. An improved understanding of the complex immunological pathogenesis of T1D over the past decade has aided the identification of immunotherapeutics aimed at preserving residual β-cell function in high risk, and new onset T1D patients. However, previous intervention studies have not yielded adequate long term clinical benefit, a limitation many have suggested, results from our reliance on monotherapeutic approaches. Additionally, the task of employing safe and effective combination approaches has been challenging due to issues surrounding equipoise and an incomplete understanding of T1D etiopathogenesis. Herein, we provide a review of recently targeted pathways, drugs selected to augment those pathways, their respective clinical trials, relevant outcomes, and future directions.
Anti-CD3 antibodies
T-cells have been shown to have play an important role in the pathogenesis of T1D with autoreactive T effector cells (Teffs) bringing about islet cell destruction and suppressive T regulatory cells (Tregs) ameliorating autoimmunity. Hence, T-cells have been targeted in various immune interventions studies with the aim of preventing or delaying immune mediated destruction of β-cells. CD3, a transmembrane protein, acts as a co-receptor for the T-cell receptor (TCR), and is involved in activation and differentiation of naïve T-cells into pathogenic Teffs. Though not clearly understood, monoclonal antibodies against CD3 prevent activation and promote depletion of T-cells, with Teffs being more sensitive to the effects of anti-CD3 antibodies compared to Tregs. This leads to depletion of Teffs, restores the Teff/Treg ratio, and thus, promotes self- tolerance.1 Experimental studies in non-obese diabetic (NOD) mice have also shown that short term anti-CD3 antibody treatment can induce remission from disease.2,3
Otelixizumab is a humanised monoclonal antibody against CD3 with a mutation in the γFc portion, rendering it incapable of binding to the Fc receptor. The Fc mutation inhibits T-cell crosslinking, mitogenicity, and cytokine release. The Belgian Diabetes Registry conducted a randomised, placebo controlled, phase II study, where otelixizumab (48–64 mg) was administered over 6 days to new onset, T1D patients (12–39 yrs, T1D duration <4 weeks and positive for Epstein Barr virus [EBV] IgG). At 6, 12, and 18 months of follow up, subjects in the treatment group had a significantly higher stimulated C-peptide compared to placebo.4 At 36 months, those <27 years old in the treatment group continued to have higher C-peptide levels (80% higher) than in the placebo group of the same age range.5 Despite no significant differences in glycated haemoglobin (HbA1c) levels throughout the study, daily dose of insulin in the treatment group at all time points were significantly lower compared to placebo. However, one notable concern was the reactivation of EBV in more than 75% of the treatment group, though polymerase chain
reaction (PCR) copy numbers returned to normal levels 5–10 weeks post treatment.4
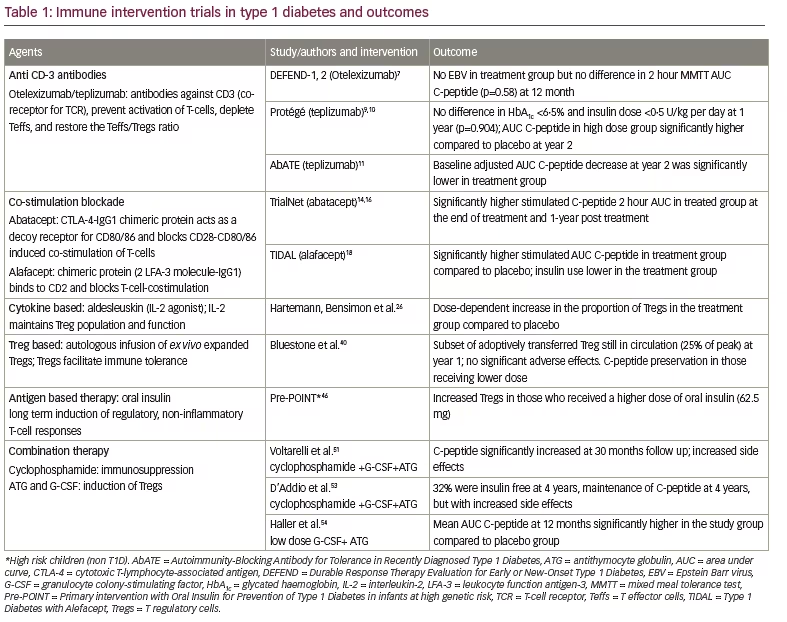
The DEFEND-1 and -2 (Durable Response Therapy Evaluation for Early or New-Onset Type 1 Diabetes) trials, were multicentre studies in new onset T1D adults and adolescents respectively (12–45 years old, T1D duration ≤90 days), designed to explore the efficacy of low dose otelixizumab in preserving residual C-peptide (Table 1).6,7 With a goal of reducing rates of EBV reactivation, the DEFEND-1 and -2 investigators utilised a lower dose of otelixizumab (3.1 mg). EBV reactivation and cytokine release syndrome rates were insignificant in the treatment group, but these were achieved at a cost of lower clinical efficacy. There was no difference in the 2-hour C-peptide area under the curve (AUC), mean HbA1c, and mean daily dose of insulin between the placebo group and the treatment group at 12 months. A dose finding phase II, single blind, randomised, placebo controlled study is currently underway where the efficacy and tolerability of escalating doses of otelixizumab (9 to 36 mg in four different arms) is being investigated in new onset T1D patients (16–27 years old, disease duration less than 32 days).8 The primary outcome of this trial includes the incidence of adverse events such as cytokine release syndrome and reactivation of EBV during the study and the follow up period, while the secondary outcomes include change in C-peptide AUC from baseline till month 24.
Teplizumab is another anti-CD3 monoclonal antibody similar to otelixizumab but with two mutations in its Fc portion. The Protégé study, investigated the efficacy and safety of low and high doses of teplizumab, in new onset T1D patients between 8-35 years old (Table 1). Patients were enrolled from 14 countries and randomised to 4 groups: 14-day high dose (9034 mcg/m2), 14-day low dose (2985 mcg/m2), 6-day high dose (2426 mcg/m2), or 14-day placebo at baseline and at 26 weeks. After 1 year, there was no difference in the primary outcome- the percentage of patients with HbA1c <6.5% and insulin dose <0.5 U/kg/day, across the four groups.9 Notably, this was one of the first interventional studies in which the primary outcome was not based on C-peptide and as such, the lack of achieving significance largely overshadowed the study’s effects on C-peptide preservation. At year 2, despite having no difference in HbA1c levels and mean insulin use per day, the 14-day high dose subgroup had a higher mean AUC C-peptide (p=0.027) compared to placebo. This benefit was more pronounced in patients with the following characteristics: young age (8–17 years), disease duration <6 weeks, HbA1c <7.5%, insulin dose of <0.4 U/kg/day, baseline mean AUC C-peptide >0.2 nmol/L, and US residents.10
The AbATE (Autoimmunity-Blocking Antibody for Tolerance in Recently Diagnosed Type 1 Diabetes) team also undertook a similar study with teplizumab; this was a randomised, open label, study in new onset T1D subjects (8-30 years old, T1D duration ≤8 weeks) (Table 1). The treatment group received teplizumab at a cumulative median dose of 11.6 mg (IQ range 5.7 mg) over 14 days. After a year, those in the treatment group who had detectable C-peptide after mixed meal tolerance test (MMTT), and meeting additional criteria, received another dose of teplizumab (median cumulative dose 12.4 mg, IQ range 5.08 mg). The adjusted mean C-peptide AUC level at year 2 was 75% higher in the treatment group compared to controls, even though there was no significant difference in HbA1c between the groups during the entire study.11 A post hoc analysis revealed that clinical responders, defined as those in the treatment group with <40% of C-peptide loss from enrollment, had lower HbA1c and daily insulin use at baseline after adjusting for C-peptide AUC. They also had increased circulating CD8 + central memory (CM) T-cells. The same study group recently demonstrated that the increased CD8+CM T-cells were derived from naïve T-cells; naïve T-cells have been demonstrated to be stimulated by anti-CD3 antibodies. However, clinical responders from the drug treated group had a higher expression of genes involved in T-cell regulatory pathways, and lower expression of genes involved in pathogenic T-cell activation which may explain the observed beneficial outcome.12 These observations also highlight the importance of patient population heterogeneity possibly influencing study outcomes.
In summary, large clinical trials studying anti-CD3 monoclonal antibodies in new onset diabetes have been carried out with each one reporting slightly different outcomes. These variable outcomes likely relate to differences in drug dosing, disease duration at enrolment, and baseline metabolic, immunological, and genetic differences in the study groups. Though these agents delay progression to complete insulin deficiency in new onset diabetes, the effects are unfortunately not sustained. This highlights the need for studies that will address dose ranging as well as redosing, and identification of new biomarkers capable of predicting responders. In addition, efforts to utilise anti-CD3 based approaches in pre-T1D subjects may be more efficacious. A randomised, double-blind, placebo-controlled clinical trial under the collaboration of TrialNet and the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) is currently investigating the efficacy of teplizumab in delaying or preventing clinical onset of T1D in non-diabetic, autoantibody positive, high risk individuals.13
Co-stimulation blockade
Activation of naïve T-cells not only requires TCR interaction with peptides presented by antigen presenting cells (APCs) but also co-stimulatory signals. These co-stimulatory signals are brought about by the interaction of T-cell surface receptor CD28 with CD 80/86 ligands on APCs. On the other hand, cytotoxic T-lymphocyte-associated antigen (CTLA-4), a homologue of CD28 inhibits T-cell responses after interacting with CD 80/86 ligands. Another co-stimulatory signal is the interaction of CD2, a T-cell surface membrane protein, with its ligand CD58 or leukocyte function antigen-3 (LFA-3) present on APCs. T-cells become anergic and refractory to further antigenic stimulation with blockade of these co-stimulatory signals.
Abatacept, a chimeric protein composed of human CTLA-4 receptor fused to a modified Fc portion of human IgG1, acts as a decoy receptor for CD80/86 and blocks CD28 induced co-stimulation. This interferes with T-lymphocyte activation, proliferation, and differentiation. Abatacept therapy in new onset T1D (6-45 years old, T1D duration <100 days) was investigated by the TrialNet study group wherein the treatment group received 27 infusions of abatacept over a 2-year period (Table 1). At the end of the treatment period, the abatacept group had a higher adjusted C-peptide AUC compared to placebo (59% higher, p=0.0029).14 Expansion of naive (CD45R0-CD62L+) CD4 T-cells was associated with a significantly slower rate of C-peptide decline in the treatment group, while increase in CM CD4 T-cells (CD4+CD45R0+CD62L+) was associated with C-peptide decline at the subsequent visit in the placebo group.15 There was also a significant reduction in the median percentage of Tregs from baseline at 6, 12, and 24 months. The decrease in Tregs could be explained by the fact that Tregs, like other T-cells, require co-stimulation for development and proper functioning. This decrease in Tregs was non-significantly associated with C-peptide level decline. This may also possibly explain the rate of C-peptide decline in the treatment group paralleling the placebo group (observed after 6–12 months of therapy), even though residual C-peptide was still much higher in the treatment group at all time points.16 The authors also pointed out that co-stimulation blockade only during the initial period of diagnosis may have a more favourable outcome, as the autoimmune process in the later part of the disease may be co-stimulation independent. It has been reported that T1D patients have persistence of circulating autoreactive effector memory T-cells (Tem) (both CD4+ and CD8+) which are less dependent on costimulatory signals for activation and clonal expansion, are more resistant to suppression by Tregs, and have increased homeostatic expansion following lymphodepletion.17 This highlights the importance of identifying and understanding the pathways associated with survival and proliferation of these autoreactive Tem cells.
Another T-cell co-stimulation blocking agent is alefacept, a fusion protein (2 molecules of LFA-3 fused to Fc portion of IgG1) that binds to CD2 on CD4+ and CD8+ Tem cells, and inhibits CD2 mediated T-cell co-stimulation. This brings about depletion of pathogenic Tem cells. The Immune Tolerance Network TIDAL (Type 1 Diabetes with Alefacept) study group investigated the effects of alafacept in new onset T1D patients (12-35 years old, T1D duration <100 days) (Table 1).18 Alafacept or placebo was administered as two 12-week courses at a dose of 15 mg/week. At 15 months post treatment, 2- and 4-hour MMTT AUC C-peptide in the treatment group was significantly higher compared to placebo (p=0.015 and 0.002 respectively); insulin use was also lower in the treatment group (p=0.002), along with reduction of hypoglycemic events by 50%. Notably, the best metabolic responses to alefacept were observed in younger subjects (similar to the Belgian Diabetes Registry and the Protege study). CD4+ and CD8+ central memory T-cells (Tcm) and Tem were significantly reduced in the alafacept group (p<0.01) with a higher Treg /Tem and Treg/Tcm ratio (overall p<0.01). The greater preservation of Tregs has been attributed to a lower expression of CD2 on Tregs compared to Tcm. However, there were no differences in T-cell subsets between complete responders (complete preservation of baseline 4-hour AUC C-peptide at 2 years) vs partial responders (preservation of 50% or more of baseline 4-hour AUC C-peptide at 2 years) vs poor responders in the alafacept group. Thus, a clear relationship between immune cell changes and clinical response could not be defined. It is unclear if this is due to heterogeneity in the involvement of the other arms of the immune system associated with T1D etiopathogeneis. This observation is in contrast to the abatacept trial where depletion of CD4+Tcm in a preceding visit was associated with better preservation of C-peptide at the subsequent visit. Despite the mechanistic differences, both trials have shown promising results and provide guidance for future studies. The abatacept study group is now investigating the efficacy of using co-stimulation blockade in delaying or altering disease course in autoantibody positive, high risk subjects.19
B lymphocyte based targets
Recent evidence has implicated B lymphocytes in T1D pathogenesis via their role in antigen presentation and T cell activation.20 CD20, a cell surface protein on B lymphocytes, is required for B-cell activation and proliferation, and thus has become a therapeutic target through the use of rituximab, a monoclonal antibody directed against CD20. The TrialNet study group investigated the efficacy of a four-dose course of rituximab in new onset T1D subjects (8-45 years old, T1D duration <3 months). Mean AUC C-peptide at year 1 was higher in the treatment group vs placebo (20%, p=0.03); the treatment group also had lower HbA1c and required less insulin.21 However, follow up of the cohort 30 months post randomisation, showed no difference in the rate of decline in AUC C-peptide between treatment group and placebo.22 The study group concluded that anti-B-cell therapy with rituximab can deplete B-cells with acceptable minimal side effects while ameliorating immune responses and preserving β-cell function. However, as B-cells are replenished rapidly as a homeostatic mechanism, there may not be a persistent effect on the major underlying disease pathology without the use of additional immunomodulatory approaches.
Cytokine based targets
Treg cell function has a critical role in controlling autoimmune or inflammatory responses and a shift in the Tregs/Teffs ratio or function (i.e. Tregs
Hartemann and Bensimon et al. conducted a phase I/II double-blind, placebo-controlled clinical trial to assess the efficacy and safety of low dose IL-2 (aldesleuskin) (0.33 MIU/day versus 1 MIU/day versus 3 MIU/ day x 5 days) in established T1D patients between 18–55 years old (Table 1).26 The authors reported a dose-dependent increase in the proportion of Tregs in the treatment group compared to placebo and with no serious adverse events. As there were no metabolic outcomes studied, it is unclear if the favourable immunological changes would equate to favourable clinical outcomes. A randomised, double-blind, placebocontrolled phase II study (DIABIL-2) in T1D subjects (12–35 years old, T1D durations <2 months) is currently ongoing with the primary outcome of AUC C-peptide change at 12 months from baseline.27 A non-randomised, open label, adaptive dose finding study by Waldron-Lynch et al. is also currently ongoing in T1D subjects with disease duration less than 2 years.28 The main objective of this study is to find the optimal minimal dose of IL-2 that would bring about targeted maximal increase in Tregs from baseline over the first 7 days following treatment.
IL-23 is another pro-inflammatory cytokine that has been targeted in immune intervention studies. It shares a p40 subunit with IL-12, another pro-inflammatory cytokine. Both IL-12 and IL-23 are involved in amplification of pro-inflammatory pathways and thus play key roles in autoimmune processes. Ustekinumab is a monoclonal antibody that targets the shared p40 subunit of IL-12 and IL-23, thereby blocking subsequent signalling and differentiation of central immune pathways. A phase I trial in new onset T1D subjects (18–35 years old, disease duration <100 days), looking into the safety profile of ustekinumab is currently ongoing, and is expected to end in 2016. The secondary outcomes of the study will elaborate on immunological and metabolic outcomes.29 Another phase I trial investigating the safety and clinical efficacy of the combined effects of ustekinumab and islet neogenesis associated protein (INGAP)-peptide (a β-cell regenerator), in established T1D subjects (19–40 years old), is currently underway.30 Other ongoing clinical studies targeting interleukins include the EXTEND trial, a phase II, randomised, double-blind, placebo-controlled trial in new onset T1D subjects (18–45 years old), where the role of tocilizumab, a monoclonal antibody against IL-6, in preserving residual β-cell function is being explored.31
Tyrosine kinase inhibitors
Imatinib and sunitinib are multi tyrosine kinase inhibitors (TKIs) initially studied in NOD mice and shown to preserve β-cell function. Although the precise mechanism underlying β cell preservation remains unclear, mechanistic studies have reported that inhibition of platelet derived growth factor receptor (PDGFR) may be involved.32 Beneficial effects of TKIs on β-cell function in humans are limited to anecdotal case reports. Huda et al. reported a 48-year-old female patient with T1D of 40 years’ duration who was treated with sunitinib for an underlying malignancy. Although the patient eventually succumbed to complications from her malignancy, the patient experienced complete remission from insulin 3 months after initiating sunitinib.33 A randomised, placebo-controlled, double-blind phase II study investigating the effects of imatinib on preservation of β-cell function in patients (18–45 years old) with new onset T1D (<3 months) is in progress.34
T regulatory cell based therapy Tregs are CD4+CD25+ T-cells that inhibit Teffs, control local cytokine or inflammatory responses and thus regulate autoimmunity and immune tolerance. Hence, Tregs remain an attractive target for many T1D researchers. In fact, decreased Tregs and/or defective activation and function have been reported in T1D subjects.35–38 Treg cell population expansion in vivo using various immune agents have been carried out in new onset T1D patients. Marek-Trzonkowska et al. carried out autologous infusion of ex vivo expanded Tregs in children with T1D (n=10, 8–16 years old, disease duration of 2 months) and compared to children who did not receive the Treg infusions.39 Two of the treated children were in remission 5 months after the infusion and 8 children required <0.5 U/kg/ day of insulin. The C-peptide in the treatment group was also significantly higher compared to the non-treated group (p=0.01).
Recently, Bluestone et al. have focused on the functionality of ex vivo expanded Tregs. He and his co-workers successfully carried out an open label, phase I trial where Tregs from T1D patients (n=14, disease duration 39±26 weeks) were harvested, expanded ex vivo using anti- CD3, anti-CD28, and IL-2 (Table 1).40 These autologous polyclonal Tregs were infused to the patients in four different cohorts of escalating doses of Tregs infusion. The infused Tregs showed robust suppressive function in in vitro studies and no major adverse events related to the treatment were noted during the study or in the follow-up period. One year following Treg infusion, almost 25% of the peak level of cells (in the assessed higher dose cohorts) remained in circulation. C-peptide levels were unchanged at 2 years from baseline in the two cohorts receiving lower dose of the Treg infusion, while those in the higher dose cohort had greater reduction in C-peptide by >50%. As the study was a phase I trial, it is too early to comment with certainty on the metabolic and immunological outcomes of autologous Treg infusion as well as the effect of dosing in T1D; a phase II study is being planned. The same study group has initiated a phase I trial looking into the safety of using polyclonal Treg plus IL-2 in new onset T1D subjects.41
Antigen based therapy
Antigen based therapies in T1D are rooted in the concept of ‘inverse vaccination’, where repeated introduction of exogenous autoantigens leads to long term induction of regulatory, non-inflammatory T- cell responses on re-exposure to the specific antigen. Although the mechanisms involved are much more complex than the above simplistic explanation with immune responses being influenced by the antigen dose as well as the route of administration, the potential outcome i.e., tolerance to islet autoantigens and suppression of autoimmunity provide an attractive solution to many T1D researchers. Additionally, as the autoimmunity against islet antigens in T1D is chronic, some researches have argued that current immunosuppressive interventions would only lead to transient remission of the disease and long term tolerance to islet antigen should be sought. Many autoantigen based therapies such as parenteral, nasal or oral insulin, glutamic acid decarboxylase (GAD) vaccines, DiaPep277 etc. have been evaluated in the last few years with either negative or non-conclusive outcomes. Non-islet antigen based therapies such as Bacillus Calmette-Guerin (BCG) vaccination, in new onset T1D have been carried out based on the concept of vaccination induced increase in tumour necrosis factor (TNF)-alpha levels, leading to killing of auto reactive pathogenic T-cells. However, the studies did not yield promising outcomes. Newer DNA based vaccines (autoantigen encoding plasmids) are now being studied in NOD mice. This section will review a few recent secondary prevention and new onset trials using antigen based therapies.
Oral insulin as a preventive agent in subjects at high risk for T1D is based on the concept of mucosal tolerance, where the unique immune lining of the gut processes foreign antigens and brings about clonal deletion or anergy of T-cells, and induction of Tregs.42 The Diabetes Prevention Trial– Type 1 (DPT-1) oral insulin study was one of the first large scale preventive trials in relatives of subjects with T1D. A total of 103,391 subjects were screened and 97,273 samples were analysed for islet cell autoantibodies. Of these, 3,483 were positive, 2,523 underwent additional testing, 388 were found to have a 5 year estimated risk of progression of 26–50%, and 372 were randomised to oral insulin or placebo. Unfortunately, annualised rate of diabetes was similar in both groups (p=0.189).43 However, a post hoc analysis showed a potential benefit of oral insulin in subjects with insulin autoantibody (IAA) ≥80 nU/mL. These “high titer” IAA subjects had an annualised diabetes rate of 6.2% with oral insulin and 10.4% with placebo (0.566, p=0.015).44 As the DPT-1 study was able to demonstrate successfully the capacity to perform large scale prevention studies, the Type 1 Diabetes TrialNet was established and now performs numerous prevention and intervention studies in T1D. A randomised, doubleblind, placebo-controlled trial is currently ongoing to re-test the DPT-1 observation that oral insulin may prevent T1D in subjects with high IAA.45
Recently, the Pre-POINT (Primary intervention with Oral Insulin for Prevention of Type 1 Diabetes in infants at high genetic risk) group studied the immunoprotective effects of increasing doses of daily oral insulin in antibody-negative children with T1D high risk human leukocyte antigen (HLA) class–II gene (2-7 years old) (Table 1).46 Children were randomised to receive either high dose or escalating doses of oral insulin (n=15) or placebo (n=10) once daily for 3 to 18 months. Nine children received insulin with dose escalations (6 months after the initial dose) from 2.5 to 7.5 mg (n=3), 2.5 to 22.5 mg (n=3), or 7.5 to 67.5 mg (n=3) after 6 months; 6 children received doses of 22.5 mg (n=3) or 67.5 mg (n=3) only. A higher number (5/6) of children who received 67.5 mg daily of oral insulin had increases in Tregs compared to the other subgroups (p=0.02) A longer follow up of this cohort may give additional information as to whether oral insulin can potentially prevent seroconversion in those at risk. Future studies should also include younger children (<2 years old) as seroconversion occurs mainly between 9 months to 2 years. In addition, TrialNet has initiated a small, open label, mechanistic study to assess the effects of varying doses and schedules of oral insulin on immunological and metabolic markers in relatives at risk for T1D the ages of 3-45 years (67.5 mg daily versus 500 mg every other week for 6 months.47
Other antigen based studies include a phase I trial investigating the safety of proinsulin peptide in new onset T1D (recently completed),48 and two ongoing randomised, double-blind, preventive phase II trials exploring the potential disease preventing effects of subcutaneous alum-GAD (DiAPREV-IT1)49 and in combination with high dose oral Vitamin D3 (DiAPREV-IT2),50 in non-diabetic, multiple antibody positive children between the ages of 4–18 years.
Combination immunomodulatory and immunosupressive therapies
Voltarelli et al. carried out a phase I/II study in new onset T1D patients (<6 weeks) where high dose immunosupresssion and autologous non myeloablative haematopoietic stem cell transplantation (AHST) were used to re-establish immune tolerance.51 Using a combination of cyclophosphamide (2 gm/m2) and granulocyte colony-stimulating factor (G-CSF) (10 μg/kg per day), haematopoietic stem cells (HSCs) were harvested and infused after the subjects were conditioned with cyclophosphamide (200 mg/kg) plus antithymocyte globulin ([ATG] 4.5 mg/kg) (Table 1). ATG and G-CSF both favour tolerance by modulating dendritic cells (DC) and induction of Tregs. During a mean follow up of 30 months, there was a significant increase in mean AUC C-peptide and the majority of patients were insulin free or required very low doses of insulin.52 After this study, three other independent clinical centres (one from Poland, two from China) investigated a similar protocol in new onset T1D patients (<6 weeks in the Polish cohort, and <12 months in the Chinese cohort).53 Fifty-nine percent of the subjects achieved remission from exogenous insulin at 6 months post treatment. At 4 years, 32% were still insulin independent (Table 1). Median C-peptide levels >1.15 ng/mL at 24 months of follow-up, and were still maintained in this range at year 4. Despite the beneficial effects seen on β-cell function and metabolic control, one of the major limiting factor of this protocol, was the high incidence of moderate to severe side effects. Fifty-two percent of the subjects reported adverse effects and one subject died due to Pseudomonas aeruginosa sepsis secondary to the high dose of the immunosuppressive agents.
Haller et al. subsequently developed a protocol in which cyclophosphamide was eliminated to avoid serious toxicity and a lower dose of ATG (2.5 mg/ kg) was used along with an extended course of G-CSF (6 mg peglylated G-CSF q 2 weeks x 6 doses) (Table 1).54 This randomised, single-blind, placebo-controlled, phase II study was carried out in subjects 12–45 years old (T1D duration >4 months to <2 years). Mean AUC C-peptide (4-hour MMTT) at 12 months post therapy, was significantly higher in the study group compared to placebo group (p=0.017). The majority of the subjects in the treatment group showed no decline in β-cell function even after 12 months. A significantly higher number of Tregs were also observed in the study group at 2 weeks and 12 months post treatment. Unlike high-dose ATG, the low dose ATG and G-CSF combination not only favoured the induction of Tregs, but also led to less severe T-cell depletion and allowed faster T-cell recovery. Only transient and fully reversible side effects such as cytokine release syndrome and serum sickness were reported in the study group.
As the sample size was small, a phase IIb, clinical study of the efficacy of ATG and G-CSF in new onset T1D (<3 months post diagnosis) patients is currently being conducted by TrialNet.55 Ongoing follow up of the original ATG/G-CSF pilot study subjects will help to determine if and when re-dosing with ATG/G-CSF or other immunotherapeutics is required to achieve long term preservation of β-cell function. In addition, Haller et al. have proposed the use of ATG/G-CSF and oral insulin as a potential option for utilising this combination approach in an effort to delay or prevent T1D in high risk subjects.
Conclusion
Although the last 20 years have seen major advances in the treatment of T1D associated with the development of insulin analogues, insulin pumps, and continuous glucose sensing, T1D is still associated with significant morbidity, mortality, and socioeconomic burden. Similarly, the search for an effective strategy to prevent and reverse T1D remains elusive. Significant but short term beneficial metabolic outcomes from past trials in new onset T1D patients have not always translated into complete independence from exogenous insulin, and it is questionable if this goal is pragmatic for those who already have clinical disease. Moreover, it is uncertain if the lack of success with immunotherapeutics is related to the relatively late phase of disease in which most trials have been performed, or the most appropriate combination of agents has yet to be studied, or the specific type of patient cohort most likely to benefit from these approaches has yet to be identified. An important aspect that should be contemplated in view of the recent finding of a more aggressive disease state in younger children with less residual β-cell function at diagnosis, is whether preventive interventions in high risk young children, will be more logical and efficacious rather than attempting to salvage residual insulin secretory capacity at diagnosis with immunosuppressive or immune modulating agents. On a contrasting note, recent new-onset trials have reported relatively better outcomes in the younger subjects compare to adults; however, these children were above 8–12 years of age.4,10,18 It remains unclear if the autoimmune process also differs between older children and adults. Identification of other factors, in addition to age, influencing disease heterogeneity is urgently needed.
This review has highlighted landmark immunotherapeutic trials in T1D. Notably, the majority of these studies have employed single immunomodulatory agents. As we enter the next era of T1D immunotherapeutic development with novel knowledge about the etiopathogenesis and heterogeneity of T1D, the focus of future preventive and intervention efforts is rapidly shifting towards the potential benefits of synergistic combinations. However, previous immune studies have demonstrated the potential pitfalls of combined strategies. For instance, it is questionable if antigen based therapies combined with immunosuppression would lack benefit or complete costimulation blockade with CTLA-4-Ig will reduce Tregs, and potentially exacerbate autoimmunity. Careful evaluation of the combined effects of proposed agents should be carried out before implementing new combinatorial trials in human subjects. Some potential synergistic combinations that could be evaluated in secondary preventive trials include antigen based therapies in conjunction with anti-inflammatory cytokines and/or Treg expansion. As for new onset intervention studies, agents that will ameliorate autoimmunity and preserve residual β-cell function may be more logical.
Ongoing efforts to better understand the heterogeneity of T1D will lead us to the development of more individualized intervention strategies for high risk, newly diagnosed, and long term T1D patients. It is only through logical efforts to simultaneously target complimentary pathways associated with progression to T1D that we can hope to improve our capacity to preserve beta cell function, and ultimately prevent and reverse T1D.







