The global prevalence of obesity has increased tremendously in recent years. According to the World Health Organization, 39% of adults were overweight, of which 13% were obese, in 2016.1 The association between excess body weight and several medical conditions that increase morbidity and mortality is well-known.
Recent clinical evidence suggests that obesity is one of the most important risk factors for secondary hypogonadism in men.2–4 Although the actual prevalence of male obesity-related secondary hypogonadism (MOSH) is still unclear, large-scale epidemiological studies, and small population-based surveys suggest prevalence rates as high as 45.0–57.5%.4,5 This very high reported prevalence may be an overestimate of MOSH arising from several factors, such as inaccuracies in the methods used to estimate androgen level. It may also be the assessment of clinical features, such as erectile function and libido that can be associated with marked subjective variations in the study populations. Male hypogonadism has been shown to be associated with excess morbidity and mortality in multiple clinical studies.6–9 Therefore, we aim to discuss the pathophysiology, clinical aspects, diagnostic approach and management options for patients with MOSH in this comprehensive review.
Pathophysiology of male obesity-related secondary hypogonadism
Obesity and hypogonadism – bidirectional relationship
There is a bidirectional relationship between obesity and hypogonadism.10 In population-based studies, obesity is the single most important factor resulting in testosterone deficiency.11 Similarly, testosterone deficiency can cause increased adipogenesis and visceral obesity as evidenced by rapid weight gain observed in men following androgen deprivation therapy or surgical castration.12–14 Testosterone deficiency is associated with visceral fat dysfunction, subsequent chronic inflammation, insulin resistance and low sex hormone binding globulin (SHBG) levels.15,16 Weight loss achieved pharmacologically with liraglutide17 or with bariatric surgery improved testosterone and gonadotrophin levels, and were able to reverse the hypogonadotrophic hypogonadism caused by obesity.18–20
Metabolic syndrome and hypogonadism – bidirectional relationship
As is the case with obesity and hypogonadism, there is also a bidirectional relationship between metabolic syndrome and testosterone deficiency. Metabolic syndrome is associated with testosterone deficiency and low SHBG.21 The higher the number of metabolic syndrome components, the lower the testosterone levels will be.22 However, low free testosterone (FT) levels are not consistently associated with metabolic syndrome risk.21 Two recent studies in hypogonadal men, in which the association between total testosterone (TT) and metabolic syndrome were adjusted for SHBG, concluded that it is not total testosterone, but SHBG that is independently associated with metabolic syndrome risk.23,24
Hypogonadal–obesity hypothesis
Pathophysiological mechanisms for hypogonadism in obesity and for obesity in testosterone deficiency are complex and multifactorial. Individuals with MOSH exhibited a normal luteinising hormone (LH) and follicle stimulating hormone (FSH) response to gonadotropin releasing hormone (GnRH) indicating a hypothalamic defect rather than a pituitary defect.25 There is a bidirectional relationship between total testosterone level and amount of visceral adipose tissue, as proposed by Cohen in the hypogonadal–obesity hypothesis.26 Obese men with metabolic syndrome are at increased risk of developing testosterone deficiency.27
Hypogonadal–obesity–adipocytokine hypothesis
The hypogonadal–obesity–adipocytokine hypothesis is an extension of Cohen’s theory, which explains why the body cannot produce compensatory testosterone via increased gonadotrophin secretion and subsequent stimulation of the Leydig cells. In obese individuals, enhanced aromatase enzymes produced by adipose tissue reduce the testosterone and increase the oestrogen hormones. Testosterone deficiency facilitates further adipocyte differentiation, adipocyte inflammation and insulin resistance. The resultant increase in oestrogen, leptin, insulin and inflammatory cytokines result in hypothalamo–pituitary–testicular (HPT) axis suppression.28
Testosterone-oestradiol shunt
Obesity increases the expression of aromatase enzyme (CYP19A1) in the adipocytes, which enhances the conversion of androstenedione and testosterone to oestrone (E1) and oestradiol (E2) respectively. The resultant reduction in circulating testosterone level leads to further adipocyte hypertrophy and further worsening of testosterone deficiency.
The increased oestrogens formed from aromatisation causes a negative
feedback at hypothalamo-pituitary level, further lowering testosterone levels.28
Adipocyte hypertrophy and dysfunction
Lipoprotein lipase present on the extracellular surface of adipocytes hydrolyses circulating triglyceride-rich lipoproteins to free fatty acids which are taken up by the adipocytes and then esterified back into triglycerides for storage. Testosterone reduces the lipoprotein lipase activity in adipose tissue and inhibits the triglyceride storage. Testosterone deficiency is associated with enhanced triglyceride storage and subsequent increase in total body fat.28
Catecholamines are the major hormones controlling lipolysis in adipose tissue, acting via the adrenoreceptors. Testosterone upregulates the beta-adrenoreceptor number; activates adenyl cyclase to produce cyclic adenosine monophosphate which, in turn, stimulates hormone-sensitive lipase to accelerate lipolysis; and decreases total body fat mass.28
Androgen receptors are present in adipose tissue, the density of which is positively regulated by testosterone. Testosterone can decrease adipogenesis via a direct androgen-receptor-dependent mechanism. Incubation of isolated pluripotent stem cells with testosterone stimulated the development of cells of myogenic lineage rather than adipogenic lineage through an androgen-receptor-dependent mechanism, providing a molecular explanation for the decreases in fat mass and increases in lean mass observed after testosterone therapy.29
Proinflammatory cytokines
Testosterone exerts an anti-inflammatory effect as it prevents adipocyte hypertrophy and dysfunction. Testosterone and its aromatisation product, oestradiol, activate androgen receptors (AR) and estrogen receptors (ERα and ERβ) within the visceral adipose tissue, with a resultant decrease in the release of adipokines (leptin, tumor necrosis factor alpha [TNF-α], interleukin-6 [IL-6], osteoprotegerin, monocyte chemoattractant protein-1α) and increase in the release of adiponectin and visfatin. Testosterone improves insulin sensitivity and reduces the c-reactive protein from the liver.30 During testosterone deficiency, which is a proinflammatory state, the increased fat mass leads to adipocyte dysfunction, resulting in a decrease in adiponectin and an increase in adipokines such as leptin, IL-1, IL-6, and TNF-α secreted from both adipocytes and activated macrophages.31 These adipokines further worsen the inflammation and induce a state of systemic insulin resistance.32 Moreover, adipokines cause hypogonadism by impairing kisspeptin signalling to reduce GnRH secretion.33,34
Insulin resistance
Insulin resistance in testosterone deficiency is mediated by body composition dependent effects, including increased adipocyte differentiation (visceral obesity) and decreased myocyte differentiation (sarcopenia), and body composition independent effects such as increased inflammation (TNF-α, IL-1 and IL-6), decreased adiponectin and reduced mitochondrial function.35,36 Resultant hyperinsulinaemia acts on the kisspeptin neurons to decrease kisspeptin signalling, which, in turn, acts on the GnRH neurons to decrease GnRH release and thereby LH secretion.37
Leptin resistance
In normal physiological conditions, leptin acts through kisspeptin neurons to stimulate GnRH and thereby LH secretion.38 Testosterone suppresses leptin secretion from adipose tissue. In obesity induced adipocyte dysfunction, there is increased leptin release from adipocytes, which, in turn, causes a central leptin resistance at the hypothalamo-pituitary level. This decreases hypothalamic kisspeptin gene expression, which subsequently decreases GnRH and LH secretion and worsens testosterone deficiency.39,40 Moreover, leptin directly inhibits the stimulatory effects of gonadotrophins on the Leydig cells to further decrease testosterone secretion, via peripheral leptin resistance.41,42
Final common pathway of GnRH regulation
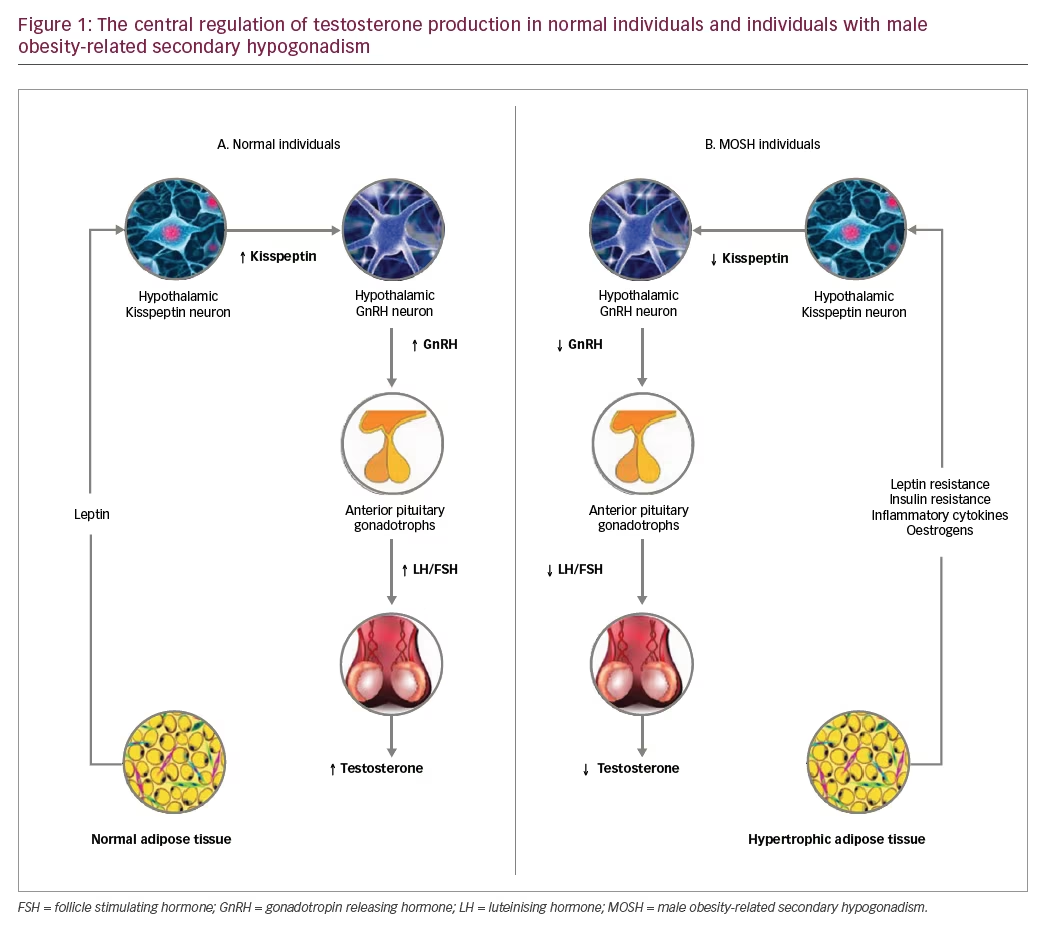
Kisspeptin neurons are located in the infundibular nucleus and GnRH neurons are situated in the preoptic area of the hypothalamus.37 Kisspeptin regulates the HPT-axis by stimulation of its receptor on GnRH neurons, thereby regulating LH and FSH secretion.43 GnRH neurons express kisspeptin receptors (KISS1R), but do not express receptors for leptin and insulin, whereas kisspeptin neurons have receptors for leptin, insulin and oestrogen.38,40,44 The central regulation of testosterone production in normal individuals is shown in Figure 1A and that in MOSH is shown in Figure 1B.
Metabolic endotoxaemia
The human gut contains more than 100 trillion bacteria and approximately 70% of these are gram negative, containing lipopolysaccharide.45 Normally these bacterial endotoxins are prevented from entering circulation by the intestinal mucosal barrier. A recently proposed GELDING (Gut Endotoxin Leading to a Decline IN Gonadal function) theory suggests that high-calorie, high-fat diet breaks down integrity of this mucosal barrier and results in metabolic endotoxaemia, a pro-inflammatory state, and consequential hypogonadism.45
Obesity and sex hormone binding globulin
Most of the SHBG in circulation is produced in the liver. Low SHBG levels seen in obesity is caused by the high lipid content of the liver and by high pro-inflammatory cytokines (TNF-α and IL-1) rather than by hyperinsulinaemia (insulin resistance) as was previously thought.46 Though SHBG functions primarily as a transporter of sex steroids, it has additional actions. SHBG has anti-inflammatory effects. It decreases fat content in macrophages and adipocytes and suppresses inflammation. Low SHBG can be the result of insulin resistance.47
Obstructive sleep apnoea and hypogonadism
There is a bidirectional relationship between testosterone deficiency and obstructive sleep apnoea (OSA). Patients with OSA have reduced rapid eye movement (REM) sleep duration, reduced deep sleep duration, and reduced sleep efficiency associated with increased night-time awakenings, sleep fragmentation and nocturnal hypoxia, all of which leads to a low testosterone level. Similarly, low testosterone promotes obesity, decreases REM sleep and deep sleep, thus negatively affecting sleep quality.48
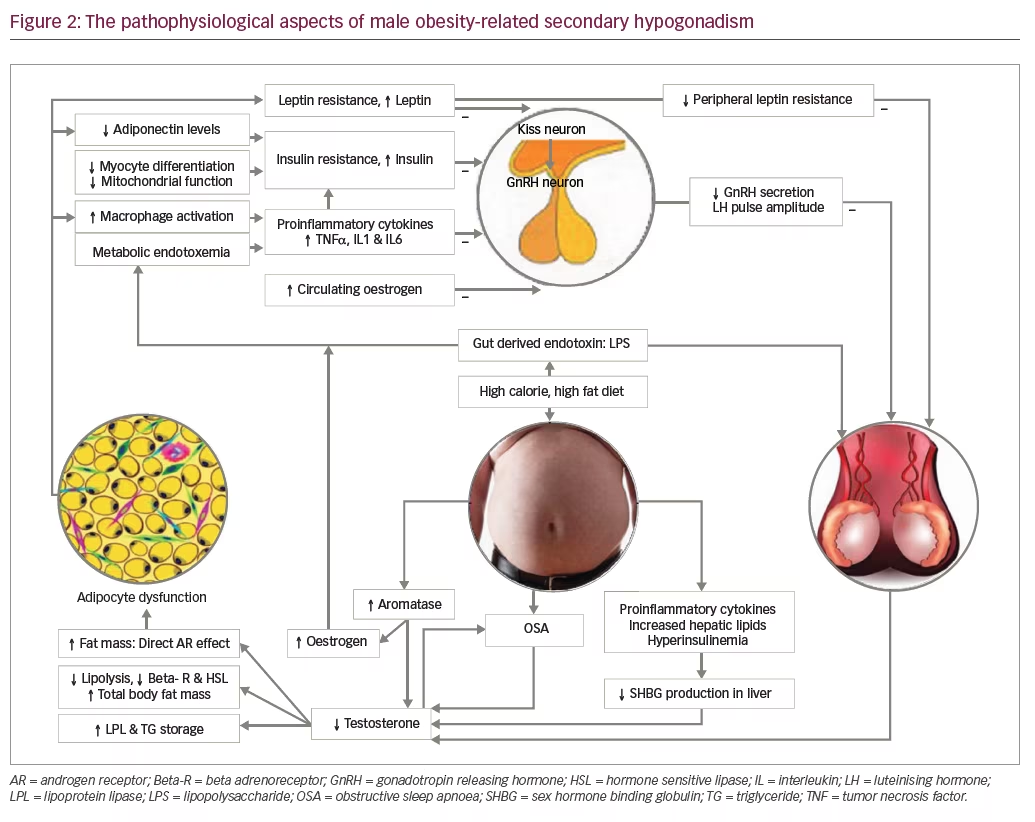
The pathophysiological aspects of MOSH are summarised in Figure 2.
Clinical presentation
Men with functional hypogonadism commonly present with non-specific symptoms and modestly low testosterone levels. In the European Male Ageing Study (EMAS), only three out of 32 sexual symptoms were syndromically associated with testosterone deficiency. 49 Only 0.6% of healthy men or 0.4% of lean men developed functional hypogonadism which implies that functional hypogonadism usually develops in obese men with comorbidities.
Diagnostic approach
MOSH can be diagnosed when all of the following features are present:2
1. Obese male with body mass index (BMI) of ≥30 kg/m2.
2. Clinical hypogonadism: impaired sexual, physical or mental performance, impaired sexual characteristics, gynaecomastia, breast pain, sleep problems, dysglycaemia, flushing, low bone mineral density (BMD) or unexplained anaemia.
3. Biochemical hypogonadism: morning TT less than the lower limit for healthy young men as measured using a reliable assay, confirmed twice, or in the presence of abnormal SHBG, FT or bioavailable testosterone less than lower limit for healthy young men in a reliable assay.
4. Secondary hypogonadism: low or inappropriately normal LH or FSH.
5. Functional hypogonadism: other causes of hypogonadism excluded systematically.
Diagnostic recommendations based on British Society for Sexual Medicine guidelines are shown in Table 1.50
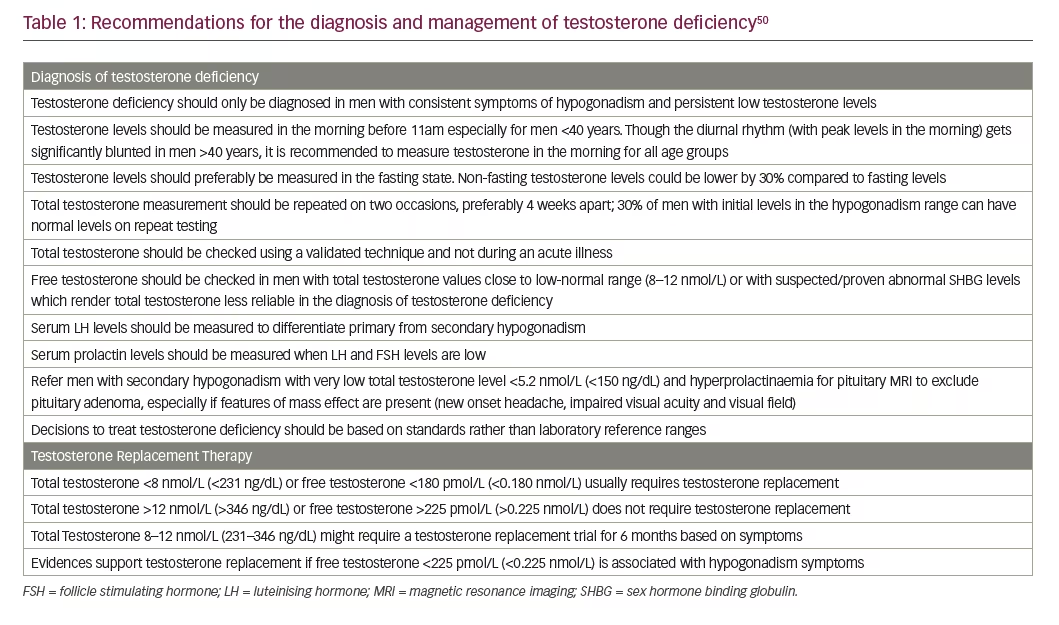
Management options
Weight loss achieved using healthy lifestyle changes
MOSH is a potentially reversible cause of HPT axis suppression and testosterone deficiency (functional hypogonadism) and hence can be managed with lifestyle measures to achieve significant weight loss, without the need for testosterone treatment.51 Longitudinal data from the EMAS showed that weight loss can increase testosterone levels in obese men. Over a period of 4.4 years, minor weight loss (<15%) was associated with a modest increase in TT levels (2 nmol/L or 58 ng/dL) and increases in SHBG (due to improvement in insulin resistance). However, there was no increase in FT levels with this degree of weight loss. Weight loss greater than 15% was associated with more marked increases in TT (5.7 nmol/L or 164 ng/dL) and FT (52 pmol/L or 52 pg/mL). The rise in testosterone level is proportional to the extent of weight loss achieved.52
Weight loss achieved by lifestyle modification can improve erectile dysfunction as measured by International Index of Erectile Function (IIEF). A randomised controlled trial (RCT) in relatively healthy obese men without diabetes, hypertension and dyslipidaemia showed that intensive lifestyle modification achieved a 15% weight loss and improved IIEF score by 3.1.53 A meta-analysis of four RCTs on obese men with cardiovascular risk factors demonstrated that lifestyle modification along with pharmacological treatment of cardiovascular risk factors resulted in an IIEF score improvement of 2.66.54 The Look AHEAD trial, which evaluated the effect of weight loss in older overweight/obese diabetic men, found that IIEF improved only by 1.3, probably due to increased frequency of irreversible neurovascular disease.55
Diet alone
A recent study in patients with MOSH concluded that customised diet therapy with low-calorie, high-protein diet with personalised dietary counselling, and physical activity can induce positive changes in hormonal profile and body composition by increasing testosterone levels, decreasing oestradiol levels and by reducing the total fat mass.56Improvements in dietary pattern (less eating out, minimal dairy products and desserts, enhanced consumption of dark green vegetables etc.) may help to prevent obesity associated testosterone deficiency.57
Exercise alone
Exercise can increase LH and testosterone production (via anti-inflammatory effects on the hypothalamus and testes), and can recover erectile function in patients with MOSH.58 Aerobic exercises do improve testosterone levels whereas resistance exercises do not have a significant effect.59,60 Moreover, in patients on testosterone replacement therapy (TRT), exercise can augment the effects of TRT and the durability of response after cessation of TRT.61 Testosterone deficiency in obese men is associated with reduced physical activity, sarcopenia, decreased BMD and visceral obesity.62 Moderate aerobic exercise has been found to reverse all these parameters, reduce body weight by 5.9 kg and improve IIEF score by 2.6.62,63 Hence it is recommended that obese physically inactive men with multiple cardiovascular risk factors should undertake supervised physical training that consists of 40 minutes of moderate-to-vigorous intensity aerobic exercise, at least 4 times per week. In general, weekly exercise of 160 minutes for 6 months can improve erectile function in obese physically inactive men.64
Weight loss by treatment with liraglutide
Glucagon like peptide-1 (GLP-1) receptor agonist, liraglutide, is approved as an adjunct in weight management, alongside dietary measures and increased physical activity, in individuals with a BMI ≥30 kg/m2 or in individuals with a BMI ≥27 kg/m2 and comorbidities such as type 2 diabetes mellitus (T2DM). A recent prospective randomised study comparing liraglutide and TRT in obese hypogonadal men, found that liraglutide treatment resulted in a significant increase of LH and FSH along with an average weight loss of 7.9 ± 3.8 kg compared with a 0.9 ± 4.5 kg loss with TRT (p<0.001).65 Recovery of metabolic syndrome was observed in two patients on liraglutide whereas no subjects recovered from metabolic syndrome while on TRT. The study concluded that following failure of lifestyle modification, liraglutide is superior to TRT in men with obesity associated functional hypogonadism.
Weight loss with bariatric surgery
Though both lifestyle modification and bariatric surgery can achieve weight loss with a resultant rise in TT and FT levels, bariatric surgery is more effective in achieving weight loss than a low-calorie diet. Lifestyle modification resulted in a mean weight loss of 9.8% with an increase in TT of 2.87 nmol/L (84 ng/dL) whereas bariatric surgery achieved a mean weight loss of 32% with an increase in TT of 8.73 (251 ng/dL).66 The rise in TT was greater in younger, non-diabetic subjects with higher baseline BMI, and in subjects who had lost the most weight. The best determinant of testosterone rise was the degree of weight loss. Weight loss was also associated with a rise in gonadotropin and fall in oestradiol levels.66
A recent study that directly compared laparoscopic gastric bypass (LGB) to restrictive bariatric surgical procedures in terms of testosterone level improvement found that both procedures are equally effective in achieving remission of MOSH.67 TT and SHBG levels increase soon after bariatric surgery, at 1 month (due to improvements in insulin resistance), whereas FT levels do not increase until 6 months after bariatric surgery. Consequently, the improvements in symptoms of hypogonadism will only be observed after 6 months following surgery.68
Weight loss achieved by bariatric surgery is associated with improvements in sexual function and quality of life. In a recent meta-analysis, obese men who underwent bariatric surgery exhibited an increase in IIEF-5 score of 4.1–5.66.69 The improvement in sexual function after bariatric surgery not only depends on testosterone levels, but also on degree of weight loss, the psychological impact of improved body image and baseline erectile function.70
Testosterone replacement therapy
Obese men with secondary hypogonadism achieved a statistically significant reduction in fat mass (3.5 kg, p=0.03), increase in lean body mass (2.9 kg, p=0.03) and glycated haemoglobin (HbA1c) improvement (9 mmol/mol, p=0.03), associated with 52% improvement in beta-cell function with TRT.71 Treatment also resulted in an overall improvement in metabolic state, including improvements in the following parameters: BMI, waist circumference, lipid profile, blood pressure, lipoprotein (a), haemoglobin, fasting glycaemia, insulin resistance and leptin resistance.72–78 TRT also reduced arterial stiffness, respiratory quotient, hepatic fat content and bone remodelling.79,80 TRT mediated and psychotropic effects included improved energy and motivation.81
Weight loss associated with TRT was almost exclusively due to loss of fat mass, whereas the weight loss due to dieting is from loss of both fat mass and lean mass. Although TRT did not augment diet-induced loss of fat mass, it prevented diet-induced loss of muscle mass.82 These favourable effects of TRT on body composition may be due to androgen receptor signalling in adipocytes and myocytes and/or increased physical activity seen in testosterone replaced men. However, successful visceral fat loss achieved by testosterone therapy is not maintained after cessation of TRT, as low testosterone (after TRT withdrawal) may lead to fatigue and inertia and less physical activity.83,84 This suggests that long term TRT is required to maintain the beneficial effects.
In obese healthy men with mild-to-moderate androgen deficiency symptoms and moderate testosterone deficiency, the improvement in androgen deficiency symptoms achieved with TRT is over and above what is achieved with weight loss alone, with the greatest benefits observed in severely symptomatic men.85 A recent meta-analysis found that TRT significantly improves erectile dysfunction in men with testosterone deficiency and improves the mean IIEF-5 scores by 1.47 and 2.95 for men with baseline testosterone levels of <12 nmol/l and <8 nmol/l, respectively.86
In obese hypogonadal men, irrespective of the class of obesity, TRT is effective in achieving and maintaining weight loss.87 Hypogonadal men on long-acting intramuscular testosterone undecanoate achieved 5% weight loss in 1 year and 13% weight loss in 5 years.88 Two meta-analyses of five and eight RCTs concluded that TRT can significantly improve glycaemic control along with a reduction in triglycerides in type 2 diabetic hypogonadal men.89,90 However, a third meta-analysis of seven RCTs failed to demonstrate any significant improvement in glycaemic control, which implies that TRT does not have a consistent effect on HbA1c.91
Due to conflicting evidences relating TRT to cardiovascular disease (CVD) and mortality, the US Food and Drug Administration has warned that TRT might increase heart attack and stroke. A critical review of all the published systematic reviews found that two out of six systematic reviews and meta-analyses showed increased CVD risk with TRT.92However, recent reviews shows that there is a trend towards reduced major adverse cardiac events, all cause and cardiovascular mortality with TRT, with the greatest benefit seen in men at highest risk of CVD, such as those with T2DM and metabolic syndrome.93 Moreover, greater benefits are observed among those treated to the target and for longer duration.94 A recently published population-based observational study showed that longer duration TRT is associated with decreased mortality, CVD events and prostate cancer, whereas shorter duration TRT increased mortality and CVD events.95
Selective oestrogen receptor modulators
TRT can cause suppression of spermatogenesis and testicular atrophy and is not the best option for young men with hypogonadism who desire fertility preservation. Clomiphene citrate is a selective oestrogen receptor modulator which is effective in stimulating the HPT axis and normalising the hormonal profile without causing testicular atrophy. A recent study evaluating the effect of clomiphene citrate in adult men with MOSH found an improvement of hypogonadal symptoms (associated with increases in TT, FT, LH, FSH, and SHBG) and improvements in lean mass, fat-free mass, and muscle mass in the clomiphene treated cohort. Investigators concluded that clomiphene citrate may be used as an alternative treatment for MOSH in adult men.96 However, selective oestrogen receptor modulators may reduce insulin-like growth factor-1 (IGF-1) levels with a resultant reduction in anabolism, and an increase in SHBG levels that reduce testosterone bioavailability.97
Aromatase inhibitors
In elderly obese men with hypogonadism, administration of anastrozole, an oral aromatase inhibitor, increased androgen levels and decreased oestradiol levels but without any improvement in body composition, strength or lipid levels.98 Despite a significant rise in testosterone levels, the use of an aromatase inhibitor is not associated with any somatic or psychological effects in obese men with hypogonadism and is associated with worsening of spinal BMD.99,100 Due to the worsening of BMD and lack of body composition improvement, aromatase inhibitors are not an ideal alternative to TRT in obese hypogonadal men.
When to consider organic hypothalamo–pituitary–testicular axis suppression in an
obese male
Young healthy men, without comorbidities, with typical androgen deficiency symptoms and unequivocally low testosterone should be considered to have organic hypogonadism. In men with suspected MOSH, lifestyle modification, including weight reduction, optimal treatment of diabetes and other comorbidities, should comprise first-line treatment of the condition. If these measures fail to normalise the androgen deficiency symptoms and/or low testosterone levels, despite successful weight loss, clinicians should repeat evaluations to rule out organic HPT axis suppression.101 Once this has been ruled out, a therapeutic trial of TRT can be considered in those with severe androgen deficiency symptoms and unequivocally low testosterone levels, unless contraindicated.
Areas of uncertainty
Effect of testosterone on HbA1c
TRT does not consistently affect HbA1c in obese men with diabetes.89–91 It is possible that increased erythropoiesis, which occurs as a side effect of TRT, may affect HbA1c independently of changes in glycaemia. Hence, studies with careful analysis of self-monitored blood glucose data and alternative measures of glycaemia other than HbA1c should be designed to evaluate the effect of testosterone on HbA1c.
Effect of testosterone on subcutaneous adipose tissue and visceral adipose tissue
Visceral adipose tissue is more strongly linked to insulin resistance than subcutaneous adipose tissue is. Though various RCTs have consistently proved that TRT can reduce total body fat mass,77,82–83,102–103 its effects on regional fat redistribution are not consistently proven; some studies have shown a reduction in visceral adipose tissue103–104whereas others have not.79,102,105 These inconsistencies may be due to small sample sizes or imprecise methodology to quantify visceral adipose tissue like dual-energy X-ray absorptiometry or ultrasound.
Indications for testosterone replacement therapy in male obesity-related secondary hypogonadism
Testosterone therapy should only be prescribed for those with clinically significant symptoms with persistently low testosterone levels. TRT should not be routinely prescribed to men with functional hypogonadism, including MOSH, and low–normal testosterone until clinical benefit is confirmed by well-powered clinical trials.
Testosterone replacement therapy and cardiovascular disease risk
Earlier studies suggested that TRT might increase CVD risk.92 However, many recent studies showed reduced CVD risk and all-cause mortality with TRT in hypogonadal men with long term treatment.93–94 This safety matter requires further investigation in large-scale prospective RCTs that focus on the cardiovascular benefits and risks associated with TRT.
Summary and conclusions
With the increasing prevalence of obesity, the incidence of MOSH is also increasing.106 Lifestyle modification remains the first-line management of MOSH as this improves the overall health of the patient and has the potential to improve androgen deficiency symptoms irrespective of any effect on testosterone levels. In selected patients with clinical indications, weight loss interventions such as bariatric surgery can revert the hypogonadotrophic hypogonadism caused by obesity. If these measures fail to relieve symptoms and to normalise testosterone levels, in appropriately selected men, TRT could be started. Other medications such as aromatase inhibitors and selective oestrogen receptor modulators are not recommended due to lack of clinical trial-based evidence.