The purpose of life is to reproduce. One purpose of physicians is to make
sure this happens safely. In the developed world this has been pretty
successful. And so we do not want to spoil things: we just want the results
to continue improving and to involve more countries in such success.
We certainly do not want an old-fashioned thing like thyroid disease to
interfere. And so it should not.
Women with thyroid failure can be treated easily with thyroxine
replacement therapy and as long as the mother takes sufficient
thyroxine during pregnancy the baby will be normal. If she does not
take her tablets she will most likely have a dull child or worse.1,2 Not a
good outcome but entirely preventable. The physician needs to verify
that the thyroid is being replaced appropriately and must not just trust
the mother. Trust and verify. But what about an overactive thyroid? Now
that is more of a problem and usually needs an endocrinologist to be
involved with the obstetrician. Hyperthyroid Graves’ disease is most
common in the reproductive age group and although fertility is said to
be reduced by hyperthyroidism, the data supporting this assumption
for mild disease are relatively weak. Clearly, overt hyperthyroidism will
disrupt ovulation but the more common mild degree of hyperthyroidism
is much less likely to do so and it has been estimated that the incidence
of hyperthyroidism in pregnancy is about one in 20, which seems much
too high.3
Nevertheless, plenty of women with mild disease do become
pregnant and need treatment. They need treatment because their risk for
complications is increased. Hyperthyroidism in pregnancy is associated
with increased pre-eclampsia, preterm birth, and need for induction
as well as more rare outcomes,4
and the neonates more often require
intensive care.5
These increased risks appear not to be just the influence
of excess thyroid hormone on the mother but also by the direct effects of
thyroid hormone on the fetus. This has been shown elegantly in mothers
with thyroid hormone resistance but a normal fetus6
where growth was
restricted and there was an increased risk for pregnancy loss. In addition,
in early pregnancy there may be an exaggeration of the hyperthyroidism
because of the influence of human chorionic gonadotropin (hCG) acting
as a thyroid stimulator.7
Treatment is, therefore, usually considered to be
needed for most women who are pregnant with hyperthyroidism.
So how to do this? The treatment of hyperthyroidism has not changed for
more than 50 years. We may be better informed and better able to use the
same old treatments but there has not been a fundamental shift in the
approach. It remains antithyroid drugs, radioiodine and surgery. Each has
well-known advantages and disadvantages and the informed young women
does not like any of them. And right she is. What a terrible choice to have
to make when carrying a precious child. Radioiodine is out straightaway for
obvious reasons. Surgery, the original treatment for Graves’ disease is never
anything to rush into unless you are a surgeon. That leaves antithyroid drugs.
Or does it? Let us first deal with antithyroid drugs. The US Food and Drug
Administration (FDA) has now black boxed propylthiouracil (PTU) because
of the unacceptable increased risk for liver failure, especially in children;8
therefore, its use as first-line treatment is no longer recommended.9
The
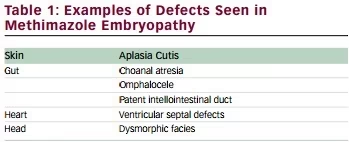
first drug of choice is now methimazole. But methimazole in pregnancy has
been well established to cause what has become known as a methimazole
embryopathy (see Table 1)
10 and potentially involves many different tissues.
So the thyroid community came up with the suggestion to switch to PTU
for the first trimester of pregnancy and then to switch back to methimazole
after organ formation is completed.9
This scenario assumes that you see the patient in early pregnancy. But that
is unlikely to be before 6 weeks—after a good deal of human development
has taken place. In essence, using this approach requires a switch to PTU
at 6 weeks and then a return to methimazole at 12 weeks with barely time
to even determine the correct dose. A better way is to switch antithyroid
drugs when the woman is planning a pregnancy although this ignores the
matter of unexpected pregnancies. If this approach does not sound difficult
enough, who says PTU is safe? There are good experimental data showing the
teratogenic effects of PTU11 and recently Peter Laurberg’s group in Denmark
have shown that there are PTU-associated birth defects in the face, neck, and
urinary system after PTU exposure.12 These tended to be less severe than after
methimazole but still mostly required surgical correction. In my view that ends
the recommended logic. Clearly neither antithyroid drug is a great choice.
So are there more options for the treatment of hyperthyroidism in
pregnancy? There are in fact two other choices. The first is not to get
pregnant. But of course it may be too late for that approach. But it is the
advice that should be offered to those young women already diagnosed
with hyperthyroidism. Delay until you are appropriately treated. And
if you are in a hurry? Or if your eggs are aging? Then go ahead and
have surgery. It is now safer than ever before if you go to a high volume
thyroid surgeon.
The second extra choice is to do nothing. If the disease is mild, the
chance of major complications is small and as the immune suppression
of pregnancy develops in the second trimester the disease will almost
certainly dissipate.13 But physicians are really bad at doing nothing.
Get used to it.







