Q. Why is molecular testing for thyroid cancer important?
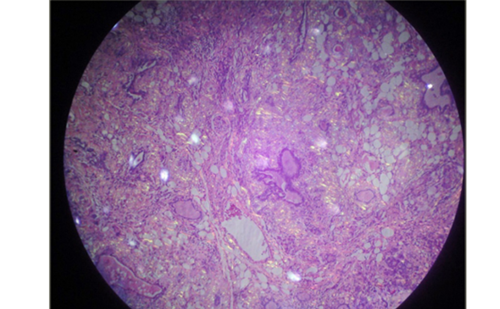
Assessment of risk of malignancy (ROM) in thyroid nodules is key to improved care. To assess ROM, we use medical history, physical examination, the results of ultrasound (US)-guided fine needle aspiration biopsy (FNA), and now we have molecular testing. Molecular testing can be diagnostic when used for thyroid nodules or prognostic in thyroid cancer.
For diagnostic use, several molecular tests are now available to separate benign from malignant nodules when FNA cytology is indeterminate. These tests are used by clinicians to avoid surgery when FNA is “suspicious,” i.e., neither benign nor malignant.
Q. What are the limitations of currently available tests?
The main limitation is that the tests are not widely available, particularly worldwide. Their cost is relatively high, especially outside the US. In addition, their positive predictive value is low, which means that when the test is positive, many nodules may not be malignant.
Q. How may these tests help in surgical decision-making in the future?
BRAFV600, a gene mutation in papillary thyroid cancer (PTC), is a marker of more aggressive tumor behavior. Thus, BRAF-positive tumors are more likely to metastasize to regional lymph nodes or have higher recurrence rates. The strongest argument against the use of BRAF mutation in surgical decision-making in practice is their high prevalence (30–80%) in PTC. However, it is expected that with more experience, molecular testing—including BRAF—will help us stratify our approach to thyroid cancer. For example, BRAF-positive tumors may require complete thyroidectomy and node dissection.
Q. How may molecular tests help determine prognosis?
A good example is the RET gene mutation in medullary thyroid carcinoma (MTC). When RET mutation is identified in the proband, family screening is relatively easy: those with a negative RET test are not at risk and need no further testing. Furthermore, it is recognized that some subtypes of RET mutations are associated with more aggressive tumors and when present, require more immediate and more aggressive surgery.
Q. What new tests are in advanced development?
Several tests are becoming available. The RET mutation in MTC is a well-established and useful test. The use of BRAF screening needs more evidence before it can be used in routine clinical applications. Testing for the RAS mutation is most common in follicular cancers. The presence of a BRAF mutation coexisting with TERT promoter mutations has been associated with a more aggressive clinical course, but this is not yet in routine use.
In addition, molecular targeted therapy is currently being studied for differentiated thyroid cancers.