Type 2 diabetes mellitus (T2DM) is a chronic disease characterised by hyperglycaemia and compounded by insufficient production of insulin (beta cell dysfunction) to overcome the ineffective action of insulin (insulin resistance). According to International Diabetes Federation Eighth Atlas (2017), there were 425 million diabetic people (20–79 years of age) worldwide.1 The number of people affected by diabetes is expected to reach 629 million by 2045.1 Unique challenges with diabetes in India include the high prevalence of the disease (9% for diabetes and 12–15% for prediabetes), nearly 2 decade earlier onset of T2DM among Indians, as compared to the rest of the world, a more aggressive disease phenotype (highest rates of prediabetes progression to diabetes of 18% per annum), increasing problem of obesity, and primarily effecting the economically productive population (age 18–60 years) of the society.2,3
Optimal and appropriate diet, calorie restriction, physical activity and medication adherence are four key pillars of therapeutic lifestyle interventions in the management of diabetes.4,5 In spite of awareness, poor compliance to therapeutic lifestyle interventions contributes to poor glycaemic control and increased end-organ damage resulting in poor quality of life in the long run. This perpetuates a viscous cycle of poor control and further complications, which at times, becomes difficult a difficult cycle for the patient to break.6 The important factors which contribute to medication non-adherence are knowledge and perception of disease, complexity of dosing regimen and difficulty in managing complex treatment regimens or their side effects, financial constraints, psychological factors, and lack of social support.5–7
Family support and social relationships, as a part of individual treatment and healthcare, are beneficial for better glycaemic control and improved quality of life.7 Health-related behaviour change interventions influence healthier lifestyles among people with diabetes but the effectiveness and sustainability is low.8,9 The role of family support and especially the spousal relationship is an important component outside of the social networks, as the partner spends a considerable portion of his or her life in the shared environment. Joint management efforts with spousal participation are hypothesised to produce effective and sustainable results in diabetes management.10,11 Hence the aim of this review is to analyse the literature to develop better insights regarding successful implementation of lifestyle intervention programmes in diabetes. There is a special focus on evaluating the role of family and partner support in successful implementation of therapeutic lifestyle programmes.
Methods
A literature search was performed in PubMed, Medline and Embase for articles published before July 2018, using the terms “therapeutic lifestyle intervention” [MeSH Terms], OR “diet changes” [All Fields], OR “spousal participation” [All Fields], OR “lifestyle interventions” [All Fields], “lifestyle changes” [All Fields] AND “diabetes” [All Fields]. The reference lists of the articles identified were also searched. The search was not restricted to English-language literature; literature in Spanish, French and German were also evaluated.
Results
A total of 66 articles were reviewed, which included 33 original work, 21 review articles and 12 systematic reviews and meta-analysis. The key information obtained from these articles has been elaborated below.
Effectiveness of lifestyle interventions in people with type 2 diabetes mellitus
Lifestyle intervention such as proper diet and physical activity, can improve glycaemic control and other metabolic risk factors, which in turn, has the potential to prevent diabetic complications. Huang et al. conducted a systematic review and meta-analysis of 17 randomised clinical trials comparing lifestyle intervention with “usual care” (control) in patients with T2DM and found that dietary intervention showed an improvement in glycated haemoglobin (HbA1c), systolic/diastolic blood pressure and high-density lipoprotein (HDL) cholesterol, suggesting that nutritional intervention had a significant impact on different components of metabolic syndrome, and hence has a potential to reduce cardiovascular risk in T2DM.12
Cezaretto et al. conducted a systematic review and meta-analysis of randomised controlled trials found a significant reduction in depression scores following lifestyle interventions in the pooled analysis (standardised mean difference [SMD] -0.165; 95% confidence interval [CI] -0.265, -0.064; I[2] 67.9%) and when limited to individuals with T2DM (SMD -0.202; 95% CI -0.288, -0.079; I[2] 72.5%).13 Htoo et al. found that Southeast Asian adults with diabetes who received lifestyle modifications for 3 months had statistically significant reductions in HbA1c, compared to the control group.14 However, the effects tended to blunt out after 6 months of follow up (i.e., non-significant reduction in HbA1c in the intervention group compared to the control group beyond 6 months follow up).14,15
The above data provides evidence to support the role of therapeutic lifestyle interventions in improving glycaemia and other complications associated with diabetes. They can also be effective for other associated features such as depression. However, evidence for long-term sustainability beyond 6 months, especially in Asians, needs to be further assessed in people with diabetes.16 It may be hypothesised that poor compliance to therapeutic lifestyle interventions beyond 6 months may contribute to its decreased efficacy over long periods of time
Real-world challenges to the implementation of therapeutic lifestyle interventions
Adherence to treatment
Low compliance to prescribed treatment approaches is a common problem in patients with chronic diseases.17,18 A meta-analysis published in 2018 (including 2,491 screened records and 24 studies on 369,251 people from 20 countries) reported that target achievement rates for glycaemic control were 42.8% (95% CI 38.1–47.5%).19 The World Health Organization (WHO) has reported that approximately 50% of patients with a chronic illness are non-adherent with their treatment regimen (diet, activity, monitoring and medications); the rate is even higher in developing countries.20 A review article published in 2014 focusing on qualitative research, meta-syntheses, and meta-ethnography articles estimated more than 40% non-adherence to treatment and medical recommendations among patients with T2DM.21
The factors associated with such non-adherence could be patient related, such as understanding of the disease, coping mechanisms, motivation for control; family related factors, such as social or financial support; treatment related, such as simplicity and effectiveness of regimen; or healthcare related, for example easy accessibility to competent doctors and relationship with healthcare professionals.22–25 Evidence-based research should explore further possible factors, their operational mechanisms and possible solutions (as summarised in Tables 1 and 2) to overcome non-adherence and improve glycaemic management.26–30 The pragmatic understanding of the various reasons of non-adherence, changes in attitude and motivation along with intensive treatment and lifestyle interventions in group setting are evidenced to improve adherence to the lifestyle recommendations and glycaemic outcomes.31 Overcoming these factors with a multifaceted approach can help in achieving good treatment outcomes, with improvement in quality of life for patients.
Given the challenges of non-adherence, family involvement can be greatly beneficial in therapeutic lifestyle programmes, as seen in Figure 1.23,25,26,29,30
Diabetes distress
Clinical depression and diabetes distress are prevalent emotional states found among people with diabetes, which can significantly affect the glycaemic control; lower blood glucose monitoring frequency; and increase micro-vascular complications, healthcare use and expenditures.32 Lack of social support is determined to be a major risk factor for diabetes distress, and social stigma often prevents discussing or seeking help for psychological problems.33 Positive spousal support in T2DM intervention programmes has been evidenced as a moderator between psychological morbidity to promote adherence to treatment therapies, patient satisfaction with healthcare services, and compliance to therapeutic lifestyle interventions.34
Exploring family-based approach to cope with real-world challenges
It has been shown that family participation can improve the effectiveness of lifestyle interventions for enhancing diabetes self-management. People eat and enjoy meals together in routine and rituals with family members which influence dietary patterns; consistent bad dietary habits can have adverse health potentials.35 On the other hand, any cumbersome dietary changes which are difficult to accept, in society or by the people they live with, can ultimately lead to non-adherence or non-compliance. Contextually, a study conducted in 2017 assessed interconnected problem domains (knowledge, communication, support, everyday life, roles and worries) to understand how family involvement can be supported in healthcare practices.36 Similarly, a systematic review conducted in 2017, identified the behavioural influence (in terms of facilitators, barriers or equivocal behaviours) affecting an individual’s diabetes self-management.37 The important themes that emerged from these, and other studies in this context, are described as follows:
Table 1: Factors affecting treatment adherence and strategies to overcome these
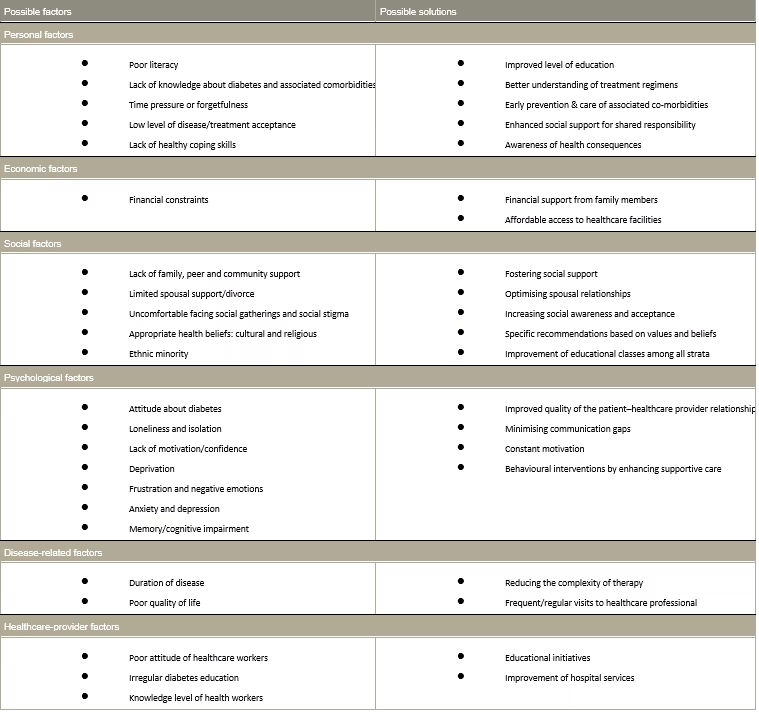
Figure 1: Approach of lifestyle interventions towards diabetes self-management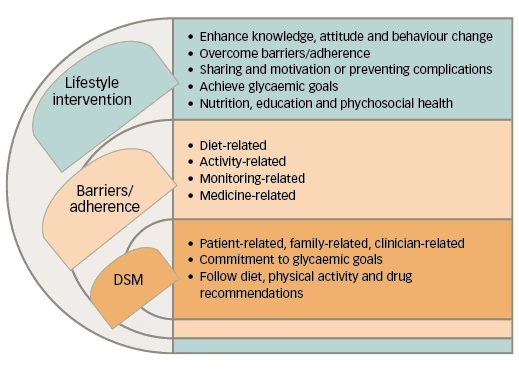
Facilitating behaviours
Positive family participation can encourage positive choices and will assist the patient to identify and overcome barriers to adherence. It can influence the patient’s psychological wellbeing, informational and financial support, and give them the confidence to follow recommendations resulting in behaviour change to adopt healthy diet, lifestyle, exercise and timely medical regimen. Family participation can also lead to improvements in glycaemic control and diabetes self-management via shared health-related activities or tasks together.38 It provides vigilance over changes in their clinical status or progressing complications.37 Finally, it enhances motivational skills for self-sufficiency, positive behaviours and independent attitudes towards disease.39–41
Negative behaviours
Despite positive influence, family participation may also lead to obstructive behaviours, refusal to share the burden and limited family support or engagement.42 The practice of unhealthy dietary habits or lifestyle routines; lack of emotional, physical and financial support; and lack of empathy, awareness, understanding and knowledge can all contribute towards non-adherence to treatment and disease management.37,43,44
Equivocal behaviours
Family behaviours such as reminders for appointments with healthcare professionals, taking medications, exercising and maintaining a healthy diet can affect as both facilitator of or barrier to diabetes self-management.37,45
Overcoming barriers
Enhancing the facilitating behaviours, overcoming the negative behaviours and optimising or reinforcing the equivocal behaviours are major facets towards effective adherence and glycaemic achievement.46,47 Family members can encourage the patient, change the types of food prepared or consumed, can enjoy similar food in a comfortable environment, engage in physical activities, attend medical visits with the patient, reprioritise family finances, and make necessary lifestyle changes. All of these supportive actions will help towards improving dietary habits, adherence to the treatment, healthcare and the patient’s clinical outcomes.40,48,49
Table 2: Regimen-specific factors and their coping strategies
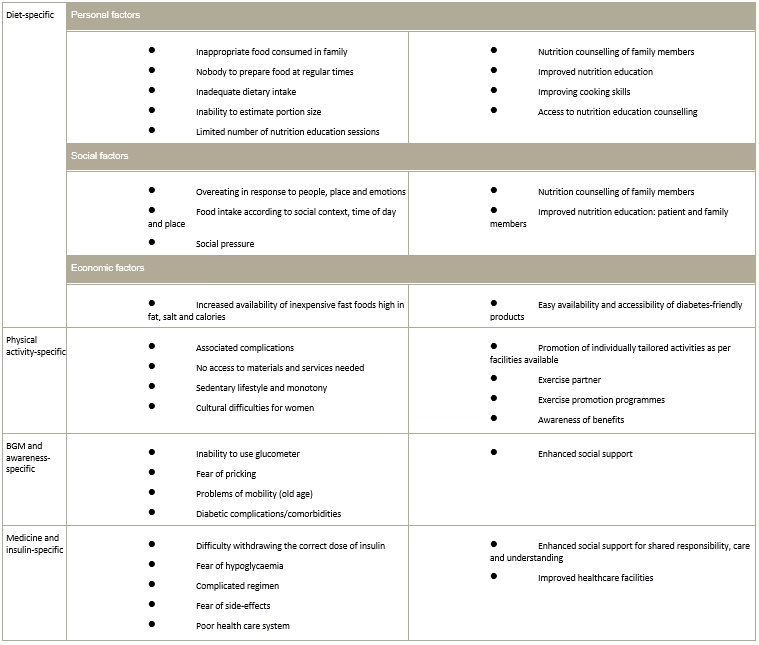
BGM = blood glucose monitoring
Diabetes control and festivals
In India, numerous festivals are celebrated irrespective of caste, creed, age, and status, with different rituals irrespective of their health implications. People with diabetes are faced with multiple challenges related to diet, physical activity pattern, healthcareseeking behaviour and healthcare provision during such occasions.5 Family or spousal compliance towards the glycaemic management of their affected relative is paramount. The patient can be supported through practices such as healthy eating, medical nutrition therapy, avoiding excessive outdoor meals and erratic meal patterns, selfcare practices, blood glucose monitoring, physical activity, medication administration, and management of acute complications may; all of which will enhance compliance for the effective management of diabetes during the cultural and religious occasions.50
Spousal participation in diabetes care plan
A collaborative project from the UK Department of Health and the Royal Pharmaceutical Society of Great Britain in the mid-1990s yielded a better understanding of the factors affecting compliance, which conceptualised the evolution of ‘‘concordance’’.48,49 With a shift from compliance to concordance in diabetes and its complications, spousal concordance is defined by researchers as “shared similarity of habits, behaviours and health statuses among the partners or spouses”.51,52
In this view, the concept of dyadic coping refers to the collective efforts of the partners to manage stress, develop problem-focused or emotion-focused strategies for better glycaemic control and improved quality of life together (Figure 2). It leads to the emergence of empirical and theoretical evidence of illness-specific spousal support in better health outcomes of chronic illness, with assumption of sustained effects with regards to the patient’s adherence to diet and exercise programmes. Spousal support is associated with better patient diabetes self-efficacy, both with regards to diet and exercise.53,54
Some of the explored factors with regards to better glycaemic control include age, family environment, emotional support, social status, positive relationship, shared expectations, motivation and responsibility, effective communication, sense of responsibility and common family eating patterns.55–57 A sense of coherence also seems to be established among older populations.58 Table 3 highlights the domains of spousal concordance in diabetes.44,54,57,59–64
A systematic review and meta-analysis conducted in 2014 has shown, with a pooled estimate, that partners have a 26% increased risk of developing diabetes which highlights the importance of collective efforts to optimise healthy eating and physical activity patterns.65 An article published by Wang et al., reported a significantly higher risk (5.19%, p<0.0001) of diabetes concordance in couples, associated with old age, middle levels of urbanisation, and high comorbidities (all p<0.05).66 A systematic review published in 2017 by Dimova et al. identified shared risk of diabetes among relatives of people with T2DM.62 It examined various randomised controlled trials to identify behaviour change strategies focussed on diet and physical activity to delay or prevent T2DM among the relatives or partners of people with T2DM to enhance effectiveness in their own health. It found sustained modifications in participant’s behaviour, which resulted in decreased daily calorie intake, increased physical activity, weight loss, decreased waist circumference and sagittal diameter, with significant correlations between the behaviour of patients and their partners.67
Only a few interventional studies have been conducted so far to explore the direct influence of partners of diabetic partners on lifestyle interventions for the improvement of adherence to the treatment (Table 4).68–70 Spousal involvement has been associated with improved support or care in chronic pain outcomes such as pain severity, pain behaviours and psychological distress.10,71 This may be especially relevant in patients with painful diabetic neuropathy or musculoskeletal complications of diabetes like frozen shoulder among others. Spousal participation can be a potential source of health-enhancing support (Figure 1).23,26,31,36,38,41,49,51,68
Table 3: Domains of spousal concordance in diabetes
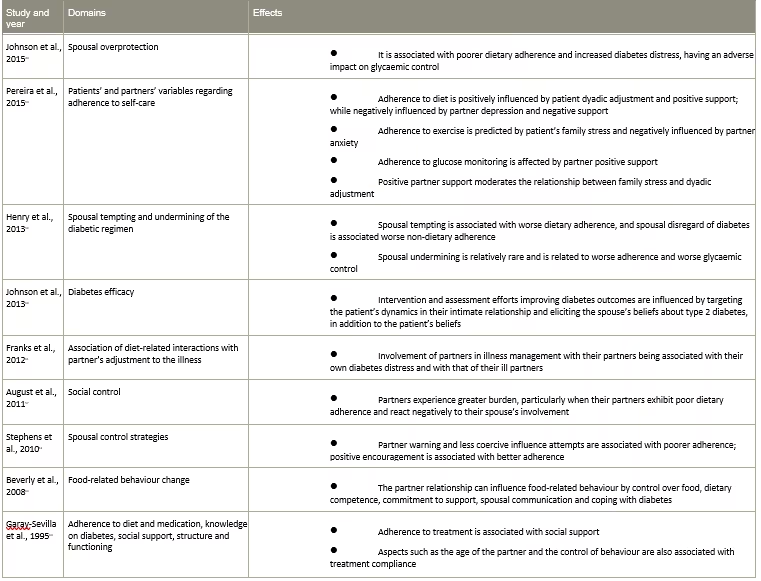
Table 4: Spousal interventional studies among people with diabetes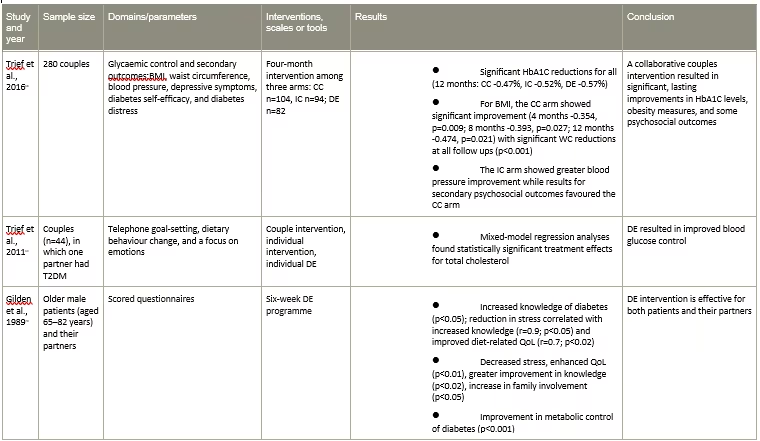
BMI = body mass index; CC = couples call; DE = diabetes education; HbA1C = glycated haemoglobin; IC = individual calls; QoL = quality of life; T2DM = type 2 diabetes mellitus; WC = waist circumference
Role of partner and family support – evidence from the clinical trials
The Look AHEAD (Action for Health in Diabetes) trial is the longest trial published, to date (8 years’ data), to evaluate the impact of intensive lifestyle interventions on weight loss, glycaemic control and cardiovascular outcomes in diabetes.72 Weight loss in Look AHEAD trial was -8.6% at 1-year follow-up and continued to be an impressive -4.7% at 8 years of follow-up.72 Unlike previous studies, the Look AHEAD trial did not involve intensive one-to-one sessions with dieticians/diabetes educators. Instead, in this study a group-counselling approach was used. A total of 19 group-counselling sessions took place over a period of 8 years where the patient and family members/ partners were given general advice on therapeutic lifestyle interventions.72,73 The study’s “toolbox” technique of group counselling, motivational interviews, improving self-image among family and friends was found to be highly effective. It was not only found to be cost effective, but also as efficacious in regards to weight loss and glycaemic control, which has been traditionally used in diabetes management.73 Hence the Look AHEAD study highlighted the importance of the positive impact of lifestyle changes in the entire family/community group rather than the individual alone.
The DiRECT (DIabetes REmission Clinical Trial) study has further highlighted the importance of weight loss in diabetes management.74 It demonstrated that in overweight and obese patients with T2DM of up to 6 years of disease duration and on multiple oral anti-diabetes medications, aggressive weight loss strategies with very low-calorie diet can result in remission of diabetes – defined as stoppage of all anti-diabetes medications and HbA1c <6.5% for at least 2 months.74 The greater the weight loss, the better were the chances of diabetes remission as evidenced by 7% remission with 0–5 kg weight loss, 34% remission with 5–10 kg loss, 57% remission with 10–15 kg loss, and 86% remission with >15 kg weight loss.74
Future implications
There is a paucity of data on the effects of spousal participation on health, glycaemic control, diabetes management and quality of life in lifestyle intervention studies and therefore more research is needed in this area. Further interventional studies evaluating the role of partner and family support in weight loss and diabetes management are urgently warranted.
Figure 2: Challenges in diabetes self-management and effect of social support
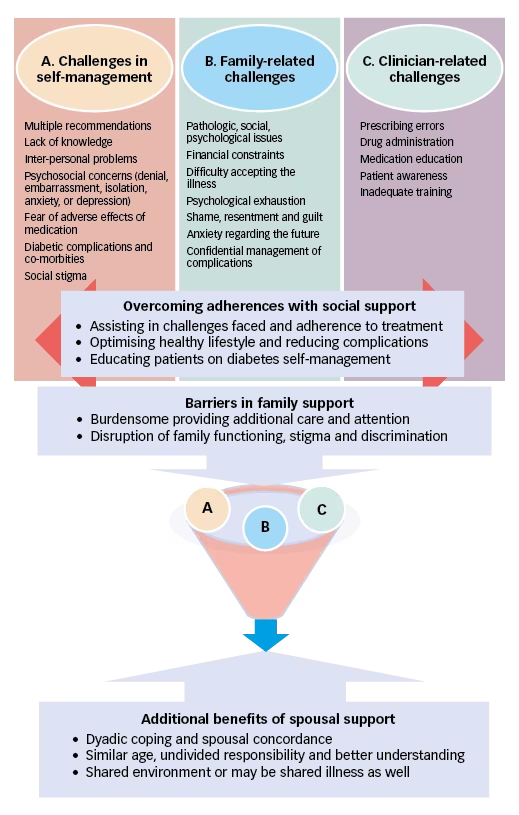
Conclusion
Social support from family members and spouses/partners is beneficial to improve adherence to the lifestyle interventions and diabetes self-management required to achieve optimum glycaemic control and prevent or delay associated complications. There is paucity of data regarding the mechanism behind such support. Clinical and research interventions should consider implementing dyadic educational (e.g. nutrition, exercise, medication adherence) and motivational skills training (e.g. problem solving, emotional expressiveness training) to facilitate and optimise spousal support resources.⬛







