The growing prevalence of obesity is a global health concern. In 2009 to 2010, more than one-third of adults and 17 % of youth in the US were obese, as defined by body mass index (BMI). Obesity is associated with numerous health risks such as hypertension,1 cardiovascular disease (CVD),2 diabetes,3,4 stroke,5 and various cancers.6 Obesity also has a considerable impact on health-related quality of life (QoL).7 Of greatest concern is the early onset of obesity compared with previous generations. This has led to a predicted growth in the proportion of the population living with obesity-related diseases and chronic disabilities, which may reverse the trend toward increased life expectancy achieved during the past century.8 The economic costs of these obese populations living with chronic diseases will be dramatically higher than the normal-weight population.9,10 Clinical evidence suggests that weight reduction can improve outcomes in obese patients. Modest weight loss (2.6–4.9 kg) is associated with improvements in weightrelated comorbidities.11–13 Higher levels of weight loss have been associated with greater benefits.14 While any intervention to combat obesity should focus on lifestyle interventions, in particular increasing physical activity, health care systems could achieve substantial cost savings through supplementing such interventions with anti-obesity medications that promote weight loss.
A growing consensus agrees that the main factors underlying the obesity epidemic are a rise in urbanization and globalization, which have led to substantial changes in the number and types of food-related cues, food availability and portion sizes, the availability of food at all hours of the day, and sophisticated marketing techniques. In the past it was believed that obesity prevention and treatment was a matter of self-control. This would imply that society has collectively lost its self-control in the last 30 years, in parallel with the rise in obesity, and that North Americans, in whom obesity levels are highest, have reduced self-control. However, this seems an unlikely explanation. The increase in obesity is seen across all socioeconomic groups, including those with high levels of education enabling the ability to make informed choices.15 The neurophysiologic mechanisms influencing food intake may therefore be operating below the level of individual awareness.16
The field of obesity medicine is changing rapidly and health care professionals have multiple weight loss medications to choose from, with more under development. It will become important to understand how each medication affects food intake and eventual weight management. This article will discuss the multiple neurophysiologic pathways underlying obesity, and describe a new pharmacologic strategy that targets the homeostatic pathways and reward pathways
associated with food intake.
Neurophysiologic Regulation of Obesity
Control over food intake is essential for weight management and represents an important aim of anti-obesity therapy. The homeostatic mechanisms responsible for energy intake and expenditure are largely regulated by the central nervous system, which integrates signals from the gastrointestinal system, adipose tissue, liver, muscle, and pancreas. This information, together with a number of higher brain centers, regulates weight.17
A major regulatory region of the brain involved in body weight homeostasis is the hypothalamus. When humans feed, peripheral signals are sent to the hypothalamus to stop eating for several hours. These signals act on a number of neurons, including the anorexigenic pro-opiomelanocortin (POMC) neurons in the arcuate nucleus of the hypothalamus. Stimulation of POMC neurons results in increased release of several hormones including a-melanocyte-stimulating hormone (a-MSH), which signals the brain to stop eating and increase energy expenditure.18 Interestingly, b-endorphin is co-secreted with a-MSH from POMC17 and provides an autoinhibitory feedback mechanism to inhibit further POMC activation. In other words, at the same time that the central control part of the brain is telling the body to stop eating and increase energy expenditure, it is also ensuring that this message is transient, in order that the body does not stop eating for too long and returns to conserving energy (presumably an adaptive survival response). The combination of these actions in part regulates energy balance, and this regulation can be altered with weight change.17,19 This is an example of the complex physiologic mechanisms regulating food intake and may explain why single drugs with single mechanisms of action within a pharmacologic treatment may in some cases not provide as much weight loss as combination treatment approaches that combine multiple mechanisms of action.
The caloric and nutritional values of food are not the only factors affecting food intake; food is associated with intrinsic reward value and the hedonic and emotional aspects of eating are of increasing importance in our obesigenic environment. It is now known that the hedonic control of food intake can override metabolic and homeostatic signals of satiety,20,21 which can result in overconsumption. Excessive food consumption will take place with food cravings and a loss of control over food intake despite awareness of its negative consequences.22 The availability of highly palatable and rewarding (i.e. fat, sweet) food can significantly affect homeostatic balance, resulting in dysregulated food intake. The behavioral aspects of eating and obesity are currently the subjects of active clinical research.
An important regulator of hedonic eating behavior is the mesolimbic dopamine system, or reward system. The ventral tegmental area, a group of neurons located in the midbrain, is the origin of mesolimbic dopamine pathways. These release dopamine, which affects a number of brain regions including the ventral striatum, nucleus accumbens, prefrontal cortex, and amygdala.23,24 Dopamine signaling is implicated in the ‘wanting’ or desire of certain foods, which underlie food craving.23 The pleasurable feeling (‘liking’) associated with rewarding stimuli is governed by opioid signaling.25,26 Opioid compounds, particularly those selective for the m-opioid receptor within the nucleus accumbens and surrounding ventral striatum,
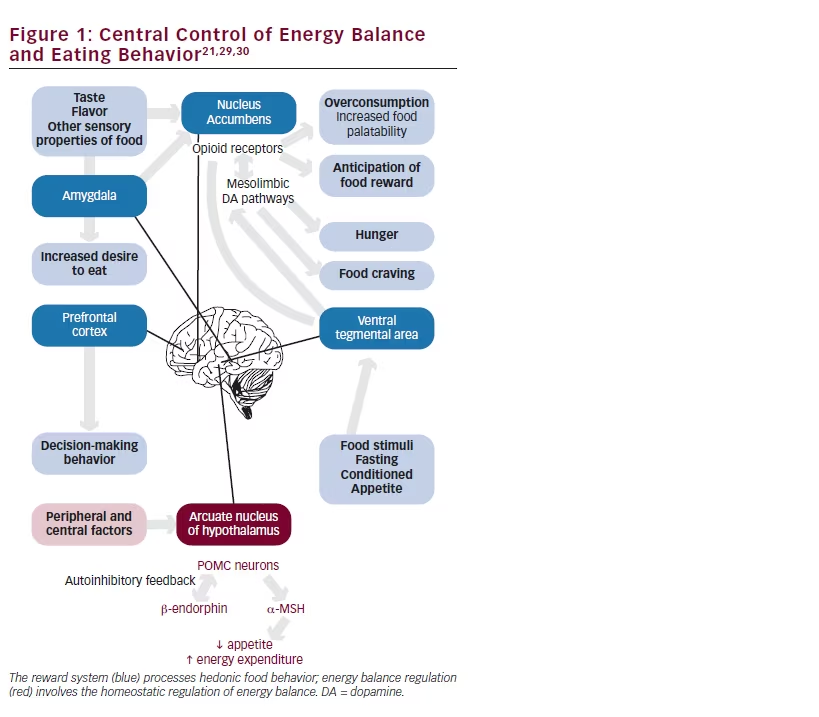
induce a potent increase in food intake.27 Opiate stimulation of orexin signaling in the ventral tegmental area has been associated with increased consumption of palatable foods.28 Brain regions known to be responsible for addiction have been associated with eating behavior. The amygdala is linked to the olfactory signaling system and can influence appetite. The complex interplay of these factors is illustrated in Figure 1.21,29,30
Genetic variability in the neurophysiology of the reward system may explain why some individuals are more susceptible than others to weight gain.31,32 Obese individuals are known to demonstrate different neural responses in response to food cues,33–36 including impairments in dopaminergic pathways.37 Visual stimulation with food cues activates regions related to reward anticipation and habit learning in the dorsal striatum. It has been shown that individuals who are obese will have an increased activation of these regions in the brain to highcalorie food images. This results in BMI-dependent activation in regions related to taste, motivation, emotion, and memory, and this activation is independent of levels of hunger and satiation.38–40 Differences in these neural regions in obese individuals have been associated with higher levels of food craving and dysregulated eating behaviors,37,41 and may influence food choice and consumption.42 These changes may also underlie delayed satiation, reduced perception of caloric intake and increase in hunger in obese individuals following a 10 % weight loss. Therefore, treatments that affect neural responses to food and food-seeking motivations such as craving may represent a novel approach in designing interventions to treat obesity.

Sustained-release Naltrexone/Bupropion— A Novel Pharmacologic Approach to the Treatment of Food Craving and Obesity
History of Use and Mechanism of Action
Combination therapies are an attractive option for pathologic states resulting from multiple regulatory mechanisms. The combination of naltrexone and bupropion (NB) in a sustained-release formulation is a novel therapeutic approach to obesity, whose effects may in part be mediated by a unique effect on reward pathways, resulting in sustained appetite reduction and enhanced control of eating behavior.43 The individual components of NB have been used independently for decades to treat a variety of disorders. Naltrexone is an opioid antagonist that has been used clinically in the treatment of opioid and alcohol dependence.44 Bupropion is a dopamine and norepinephrine re-uptake inhibitor that has been used to treat nicotine dependence, depression, and seasonal affective disorder.45
Bupropion has been investigated as monotherapy for weight loss, its effect is believed to be due in part to a combined dopaminergic and noradrenergic effect on POMC signaling.46 As expected as a single drug therapy it is been associated with modest weight loss in clinical studies.47–49 The limited efficacy of bupropion monotherapy was in part explained with the novel finding that POMC stimulation also initiates an opioid-mediated auto-inhibition pathway.17 It was this novel finding that led to the concept of adding naltrexone, a m-opioid receptor antagonist, which therefore slows down this auto-inhibition mechanism. By combining naltrexone with bupropion it would be possible to sustain POMC activation, leading to more weight loss than with bupropion alone.50 Selective antagonism of the m-opioid receptor has also been associated with reducing the motivational properties of stimuli that elicit the binge eating commonly associated with obesity.51 Animal studies have shown that naltrexone influences neural reward pathways and hedonic eating behavior.52 Because naltrexone does not have a direct and independent effect on hypothalamic control of energy balance (i.e., naltrexone attenuates autoinhibition in response to increased POMC activity), naltrexone by itself has failed to produce consistent or clinically meaningful weight loss when administered as monotherapy.53,54
It is believed that in addition to stimulation of POMC neurons, the NB combination regulates the mesolimbic dopaminergic reward pathways, which may lead to further weight reduction by modulating reward values and goal-oriented behaviors.50,55 Preclinical studies have shown that direct administration of naltrexone and bupropion into the reward system results in a synergistic reduction in food intake,56 suggesting that the two drugs have complementary actions in the reward system.
Clinical Studies—Effect on Weight Loss and Cardiometabolic Risk Factors
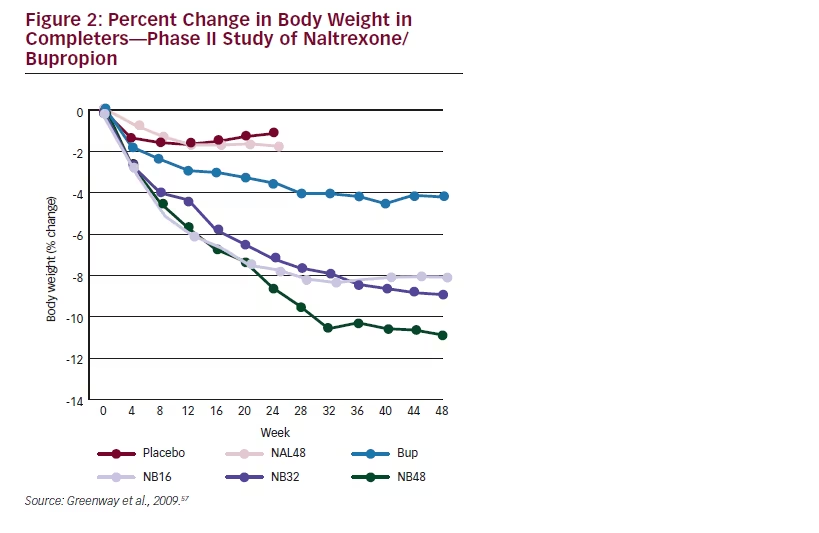
An important phase II dose-ranging study that led to phase III dose selection demonstrated that the NB combination was synergistic and more effective than the individual components.57 In this study of the NB combination (16 [NB 16], 32 [NB 32], or 48 [NB 48] mg/day naltrexone with 400 mg/day bupropion), weight loss in the completer population at week 24 was –7.6 % for NB 16, –7.1 % for NB 32, –7.5 % for NB 48, and –1.1 % for placebo. At week 24, the weight loss of the combination was greater than the sum of the weight loss resulting from the individual components as monotherapy. The trajectory of weight loss was also sustained to week 48, in contrast to the plateau at week 24 observed with monotherapies (see Figure 2).56
The Contrave Obesity Research (COR) phase III clinical trial program investigated the efficacy and safety of NB in approximately 4,500 participants and comprised four studies, which are summarized in Table 1 and Figure 3.58–61 These studies demonstrated that weight loss with NB was seen as early as week 4 and was sustained for at least 56 weeks. In COR-I, bupropion sustained-release (360 mg/day) combined with naltrexone sustained-release 32 mg/day (NB 32) or 16 mg/day (NB 16) were compared with placebo.58 The mean change in body weight
among study completers was –1.8 % in the placebo group, –8.1 % in the naltrexone 32 mg plus bupropion group (p<0.0001 versus placebo), and –6.7 % in the naltrexone 16 mg plus bupropion group (p<0.0001 versus placebo). In COR-II, subjects who did not maintain 5 % weight loss were re-randomized to NB 32 or a higher naltrexone dose of 48 mg/day (NB 48).59 However, NB 48 did not result in additional weight loss, and it was concluded that 32 mg was the maximum effective dose. The CORbehavior modification (BMOD) study combined NB 32 or placebo with an intensive BMOD program that was delivered by registered dieticians, behavioral psychologists, or exercise specialists. The NB 32 group with intensive behavior modification achieved a weight loss of 11.5 %, a significantly greater (p<0.001) weight loss than was seen in the BMOD plus placebo group (7.3 %).60
Treatment of obese patients with diabetes is particularly challenging as many therapies for diabetes lead to weight gain.62 COR-Diabetes Mellitus (COR-DM) recruited patients with type 2 diabetes who were either not taking diabetes medication or who were taking a stable daily dose of oral antidiabetic agents (OADs: sulfonylurea, thiazolidinedione, metformin, dipeptidyl peptidase-4 [DPP4] inhibitors). NB 32 produced a greater weight loss compared with placebo.61 The lower weight loss compared with other COR trials is not surprising: weight loss in patients with diabetes taking OADs is typically lower than weight loss observed in patients without diabetes because some OADs promote weight gain. The weight loss was associated with improvements in glycemic control. NB resulted in significantly greater glycated hemoglobin (HbA1c) reduction (–0.6 versus –0.1 %; p<0.001) and percentage of patients achieving HbA1c <7 % (44.1 versus 26.3 %; p<0.001). In addition to the HbA1c changes observed in COR-DM, major secondary endpoints describing cardiovascular and metabolic risk factors, including waist circumference, visceral fat, high-density lipoprotein (HDL) cholesterol, and triglycerides, were met across all COR trials.
QoL was assessed in the COR trials. An integrated analysis of data from all four trials shows that NB resulted in significantly greater improvement in Impact of Weight on Quality of Life-Lite (IWQOLLite) total score (+11.9±0.3 versus +8.2±0.3 placebo; p<0.001) and all subscores (physical function, self-esteem, sexual life, public distress, work; all p<0.05 versus placebo).63 These improvements were observed as early as week 8.58–60
Clinical Studies—Effect on Eating Behavior
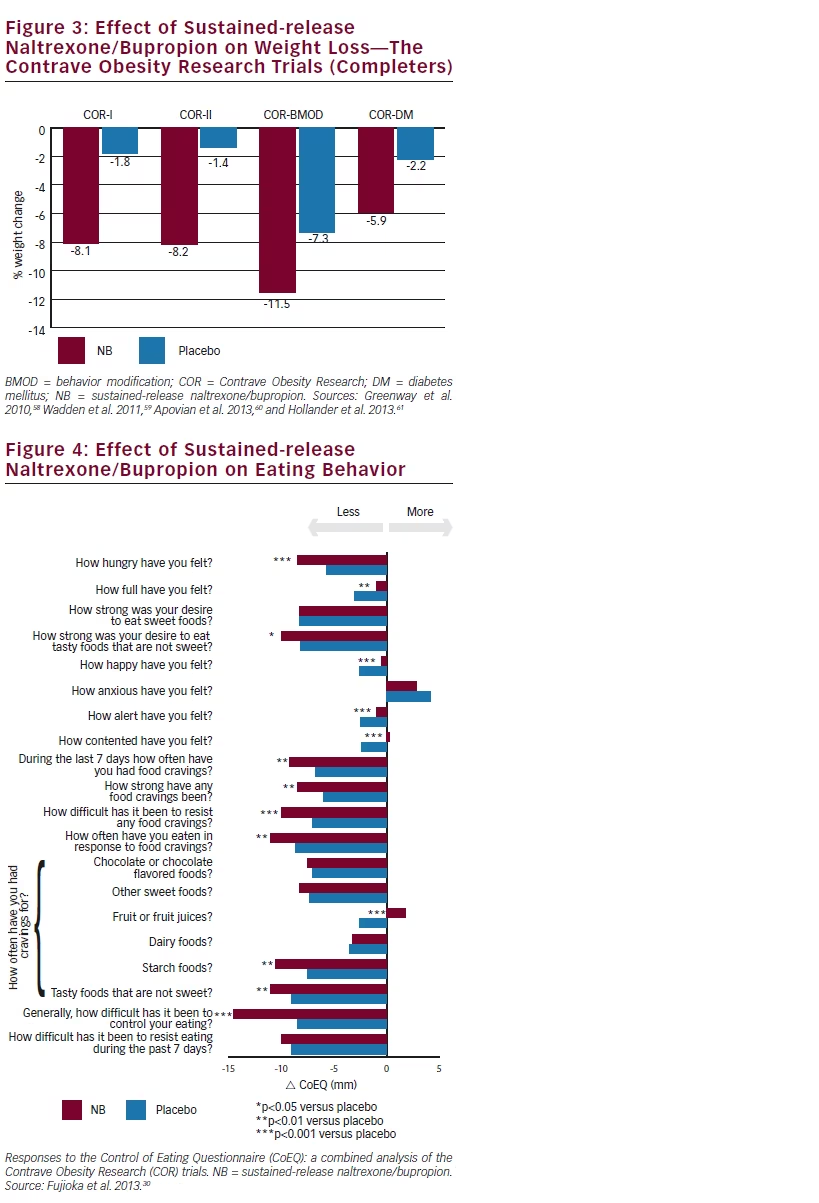
In addition to measures of weight loss, and cardiovascular and metabolic risk each of the COR studies had secondary endpoints of assessment of eating behavior through use of the Control of Eating Questionnaire (CoEQ), a behavioral measure instrument.64 An analysis of all COR studies showed that NB was associated with a significant improvement in a number of CoEQ items related to control of eating and cravings (see Figure 4).30 Specifically, there was a significant improvement relative to placebo in response to the following questions:
- How hungry have you felt?
- During the last 7 days how often have you had food cravings?
- How strong have any food cravings been?
- How difficult has it been to resist any food cravings?
- Generally, how difficult has it been to control your eating?
In addition, there was a correlation between ability to control eating and weight loss. Individuals who reported greater ability to control their eating at week 8 had greater weight loss at week 56.30 In a separate study of 40 obese women, functional magnetic resonance imaging (fMRI) demonstrated that NB 32 decreased hypothalamic reactivity to food cues while enhancing the activation of regions involved in self-control and internal awareness.65
Clinical Studies—Safety and Tolerability
The most common (≥10 %) treatment-emergent adverse events associated with NB were: nausea (32 % NB versus 7 % placebo), constipation (19 % NB versus 7 % placebo), headache (18 % NB versus 10 % placebo), and vomiting (11 % NB versus 3 % placebo).66 These were primarily mild to moderate in severity, occurred early in the treatment course, and did not lead to treatment discontinuation in the majority of patients.58–61 Nausea led to treatment discontinuation in 6.3 %, 6.0 %, 4.6 %, and 9.6 % in COR-I, COR-II, COR-BMOD, and COR-DM, respectively. The incidence of subjects with serious adverse events was low (≤1.6 %) in all trials (the highest rates reported were 3.9 % for NB and 4.7 % for placebo in COR-DM).61
Bupropion is an antidepressant and has been associated with rare occurrences of psychiatric symptoms during treatment and after drug cessation.67 The COR clinical trials therefore assessed psychiatric symptoms. To date, no difference in psychiatric adverse events or depressive and anxiety symptoms has been reported between NB and placebo, and no episodes of suicidal ideation have been reported in treatment groups. No clear evidence of teratogenicity has been associated with the use of NB.
NB 32 was associated with an attenuation in the typical improvements in systolic and diastolic blood pressure associated with weight loss by approximately 1 mmHg.58–61 These are typical pharmacologic responses of bupropion. An ongoing clinical trial, the Light study, is being conducted under a US Food and Drug Administration (FDA) Special Protocol Assessment and is designed to assess the occurrence of major adverse cardiovascular events in subjects treated with NB or placebo.68 A prespecified interim analysis of this trial has shown that NB has met one of the safety goals specified by the FDA.69
Other Clinical Studies
Bupropion is an antidepressant and smoking cessation agent. In an openlabel trial, NB was associated with smoking cessation in the absence of weight gain, typically observed with other smoking cessation treatments, in overweight and obese individuals.70 Improvements in symptoms of depression in overweight and obese women with major depressive disorder were observed in a separate open-label clinical trial.71 These effects warrant further investigation.
With diet and exercise, weight loss is primarily due to a reduction in adipose tissue, and not lean mass. A recent analysis of phase II study data57 investigated the effect of NB on body composition and visceral body fat (VAT) mass. At 24 weeks, NB resulted in significant reductions in VAT mass compared with placebo (–15.0 % versus –4.6 %; p<0.001).72 Importantly, overall weight loss was primarily (78 %) the result of loss of adipose tissue, which is similar to the pattern of weight loss observed with diet and exercise.
Summary and Concluding Remarks
The unmet need of pharmacologic treatment of obesity is slowly changing and physicians will have multiple new pharmacologic treatment options. The timing of this could not be better in the face of our current obesity pandemic and its consequences on health and health care budgets. Obesity has many causes and one well-studied aspect is food overconsumption driven by sensitivity to food stimuli and the pleasure derived from eating. These processes should be effective targets for pharmacotherapy.
NB represents a novel approach that may influence both the hypothalamic control of energy balance and the mesolimbic reward system. This dual mechanism of action will have its place in treatment of the obese patient. Of interest is that this medication may have advantages in patients struggling with craving and overconsumption related to using food as reward.
The weight loss achieved with NB is significant and sustained with an acceptable safety and tolerability profile. Clinical studies have demonstrated that the drug will yield optimal results when combined with lifestyle modifications involving decreased food intake together with increased physical activity. NB therefore represents a new and welcomed pharmacologic option for patients and physicians.