The total number of people with diabetes worldwide is projected to double by 2030.1,2 Given the increasing prevalence of obesity, these fgures probably underestimate the future prevalence of diabetes. The risk for developing type 2 diabetes mellitus (T2DM) and premature cardiovascular disease are strongly linked to the metabolic syndrome, a condition characterized by excess central adiposity, elevated triglycerides, reduced high-density lipoprotein (HDL) cholesterol, hypertension, and impaired glucose tolerance.3
The total number of people with diabetes worldwide is projected to double by 2030.1,2 Given the increasing prevalence of obesity, these fgures probably underestimate the future prevalence of diabetes. The risk for developing type 2 diabetes mellitus (T2DM) and premature cardiovascular disease are strongly linked to the metabolic syndrome, a condition characterized by excess central adiposity, elevated triglycerides, reduced high-density lipoprotein (HDL) cholesterol, hypertension, and impaired glucose tolerance.3
A number of dietary factors have been implicated in the development and progression of this cardiometabolic phenotype. Chief among them have been sugars containing fructose: fructose, sucrose, and high-fructose corn syrup (HFCS). Since a temporal relationship was frst demonstrated between the increasing availability of HFCS and the prevalence of overweight and obesity in the US nearly a decade ago,4a fructose-centric view of cardiometabolic diseases has emerged. We aim to review the scientifc evidence supporting the role of fructose-containing sugars in the epidemics of diabetes and its related cardiometabolic complications.
Current Dietary Advice Regarding Sugar Intake
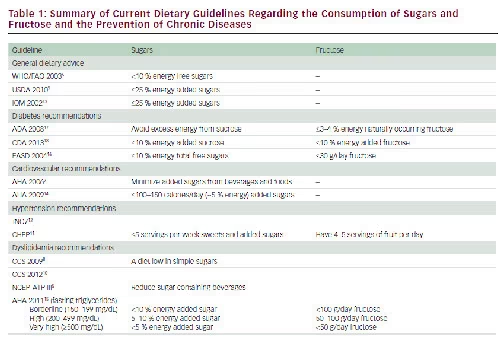
Various dietary guidelines have addressed sugars (see Table 1). Most have focused on the reduction of added fructose-containing sugars to maintain a healthy bodyweight.5–14 Recent American Heart Association lipid guidelines15 and international diabetes guidelines16–18 have singled out fructose by setting upper thresholds for fructose intake based on putative adverse lipid effects, although the American Diabetes Association acknowledges that fructose produces a lower postprandial glucose response when it replaces sucrose or starch in the diet.17 The guidelines implicate all fructose-containing sugars. There is now broad scientifc consensus that sucrose and most forms of HFCS are nutritionally and metabolically equivalent.19–21 Differences in the thresholds for harm set by the different guidelines, however, re”ect some uncertainty in the evidence on which the guidelines are based.
Dietary Sugar Sources/Typical Intake Patterns
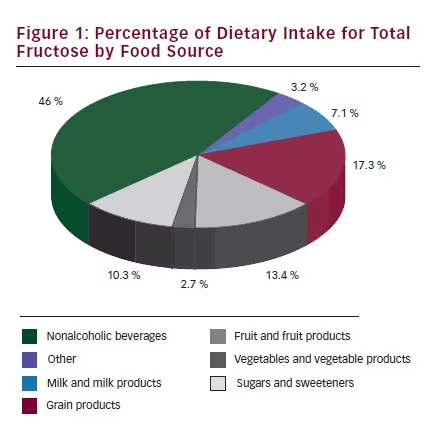
Sugars are found naturally in fruit and fruit products (fructose) and are added to foods mainly as sucrose (50 % bound fructose) or HFCS (42 % to 55 % free fructose) during preparation or processing to improve their palatability. HFCS is available at various fructose levels. HFCS 42, used in beverages, processed foods, cereals, and baked goods, comprises 42 % fructose and 53 % glucose. HFCS 90 comprises 90 % fructose and 10 % glucose. It is used in small quantities for specialized applications, but is primarily blended with HFCS to produce HFCS 55, which is used in soft drinks. The most important sources of fructose are nonalcoholic beverages (46 %) followed by grain products (17.3 %), and fruit and fruit products (13.4 %) (see Figure 1). The introduction of corn sweeteners in the early 1970s led to the progressive replacement of sucrose with HFCS in sugar-sweetened beverages (SSBs), so that the availability of sucrose (44 %) and HFCS (42 %) in the US market is roughly equal.22 The use of fruit sugar concentrate is also increasing.23
Although the availability of sugars has increased considerably over the last 50 years,24 total added sugar intake has begun to decrease over the last decade in the US. According to an analysis of the National Health and Nutrition Examination Survey (NHANES) III from 1999 to 2008 (n=42,316), the intake of added sugars in the US has decreased from 100.1 g/day (18.1 % energy) to 76.7 g/day (14.6 % energy), with a reduction in the intake of SSBs accounting for two-thirds of this reduction.25 The contribution of fructose to the diet has followed these trends. Total fructose intake is 49 g/day (9.1 % energy intake) at the 50th percentile and 87 g/day (14.6 % energy intake) at the 95th percentile.22 The highest intakes of fructose are among males 15–18y and 19–22y, each of whom consumes 75 g/day at the 50th percentile and 121 g/day and 134 g/ day, respectively, at the 95th percentile. On a per bodyweight basis, the highest intakes of fructose are in non-breast-fed infants and toddlers.22
Animal Models
The biologic plausibility supporting a link between fructose and cardiometabolic diseases arises from the unique metabolism of fructose. Fructose, unlike glucose, bypasses phophofructokinase, allowing it to enter glycolysis as an unregulated substrate for de novo lipogenesis (DNL) inducing a metabolic syndrome phenotype. The systemic effects of fructose-induced uric acid elevation mediated by intracellular adenosine triphosphate depletion may further modulate this phenotype.26 Fructose may also accelerate the development of obesity by uncoupling hormonal regulation of food intake through a lack of stimulation of insulin and leptin and impaired suppression of ghrelin.27 Animal models support these mechanisms. It is well established that excess fructose feeding in animal studies induces a metabolic syndrome phenotype with obesity, insulin resistance, hypertension, and dyslipidemia.28–31
The ability to extrapolate from animal models, however, is limited by supraphysiologic doses (%60 % of total energy intake), and the differences in carbohydrate metabolism between animals and humans. Whereas DNL can contribute >50 % of fatty acids in rodents, this proportion is much lower in humans.32 Two carefully conducted reviews of isotopic tracer studies in humans showed that <1 % of fructose is converted to triglycerides (DNL), while the conversion to glucose (~41 %), lactate (~28 %), and glycogen (>15 %) are much higher.33,34 These estimates, however, depend on the feeding state and will likely be higher under conditions of overfeeding and excess calories.35
Although a DNL-mediated mechanism of fructose may not be quantitatively signifcant in humans, there is evidence from experimental studies in humans to support a uric acid mediated mechanism36 and impaired satiety signaling involving insulin, leptin, and ghrelin.19,20 Whether these mechanisms will translate into downstream increases in obesity, diabetes, and cardiometabolic complications at population levels of exposure, however, remains unclear.
Ecologic Studies
Ecologic studies are frequently cited as the next line of evidence strongly supporting the link between sugars and cardiometabolic disease. This link has been extensively reviewed among various indigenous populations, in which the introduction of sugar has led to a transition from healthy individuals absent of chronic disease to a population with excessive rates of obesity and cardiometabolic diseases.26
A similar association has been shown in two recent ecologic analyses for the prevalence of type 2 diabetes. One study of 43 countries and the other of 175 countries showed a significant association with the availability of HFCS37 and total sugars,38 respectively. The prevalence of diabetes was 20 % higher in countries that use HFCS compared with countries that do not37 and increased by 1.1 % for every 150 kcal/ person/day increase in total sugar availability.38 Although these studies did attempt to control for some potential confounders, residual confounding cannot be ruled out, as a number of important confounders were not addressed. The estimates were also based on the pooling of heterogeneous measurements of exposure (both for the availability of HFCS or sugars and the potential confounders for which adjustments were made) and disease incidence.
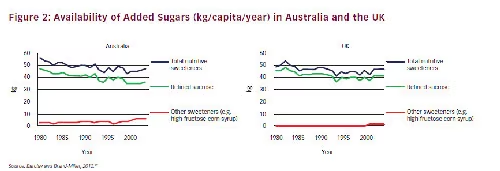
There are, however, some disparities in the ecologic data. From 1980 to 2003, total nutritive sweeteners declined 16 % in Australia (see Figure 2). Despite this decline, there was a threefold increase in the prevalence of obesity among adults and children, in line with other developed world populations. This fnding, was coined the ‘Australian Paradox’.39 The same paradox has been seen in the UK,39 the US, and Canada. Over the last decade, the reductions in the intake of total added sugars25 have not resulted in a decrease of obesity or diabetes in the US.40
These con”icting results highlight a limitation of ecologic studies of fructose. Even after adjustments, it can be diffcult to conclude whether the associations seen with fructose are caused by fructose, excess energy, or an interaction with other dietary and lifestyle factors associated with obesity and cardiometabolic risk. One reason may be the reliance on cross-sectional or passive inaccurate surveillance.41
In the case of the US, over the last decade, the reduction in added sugars has been accompanied by reciprocal increases in protein, fat, and other carbohydrates.25 These limitations open all ecologic analyses to ‘ecologic fallacy’ and reinforce the need to rely on higher-level evidence for drawing inferences.
Evidence from Prospective Cohort Studies
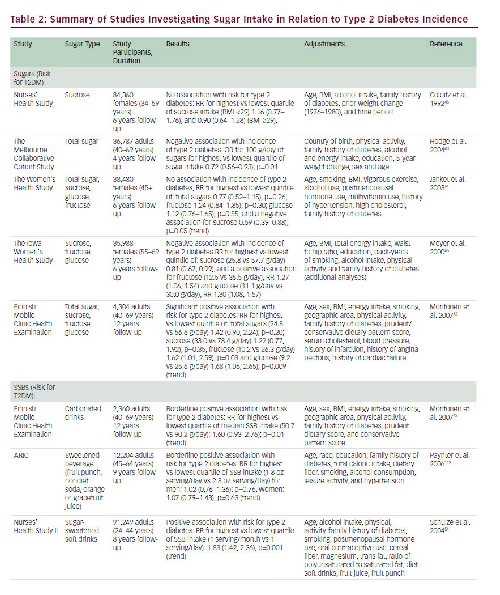
Among observational studies, prospective cohort studies offer the highest quality design. Several large prospective cohort studies have investigated sugars in relation to diabetes and other cardiometabolic outcomes (see Table 2). Results have differed based on whether sugars are measured as total sugars (fructose, sucrose, and or HFCS) or SSBs.
Total Sugars
Type 2 Diabetes Mellitus
None of the available cohort studies have found a signifcant positive association between total sugar and T2DM (see Table 2). The results have been equally inconclusive for the data regarding individual sugars.42–46
Other Cardiometabolic Outcomes
A similar lack of a consistent relation has been shown between total sucrose or fructose and other related cardiometabolic outcomes. No association has been shown with hypertension47 or coronary heart disease (CHD).48 Results have been mixed for gout.49–51 Under conditions where positive associations were seen, comparisons were between the highest and the lowest intakes of total fructose. There were no associations seen at levels of exposure equivalent to or below the 50th percentile for fructose intake in the US.22
Sugar-sweetened Beverages
Type 2 Diabetes Mellitus and the Metabolic Syndrome
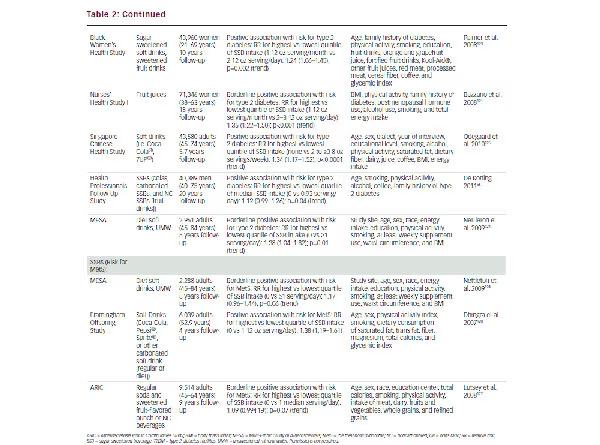
The prospective cohort evidence has more consistently shown an association with SSBs in relation to the metabolic syndrome and T2DM (see Table 2). A systematic review and meta-analysis of the available prospective cohort studies showed evidence of a signifcant association between SSBs and the risk for both T2DM and the metabolic syndrome, comparing the highest level of exposure with the lowest level of exposure of SSBs.52 There was, however, evidence of heterogeneity among the effect estimates. The reasons for this heterogeneity remain unexplained. One factor may relate to the small effect sizes and differing levels of exposure when comparing the highest with the lowest intakes. None of the studies showed signifcant associations at levels of exposure equivalent to or below the 50th percentile for added sugars or fructose intake in the US.22,25 The authors also preferred studies reporting energy unadjusted models providing the rationale that it is on the “causal pathway” between the exposure (SSBs) and the outcome (the metabolic syndrome or diabetes). Because energy is intrinsic to all caloric foods, this lack of adjustment complicates interpretation (especially where there may be important collinearity with other highly palatable caloric foods). Adjustments also differed among the studies for body mass index (BMI), family history of diabetes, smoking, physical activity, and various other dietary factors associated with the metabolic syndrome and diabetes.
Other Cardiometabolic Outcomes
The relationship with the metabolic syndrome and diabetes is supported by other prospective cohort studies that have shown a signifcant relation of SSBs with related cardiometabolic outcomes. A World Health Organization (WHO) commissioned systematic review and meta-analysis showed that SSBs increased the risk for overweight and obesity comparing the highest with the lowest intakes in children.53 Individually, large cohort studies have also shown increases in BMI54 and a higher risk for hypertension,55 gout,50 CHD,56 and stroke57 comparing the highest with lowest intakes of SSBs. As is the case for the metabolic syndrome and diabetes, these associations, however, have not been sustained at levels of intake equivalent to or below the 50th percentile for added sugars or fructose intake in the US.22,25 These associations do remain signifcant after adjustment for energy, although the effect estimates are smaller in these models. The one exception has been for BMI in children and adolescents.22,58
The reason for the different fndings when assessing the intake of total and individual sugars versus that of SSBs remains unclear. A lower satiety potential and inadequate compensation of energy from SSBs may lead to increased energy intake and weight gain with attendant cardiometabolic complications.52 On the other hand, the contribution of total sugar intake from nutrient dense fruits and vegetables as well as whole grain products, both of which have been associated with weight loss and improved metabolic outcomes in large prospective cohort studies59–61 and randomized dietary trials,62,63 may offset any adverse metabolic effects attributable to sugars. A more compelling reason may relate to collinearity between SSBs intake and various other lifestyle factors. For example, people who have high intakes of SSBs tend to eat more calories, exercise less, and smoke more,55 whereas the opposite is true for people with high intakes of total fructose.47 A high intake of SSBs is also associated with a high intake of red meat, processed meat, refned grains, French fries, sweets, and desserts, each of which have been shown to lead to weight gain60 and increase diabetes risk.61,64,65 Analyses that have taken advantage of this collinearity by combining these foods using dietary patterns analyses have shown that a Western dietary pattern characterized by the high intakes of these foods is more associated with weight gain and diabetes risk than SSBs alone even after adjustment for SSBs.66,67
Evidence from Controlled Dietary Trials
Sugar-related Interventions
Well-conducted dietary trials, controlling for both known and unknown confounders, provide the highest level of evidence for addressing the controversy of whether there are adverse effects of sugar intake. Careful inspection of these trials show contrasting effects between isocaloric trials, in which sugars are provided in isocaloric exchange for other macronutrients (energy-matched comparison) and hypercaloric trials, in which energy from sugars are added to or displaced from background diets compared with the background diets alone (a nonenergy matched comparison).
Glycemic Control
Isocaloric trials have not shown consistent evidence of differences between the effects of sugars and those of other macronutrients on glycemic control. A relatively large database of small trials exists of the effect of sucrose in isocaloric exchange for other carbohydrates on glycemic control. Only one shorter-term trial showed that high sucrose feeding (16 % total energy) raised day-long but not fasting blood glucose compared with low-sucrose feeding under energy-matched conditions in people with T2DM,68 while all remaining trials did not show signifcant effects on any indices of glycemic control for up to 52 weeks at large intakes up to 220 g/day in people with and without diabetes.69–77 Larger and longer trials have also failed to show consistent differences in glycemic effects between diets high and low in sugars in the CArbohydrate Ratio Management in European National diets (CARMEN) trial78 or between high and low carbohydrates (including sugars) in The Pounds Lost Trial.78–80
Few hypercaloric trials have assessed the effect of sugar on glycemic control. Two small feeding trials in people with diabetes and one larger trial in people without diabetes, in which diets were supplemented with small to moderate amounts of extra energy from sucrose (24 g/day to ~72 g/day) compared with a low-calorie sweetener, have failed to show adverse effects on glycemic control for up to 22 months.76,81,82 One trial, however, showed that overfeeding of carbohydrates, including sugars, sugar-sweetened foods, and beverages, at 50 % above energy requirements increased insulin without affecting fasting blood glucose compared with the baseline diet alone (without the excess energy) in lean and obese subjects at 2 weeks.83 These data suggest that a higher level of overfeeding may be required to provoke adverse glycemic effects. Nevertheless, it is unclear whether this isolated effect on insulin would have been true if this high level of overfeeding had been restricted to sucrose.
Other Cardiometabolic Risk Factors
Isocaloric trials, using energy-matched comparisons, have not shown any consistent evidence of an adverse effect of sugars in exchange for other macronutrients on a range of cardiometabolic risk factors. In overweight adolescents, a 1,500 kcal restricted snack diet containing calorie-free sodas achieved equal weight loss and changes in BMI as an isocaloric snack diet containing regular sodas.84 The CARMEN trial showed no differences in bodyweight, body fat, or blood lipids between the high-sugar diet and high-complex carbohydrate at 6 months.78 Similarly, no differences in bodyweight, fat, and ectopic fat distribution, changes were reported in The Pounds Lost Trial when comparing the higher carbohydrate diet (in which sugars were higher) with the lower carbohydrate diet (in which sugars were lower).79,80 Furthermore, isocaloric exchange of SSBs with milk showed no effect on bodyweight or body fat in a 4-month trial in children85 or 6-month trial in adults.86 The high intakes of SSBs (1 L/day providing 106 g/day sugars) in isocaloric exchange for milk, however, did increase ectopic liver, visceral fat, blood pressure, and triglycerides in the trial in adults.86 With few exceptions,68–70,87 smaller isocaloric trials of sucrose feeding up to 220 g/day have not shown signifcant differences in bodyweight, lipids, or any other cardiometabolic risk factors for up to 22 months in people with and without diabetes.71–76,88–91
A World Health Organization (WHO)-commissioned systematic review synthesized the available evidence in relation to bodyweight from the isocaloric trials published through December 2011. The conclusion was that sugars in isocaloric exchange with other sources of carbohydrate do not affect bodyweight.37 The same lack of a consistent effect would appear to apply to downstream metabolic complications. Further investigation, however, is required to understand the effect of SSBs in isocaloric exchange for milk on ectopic liver, visceral fat, blood pressure, and triglycerides.
In contrast with the results from isocaloric trials, adverse metabolic outcomes have been consistently reported in hypercaloric trials in which background diets are supplemented with sugar from SSBs providing excess energy at high doses. An earlier systematic review and meta-analysis of such trials, supplementing excess energy from SSBs compared with calorie-free control beverages, showed evidence of weight gain over 3 to 52 weeks of follow-up.92 The weight gain achieved, however, showed a linear dose response that was directly proportional to the degree of energy supplementation.90 A similar fnding was subsequently reported among children who had their diets supplemented with excess energy from SSBs (250 mL/day providing 104 Kcal/day) compared with calorie-free beverages for 18 months in the Double-blind, Randomized Intervention Study in Kids (DRINK).93 Smaller hypercaloric trials in which diets have been supplemented with sucrose in mixed forms (added to both solids and liquids) have shown mixed signals.76,81,82,94 Similarly, systematic reviews and meta-analyses90 and a subsequent large intervention trial95 have shown a weight decreasing effect of displacing energy from SSBs but only in some high-risk groups. In addition to a decrease in bodyweight, two small intervention trials of displacing energy from sucrose from usual intakes also showed decreases in triglycerides.73,77 Although another larger trial did not show a weight-decreasing effect of displacing energy from added sugars along with increasing dietary fber, it did show an improvement in insulin sensitivity over 16 weeks.96 When the available evidence from both the energy supplementation and displacement trials was synthesized in the most recent WHO-commissioned systematic review, the conclusion was that sugars are a determinant of bodyweight in so far as they supplement or displace energy in ad libitum diets.37 The same appears to apply to the observed downstream adverse metabolic effects.
In the absence of a macronutrient comparator supplementing or displacing the same amount of excess energy in the available hypercaloric trials, it is diffcult to disentangle whether the results are attributable to excess energy or sugar. In this regard, the overfeeding of carbohydrates (including sugars, sugar-sweetened foods, and beverages) compared with fats at 50 % above energy requirements resulted in similar weight gain.83 Displacement of energy from SSBs may also not offer any advantages over general weight loss strategies, as seen in the Choose Healthy Options Consciously Everyday (CHOICE) trial.97 These data support the idea that total energy is the critical component.
Taken together, the available trial data suggest a signal for harm when sugars and SSBs contribute excess energy to diets. The same has not been found to be true when sugars and SSBs replace starch, other macronutrients, or some snacks under energy-matched conditions. The one exception has been where large quantities of SSBs are provided in isocaloric substitution for milk. Further research is required to clarify whether sugars and SSBs have different effects than other commonly consumed sources of energy that are likely to replace them under free-living conditions.
Fructose Interventions
Several systematic reviews and meta-analyses, including a series (ClinicalTrials.gov identifer: NCT01363791) funded by the Canadian Institute of Health Research (CIHR), have been undertaken to investigate whether the consumption of fructose, as the main metabolic actor, predisposes individuals to weight gain and increase cardiometabolic risk, beyond that which would be expected with other sources of carbohydrate in controlled feeding trials. Collectively, these reviews have synthesized a large database of over 50 trials in over 1,000 participants. Consistent with the effect seen for sugar-related interventions, fructose has been shown to have differential effects in isocaloric and hypercaloric trials across a range of cardiometabolic endpoints.
Glycemic Control
In support of the early interest in fructose as an alternative sweetener in diabetes.73,98 isocaloric trials have provided evidence of a glycemic beneft of fructose (see Figure 3). A recent systematic review and meta-analysis of 18 controlled feeding trials in diabetes showed an improvement in long-term glycemic control when replacing an equal amount of other carbohydrate with fructose.99 At a median fructose dose of 60 g/day, which is near the mean intake in the general population,22 fructose in isocaloric exchange for other carbohydrates led to a clinically signifcant reduction in glycated hemoglobin (HbA1c) of ~0.53 %, a reduction equivalent to the lower limit of effcacy expected for oral hypoglycemic agents.99 These results confrm the results of an earlier meta-analysis of controlled feeding trials of the effect of fructose at intakes from 0 to %90 g/day in isocaloric exchange for other carbohydrates on HbA1c in people with and without diabetes.100
Similar glycemic advantages have been seen for fruit as an important source of fructose. A randomized controlled feeding trial showed that naturally occurring fructose from fruit at a dose equivalent to the median dose of fructose used across isocaloric feeding trials (~60 g/day) had a nonsignifcant tendency to decrease fasting blood glucose and signifcantly decreased bodyweight without adverse effects on lipids, blood pressure, uric acid, or insulin resistance compared with a low-fructose control diet under matched hypocaloric feeding conditions in overweight humans.62 Improvements in glycemic control seen in a RCT investigating the effect of a 6-month low glycemic index (GI) diet compared with a high-cereal fber diet in people with T2DM were also found to be attributable to low GI fruit as a source of small doses of fructose in T2DM.17,63 The improvements in glycemic control seen in this trial were nearly identical to those seen in a small systematic review and meta-analysis of six controlled feeding trials of fructose at a level (22.5–36 g/day) obtainable from fruit.101

The mechanisms by which fructose alone or as part of fruit may improve glycemic control is unclear. One explanation may relate to the ability of fructose to lower the GI of the diet.98 Another mechanism may relate to the ability of fructose to improve the metabolic handling of glucose derived from pure glucose and starch. An emerging body of evidence from elegant stable isotope and clamp studies in humans indicates that low-dose fructose may beneft glycemic control through a ‘catalytic’ mechanism, whereby fructose, through its metabolite fructose-1-P, increases the hepatic disposal of coingested glucose by increasing glucokinase activity.102,103 These effects have been shown to translate into decreases of ~15-30 % in the acute postprandial glycemic responses to coingested glucose and high-GI meals.104–106 This ability to lower the postprandial glycemic response to carbohydrate-rich meals may explain the reduction in HbA1c seen secondary to low-GI fruit in our recent RCT, as the low-GI fruit increase (2.2 servings/day) was equivalent to a ‘catalytic’ increase in fructose.63,107 A dose threshold for beneft, however, may lie above 10 g/day. Our systematic review and meta-analysis showed improvements in glycemic control at doses up to 100 g/day.99 There is currently insuffcient evidence to conclude that fructose benefts glycemic control. Fructose may only have beneft in so far as it does not contribute to a positive energy balance.
Other Cardiometabolic Risk Factors
A beneft of fructose on glycemic control must be weighed against its overall effects on cardiometabolic risk. Aggregate analyses of the available controlled feeding trials again show differences along the lines of isocaloric and hypercaloric trials (see Figure 3). Fructose in isocaloric exchange for other carbohydrates (even under positive energy balance or in fluid form) does not harm other cardiometabolic risk factors and even benefts blood pressure,108–110 the same is not true in hypercaloric trials. Aggregate analyses of hypercaloric trials show that diets supplemented with fructose providing excess energy (+18–97 % energy) at extreme doses (+104–250 g/day) well above the 95th percentile for intake in the population22 compared with the same diets alone (without the excess energy) increase bodyweight and uric acid,109,110 as well as fasting triglycerides, postprandial triglycerides, and markers of nonalcoholic fatty liver disease (NAFLD) (unpublished data). Formal tests of interaction suggest that these adverse cardiometabolic effects are more attributable to the excess energy than fructose. There was a subset of fve isocaloric trials included in our systematic reviews and meta-analyses111–116 that used excess energy diets (positive energy balance) in both the fructose and glucose comparison arms. If we restrict our meta-analyses to these trials, then there was no evidence of harm and even a possible blood pressure beneft. The suggestion is that diets supplemented with fructose providing excess energy do not differ from diets supplemented with excess energy from glucose as long as the comparison is matched for the excess energy. Two earlier meta-analyses, however, suggested possible high-dose thresholds for harm for the effect of fructose on fasting (>60 g/ day114 and >100 g/day97) and postprandial (>50 g/day97 triglycerides under energy-matched conditions.
Taken together, the available trial evidence suggests that moderate fructose levels of intake under energy neutral, weight-maintaining conditions does not have adverse effects on cardiometabolic risk factors with possible advantages for glycemic control and blood pressure. Low-GI fruit, as an important source of fructose, may have particular advantages under these conditions. A signal for harm does emerge when fructose is provided at high doses or contributes excess energy to diets. The increase in cardiometabolic risk factors provoked by fructose providing excess energy, however, does not differ from that seen with glucose providing excess energy, suggesting that excess energy is driving the observed effects.
Summary and Concluding Remarks
While there are data to suggest a role for sugars in the epidemic of diabetes, much of the current available evidence arises from lowquality observational studies, animal models, and overfeeding trials featuring high-intake levels. Prospective cohort studies have failed to show a consistent relation of fructose-containing sugars with weight gain or diabetes risk. Although signifcant associations have been shown comparing the highest with the lowest levels of intake of SSBs, these associations are small, do not hold at moderate levels of intake, and are subject to collinearity effects. SSBs may be a marker for an overall unfavorable Western dietary pattern and lifestyle. As many of the metabolic consequences of a diet high in fructose-containing sugars in humans can also be observed with high-fat or high-glucose feeding, it is possible that excess calories may be the main culprit in the development of the metabolic syndrome.118 Thus, it is important to distinguish between isocaloric trials in which fructose-containing sugars are exchanged isocalorically for other carbohydrates from hypercaloric trials in which fructose-containing sugars supplement diets providing excess energy at high doses. Systematic reviews and meta-analyses of the highest level of evidence from controlled feeding trials have not shown evidence of harm of fructose-containing sugars in isocaloric trials with possible advantages for glycemic control in the case of fructose interventions, especially where these interventions provide small doses of fructose at a level obtainable from fruit. Nevertheless, hypercaloric trials have consistently shown adverse effects, which appear more attributable to the excess energy than the fructose-containing sugars. Translation of these data is limited by the small sample sizes, short duration, and poor study quality of the available trials.
There remains a lack of consistent evidence to suggest that fructose, sucrose, or HFCS at moderate doses is directly related to the development of diabetes and other cardiometabolic diseases, although there is potentially cause for concern where fructose is provided at high doses or contributes excess energy to diets. Many questions remain unanswered. High-quality trials are needed to assess the role of fructose-containing sugars in free exchange with foods likely to replace them in the diet in the development of diabetes and cardiometabolic diseases.







