Rationale for Development of a New Discipline
Lifestyle medicine is a nascent discipline that has recently emerged as a systematized approach for management of chronic disease. The individual elements and skillsets that define lifestyle medicine are determined, in large part, by the primary contributors to noncommunicable diseases (NCDs). Unhealthful lifestyle behaviors are among the leading risk factors for increased disability-adjusted life years (DALYs) in the US1 and around the world.2 DALYs have become an important metric for assessing health outcome and are defined as the sum of years of life lost to premature mortality and years lived with disabilities. Globally, NCDs account for about 63 % of all deaths. By 2030, it is estimated that NCDs may account for 52 million annual deaths worldwide.3 One of the primary aims of the 2011 UN high-level meeting of the General Assembly on noncommunicable diseases was as follows: “Reducing the level of exposure of individuals and populations to the common modifiable risk factors for NCDs, namely, tobacco use, unhealthful diet, physical inactivity, and the harmful use of alcohol, and their determinants, while at the same time strengthening the capacity of individuals and populations to make healthier choices and follow lifestyle patterns that foster good health.”4 More recently, the World Health Organization (WHO) published its 2008–2013 Action Plan for the Global Strategy for the Prevention and Control of Noncommunicable Diseases to prevent and control the four NCDs (cardiovascular diseases [CVDs], diabetes, cancers, and chronic respiratory diseases) and the four shared risk factors (tobacco use, physical inactivity, unhealthful diets, and harmful use of alcohol).5 These diseases are preventable. It is estimated that up to 80 % of heart disease, stroke, and type 2 diabetes (T2D) and more than a third of cancers could be prevented by eliminating these four shared risk factors. These four types of diseases and their risk factors are considered together in the WHO action plan to emphasize common causes and highlight potential synergies in prevention and control.
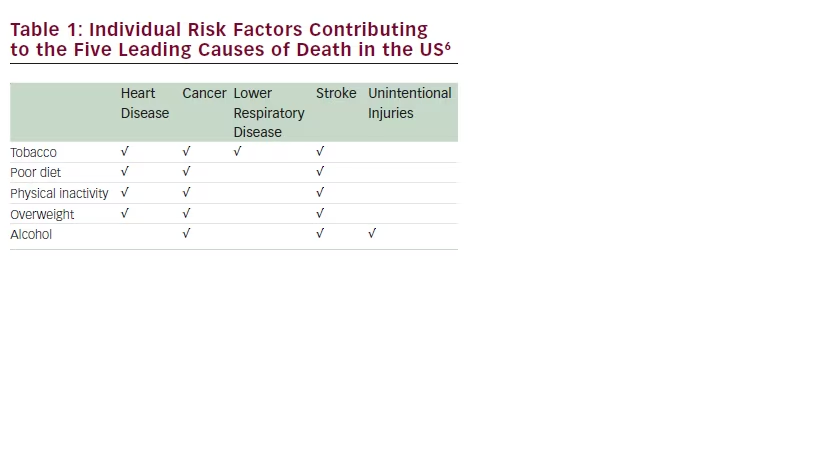
In the US, the five leading causes of death in 2010 were diseases of the heart, cancer, chronic lower respiratory diseases, cerebrovascular disease (stroke), and unintentional injuries.6 Among persons younger than 80, these five diseases represented 66 % of all deaths. Table 1 displays selected modifiable lifestyle risk factors for these diseases. Other modifiable risk factors associated with these diseases include sun exposure, ionizing radiation, and hormones (cancer); and air pollutants, occupational exposure, and allergens (lower respiratory disease).
There is a similarity of modifiable lifestyle risk factors for the five leading causes of death. The strength of the evidence regarding the effects of daily habits on health outcomes is further supported by comparing the leading clinical guidelines on prevention and treatment of disease (see Table 2).7–11
Individual lifestyle behaviors are among the five multiple determinants of health as defined by Healthy People 2020, the science-based 10-year national objectives for improving the health of all Americans.12 The other four determinants are environment, social, healthcare, and genetics and biology. In reality, the occurrence or reduction of individual risk factors closely align with the other major determinants. For example, whether an individual consumes an unhealthful diet or is physically inactive will depend, in part, on social, demographic, environmental, economic, and geographical attributes of the neighborhood within which the person lives and works.6
Defining Lifestyle Medicine
The proposed new discipline of lifestyle medicine differs from other closely aligned fields in medicine, such as preventive medicine, individualized or personalized medicine, and integrative medicine. Certainly there is overlap in the targets of intervention, but there are also important differences in philosophy and scope of practice. Preventive medicine focuses on the health of individuals, communities, and defined populations. Its goal is to protect, promote, and maintain health and well-being and to prevent disease, disability, and death.13 Individualized or personalized medicine tries to tailor medical interventions in terms of stratifying care by genetic characteristics.14 A recently suggested definition was offered by Schleidgen et al.15 as a discipline that “seeks to improve tailoring and timing of preventive and therapeutic measures by utilizing biological information and biomarkers on the level of molecular disease pathways, genetics, [and] proteomics, as well as metabolomics.”
Integrative medicine is closely aligned with lifestyle medicine in its core tenets. It has multiple definitions that describe a specialty that incorporates both conventional and alternative therapies. Rakel16 defines it as “[h]ealing-oriented medicine that takes account of the whole person (body, mind, and spirit), including all aspects of lifestyle. It emphasizes the therapeutic relationship and makes use of all appropriate therapies, both conventional and alternative.” According to Rees and Weil,17 “Integrated medicine selectively incorporates elements of complementary and alternative medicine into comprehensive treatment plans alongside solidly orthodox methods of diagnosis and treatment. It focuses on health and healing rather than disease and treatment.” The core competencies in integrated medicine for medical school curricula defines integrative medicine as “an approach to the practice of medicine that makes use of the best available evidence, taking into account the whole person (body, mind, and spirit), including all aspects of lifestyle.”18 Last, Snyderman and Weil19 define integrative medicine as “preventive maintenance of health by paying attention to all relative components of lifestyle, including diet, exercise, and well-being.”
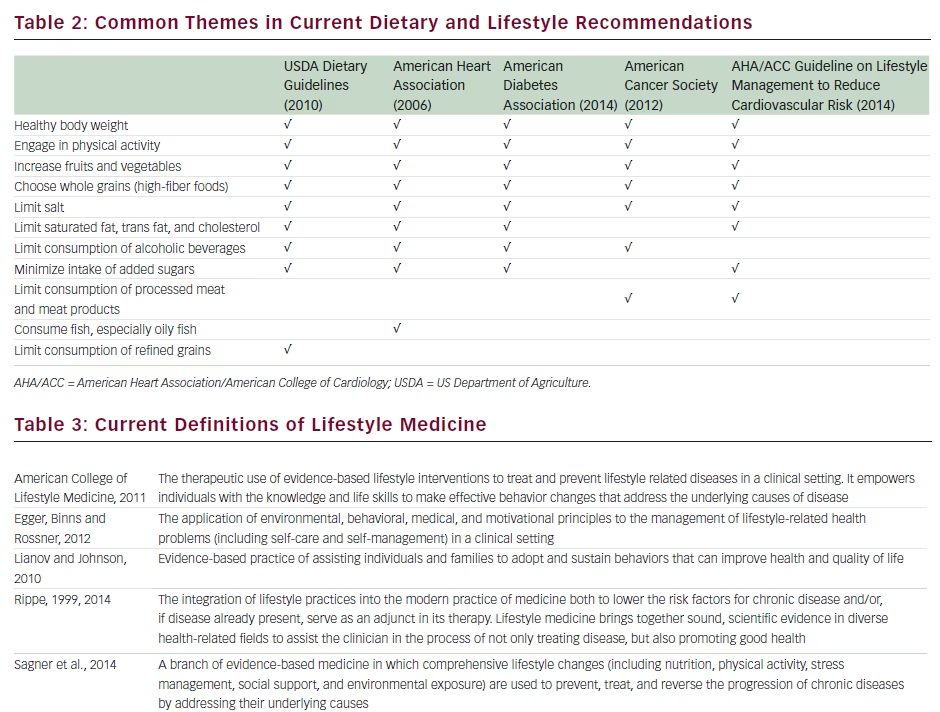
Much as is the case with integrative medicine, several definitions of lifestyle medicine have been proposed and are listed in Table 3.20–24 Common elements in all of these definitions are the application of evidence-based lifestyle interventions that promote self-management for promotion of well-being, prevention of illness, and management of chronic disease. Although medication adherence can be considered an aspect of self-care, most definitions consider lifestyle interventions to be used in conjunction with pharmacotherapy rather than encompassing drug therapy itself. To support this new initiative, the American Journal of Lifestyle Medicine was launched in 2007 in conjunction with the creation of a new academic medical society, the American College of Lifestyle Medicine (http://lifestylemedicine.org) and an educational track in lifestyle medicine, all announced at the American College of Preventive Medicine’s annual meeting. Societies promoting lifestyle medicine have also been formed in Europe (ESLM; https://eu-lifestylemedicine.org) and Australia (ALMA; http://lifestylemedicine.com.au). Other educational
initiatives include the Lifestyle Medicine Education Collaborative (www. LifestyleMedicineEducation.org) created to provide leadership, guidance, and resources to advance the adoption and implementation of lifestyle medicine curricula throughout medical education,25 and the Institute of Lifestyle Medicine (http://www.instituteoflifestylemedicine.org/) at the Joslin Diabetes Center. In short, lifestyle medicine is defined as the achievement of health in conjunction with the prevention or management of chronic disease by enhancing the power of self-care behaviors.
Effects of a Healthful Lifestyle on Chronic Disease
There is a strong body of evidence to show that practicing healthful lifestyle behaviors reduces the risk for chronic disease. In 2009, the American College of Preventive Medicine published a comprehensive review of the scientific evidence for lifestyle medicine both for the prevention and treatment of chronic disease.26 Twenty-four chronic diseases were reviewed in this publication, highlighting the effects of a healthful lifestyle on improving the root causes of disease.
Recently, multiple systematic reviews and meta-analyses have been published that demonstrate the beneficial effect of lifestyle interventions in reducing T2D incidence in patients who have impaired glucose tolerance,27,28 management of T2D,28-30 hypercholesterolemia,31 CVD,11 and metabolic syndrome.32,33 In a NIH–AARP population-based cohort study of 207,449 men and women, the 11-year risk for incident T2D for men and women whose diet score, physical activity, smoking status, and alcohol use were all in the low-risk group had odd ratios (ORs) for T2D of 0.61 and 0.43, respectively, compared with the high-risk group.34 T2D and obesity are among the two most significant NCDs, currently affecting 366 million and 500 million people worldwide, respectively35,36 and often called “diabesity” because of their close association. One of the most effective targets for T2D treatment is management of excess body weight by diet and physical activity. The beneficial effect of weight loss on glycemic control and reduction of cardiovascular risk factors has been recently demonstrated in the Look AHEAD (Action for Health in Diabetes) trial. In this prospectively controlled, randomized study conducted at 16 US research centers, 5,145 overweight adults aged 45–76 and having T2D were randomly assigned either an intensive lifestyle-based weight loss intervention (ILI) or a diabetes support and education intervention (DSE).37 Although 4-year results showed statistically significant improvements in fitness, glycemic control, and cardiovascular risk factors,38,39 the trial was discontinued in September 2012 after a median follow-up of 9.6 years on the basis of a futility analysis.40 The probability of observing a significant positive result at the planned end of follow-up was estimated to be 1 %. Proposed explanations for the lack of significant difference in rates of cardiovascular events between the ILI and DSE groups include a 2.5 % difference in weight loss between groups at
year 10, intensification of medical management of cardiovascular risk factors, and low event rate.41
Over the past few years, there has been an increased interest in evaluating the benefit of adhering to “low-risk lifestyle” behaviors on the development of morbidity and mortality. Although the criteria for defining low-risk lifestyle factors vary, these studies have shown that adherence to a healthful lifestyle is associated with improved health outcomes. The following population studies are notable for their size and magnitude in demonstrating the potential effects of fostering lifestyle medicine as a new discipline.
- In the European Prospective Investigation Into Cancer and Nutrition (EPIC) study, 23,153 German participants aged 35–65 were followed up for a mean of 7.8 years. Adherence to four health behaviors (not smoking, exercising 3.5 hours per week, eating a healthful diet [high intake of fruits, vegetables, and whole-grain bread and low meat consumption], and having a body mass index [BMI] of <30 kg/m2) at baseline was associated with 78 % lower risk for developing chronic disease (T2D 93 %, myocardial infarction 81 %, stroke 50 %, and cancer 36 %) than participants without the healthful factors.42
- In the Nurses’ Health Study, a prospective cohort study of 81,722 US women from 1984 to 2010, a low-risk lifestyle was defined as not smoking, having a BMI of less than 25 kg/m2, exercise duration of 30 minutes/day or longer, and being in the top 40 % of the alternate Mediterranean diet score, which emphasizes high intake of vegetables, fruits, nuts, legumes, whole grains, and fish and moderate intake of alcohol. Compared with women having no lowrisk factors, the multivariate relative risk for sudden cardiac death (SCD) decreased progressively for women having one, two, three, and four low-risk factors to 0.54, 0.41, 0.33, and 0.08, respectively. The proportion of SCD attributable to smoking, inactivity, overweight, and poor diet was 81 %.43
- The Atherosclerosis Risk in Communities Study (ARIC), a prospective epidemiologic study of 15,792 men and women aged 44–64 years at enrollment, demonstrated that adopting a healthful lifestyle after age 45 results in substantial benefits after only 4 years compared with people living less healthful lifestyles, reducing mortality, and CVD risk by 40 % and 35 %, respectively.44
- To further explore the relationship between change in health behaviors, socioeconomic status, and mortality, Stringhini et al.45 followed a cohort of 10,308 civil servants from baseline examination (1985–1988) to phase 7 (2002–2004) in the British Whitehall II study. After adjusting for sex and year of birth, those having the lowest socioeconomic position had 1.60 times higher risk for death from all causes than those with the highest socioeconomic position. However, this association was attenuated by 72 % when four health behaviors (smoking, alcohol consumption, diet, and physical activity) were entered in the statistical model.
- In a population-based prospective cohort of 20,721 Swedish men aged 45–79 without history of chronic disease, followed for 11 years, five low-risk behaviors (healthful diet, moderate alcohol consumption, no smoking, physical activity, and healthy waist circumference) were associated with an 86 % lower risk for myocardial infarction events compared with the high-risk group with no low-risk factors.46
Another approach used to assess the burden of disease is to combine lifestyle and physiologic risk factors. This has been extensively applied to CVD. In the INTERHEART study, a case control study of acute myocardial infarction across 52 countries, 15,152 cases and 14,820 controls were enrolled between 1999 and 2003 to assess the effect of risk factors on development of coronary heart disease.47 The study showed that more than 90 % of the proportion of risk for an initial myocardial infarction is collectively attributable to nine measured and potentially modifiable risk factors: cigarette smoking, diabetes, raised ApoB/Apo A1 ratio, hypertension, abdominal obesity, psychosocial factors, daily consumption of fruits and vegetables, regular alcohol consumption, and regular physical activity.
The concept of “cardiovascular health metrics” has also emerged as a method to assess cardiovascular risk and has been called “Life’s Simple 7” by the American Heart Association (AHA) in its 2020 Strategic Impact Goals targeting a 20 % relative improvement in overall cardiovascular health in all Americans.48 The AHA combines four health behaviors (smoking, diet, physical activity, and body weight) with three health factors (plasma glucose, cholesterol, and blood pressure) as metrics and assesses adherence as poor, intermediate, or ideal by distinct definitions.49 The AHA also recently published 11 comprehensive articles in a themed series, “Recent Advances in Preventive Cardiology and Lifestyle Medicine,” emphasizing the multiple determinants of cardiovascular health.50 Finally, Yang et al.51 analyzed the associations between the number of ideal cardiovascular health metrics and mortality over a median follow-up of 14.5 years using data from the National Health and Nutrition Examination Survey (NHANES). Compared with individuals having zero or one metric at ideal levels, those having six or more metrics at ideal levels had 51 %, 76 %, and 70 % lower adjusted hazards for all-cause, CVD, and ischemic heart disease mortality, respectively.
Practitioner Skills for Lifestyle Medicine
The practice of lifestyle medicine is dependent upon the provider’s ability to implement and sustain behavior change in patients regardless of the target behavior—e.g., smoking cessation, reduction in alcohol use, increasing consumption of fruits and vegetables, engagement in physical activity, and reducing body weight. As already noted, the five determinants of health defined by Healthy People 202012 that influence health outcomes are individual behavior, environment, social, healthcare, and genetics and biology. The term “behavioral” refers to underlying processes, such as cognition, emotion, temperament, personality, and motivation. The term “social” encompasses sociocultural, socioeconomic, and sociodemographic status.52 Attention to these and other contextualizing factors is important to further understand the barriers that patients face when implementing lifestyle changes. How we help patients change behavior represents a set of cognitive tools grounded in behavioral science.
The social determinants of health—i.e. the economic and social conditions that influence the health of people and communities—are particularly important in the practice of lifestyle medicine and present several considerations that must be incorporated when providing effective counseling. The first is health disparities, which encompass an appreciation of the racial, ethnic, and cultural factors that affect treatment decision-making. Cultural competence refers to having the capacity to function effectively as a healthcare provider within the context of the cultural beliefs, practices, and needs presented by patients and their communities.53 By contrast, cultural humility implies having an attitude that acknowledges that a patient’s culture can only be appreciated by learning from the patient. The second consideration is health literacy, often defined as a set of skills that people need to function effectively in the healthcare environment.54 It represents the capacity for individuals to obtain, communicate, process, and understand health information and services to make appropriate decisions.55 The skills include the ability to read and understand text, interpret information, and speak and listen effectively. These skills are particularly important when we ask patients to track their diet, read food labels, incorporate behavioral advice, or take prescribed medication. Low health literacy is associated with poorer health outcomes and poorer use of healthcare services.54
The concept of shared decision-making (SDM) is stipulated in the Affordable Care Act to ensure that medical care better aligns with patients’ preferences and values.56 SDM describes a collaborative process between patients and their clinicians to reach agreement about a health decision that may involve multiple treatment options and targets or therapy.57,58 Clinicians and patients work together to clarify the patients’ values and concerns, select a preference-sensitive decision, and agree on a follow-up plan. Intrinsic to SDM is the use of patient decision aids, which include written materials, videos, and interactive electronic presentations designed to inform patients about care options.56 An example of SDM using a patient decision aid is smoking cessation counseling. The pros and cons of gradual reduction in the number of cigarettes smoked versus abrupt cessation can be discussed along with which (if any) of the multiple pharmacotherapy treatments to choose
Implementation of Lifestyle Medicine in Clinical Practice
Despite the appeal of this new emerging discipline, existing evidence for implementing lifestyle medicine counseling in primary care is mixed and limited. The US Preventive Services Task Force (USPSTF) found that the health benefit for diet, physical activity, and behavioral counseling to prevent CVD in the primary care setting is small (Grade C).59,60 By contrast, the USPSTF found stronger albeit modest evidence for diet and physical activity counseling for CVD prevention in adults with existing cardiovascular risk factors (Grade B) 61 and behavioral counseling for obesity (Grade B).62, 63 The research data on management of obesity in primary care is most intriguing. Although intensive behavioral counseling has been found to be effective, studies demonstrating successful implementation in primary practice are limited.64,65 Even if the primary care system- and practice-based barriers are ameliorated, implementation of lifestyle medicine will require multiple strategies that incorporate public health, environmental, and community approaches.66,67
Conclusion
A significant body of literature demonstrates that adoption of lowrisk lifestyle behaviors and ideal cardiovascular health metrics are associated with reduced morbidity and mortality. However, there is also considerable evidence that healthful lifestyle behaviors are incorporated by a minority of the population. Lifestyle medicine presents a new and challenging approach to address the prevention and treatment of NCDs, the most important and prevalent causes for increased morbidity and mortality worldwide. Good communication between the provider and patient is paramount in eliciting behavior change. Rather than simply educating and instructing patients about what to do, behavior change counseling should be a guiding and collaborative process.