Globally, non-communicable diseases (NCDs) are currently the leading cause of mortality and morbidity. Of the 56.4 million global deaths in 2015, nearly 39.5 million (70%) were due to NCDs.1 Mental health disorders are one of the known major contributors to NCD burden. They are responsible for 7.4% of global disability adjusted life years (DALYs) and 22.9% of years lived with disabilities (YLDs), making them the fifth leading cause of DALYs and YLDs.2 Depression is one of the most common mental health disorders and is the leading cause of ill health and disability worldwide. Nearly 300 million people are now living with depression, an increase of more than 18% between 2005–2015.3 Similarly, anxiety disorders are also very common, being the sixth leading cause of disability, in terms of YLDs.4
The world is undergoing rapid cultural and social changes, which include aging populations, increasing urbanisation, dietary changes, reduced physical activity, unhealthy lifestyle and limited capacity of the health system to manage the existing burden and prevent further cases.5 This changing scenario has augmented the disease burden transition from communicable to NCDs. Many studies indicate that the co-existence of NCDs, such as hypertension and diabetes, with depression and other psychological morbidities is detrimental to care and prognosis leading to poor glycaemic control, uncontrolled hypertension, greater risk of cardiovascular complications and higher mortality rates.6 A survey conducted by the World Health Organization (WHO) across 60 countries, found that between 9.3–23.0% of patients with chronic diseases had comorbid depression.7
India is witnessing a steep rise in the NCD epidemic including mental disorders. As a result of the demographic transition, the nation is also aging with nearly 104 million elderly persons (≥60 years) and the proportion of elderly has increased from 5.6% in 1961 to 8.6% in 2011.8 For a country like India, with the exponential rise in NCDs along with an increase in aging population, it is becoming increasingly important for the healthcare providers to quantify the burden of comorbid NCDs and mental illnesses, and to design a pragmatic healthcare delivery model that provides holistic management for these conditions. In line with this requirement, a healthcare delivery model was developed and implemented at a rural secondary healthcare setting in Punjab, India during 2015, which envisioned a comprehensive care model for patients suffering from NCDs mainly elderly (≥60 years) with diabetes and hypertension. To provide holistic care, patients were screened for common mental illnesses using simple validated tools and linked to mental healthcare services, if needed. Against this background, we conducted this study to determine the prevalence of depression and generalised anxiety disorder among the elderly population with diabetes and/or hypertension and explore the risk factors associated with it.
Methods
Study design
A cross-sectional study was conducted using a semi-structured questionnaire at district Fatehgarh Sahib in the northern state of Punjab, India (population 600,000; area 1,147 km2; sex ratio 871; literacy rate 80.3%). The government health infrastructure of the district includes six secondary level hospitals, 13 primary level health facilities, 26 subsidiary health centres, 72 sub-centres along with the private sector with
nursing homes and practitioners who play a major role in providing healthcare services.
Specific setting
The study was conducted at two Community Health Centres (Khera and Bassi Pathana) of Fatehgarh Sahib, which is the field practice area of the Department of Community Medicine, School of Public Health, Post Graduate Institute of Medical Education and Research, Chandigarh. Each facility caters to a population of around 150,000. The department conducts a chronic disease clinic at both these public facilities once a week which targets mostly the geriatric population. Besides preventive and diagnostic services, the patients who are diagnosed with diabetes or hypertension are also provided medicines and weekly follow-up free of cost. The clinic is also supported by a charitable trust which is actively engaged in community service in that area. Around 80 patients visit the facility per clinic day.
Study population
All patients aged ≥60 years or above and diagnosed with diabetes and/or hypertension attending a chronic disease clinic in Fatehgarh Sahib district of Punjab, India.
Study period
The study was conducted between September 2017 and June 2018.
Sample size and sampling
Considering the prevalence of depression among elderly with comorbid diabetes as 25%,9 5% precision and 10% non-response rate, the sample size was calculated to be 310. (Stat-calc, Epi Info: version 7.2.0.1). All new patients aged ≥60 years diagnosed with diabetes and/or hypertension were recruited at the clinic consecutively until the required sample size was attained.
Data collection process
Data were collected using a structured questionnaire administered by the principal investigator (MV) and another trained public health nurse (GS) at the chronic disease clinic. The questionnaire collected information on socio-demographic and clinical characteristics. The socio-demographic variables included age, gender, locality (urban/rural), education, occupation, family income, marital status and family type. The clinical characteristics included the body mass index (BMI) of the patients, presence of morbidities such as diabetes, hypertension or both; duration of the disease; history of stroke, myocardial infarction or coronary artery disease; tobacco, alcohol or any other substance abuse as per standard definitions; and family history of certain illnesses.10 Validated tools were used to assess depression (Geriatric Depression Scale) and generalised anxiety disorder (GAD-7 scale).11,12
The Geriatric Depression Scale is a 30-item scale where each question is given a score of 0 or 1. Questions 1, 5, 7, 9, 15, 19, 21, 27, 29 and 30 have a reverse scoring where a “no” response is given a score of 1. All other questions are given a score of 1 if the answer was “yes”. The interpretation of the total score is as follows: normal, 0–9; mild depression, 10–19; severe depression, 20–30. For this study, the validated Hindi version of the scale was used.13 GAD-7 scale is a -item scale where each item is given a score ranging from 0–3 (0, not at all; 1, several days; 2, more than 50% of days; 3, nearly every day). The score against each question is added and interpreted as follows: minimal anxiety, 0–4; mild anxiety, 5–9; moderate anxiety, 10–14; severe anxiety, 15–21. A score of ≥10 is indicative of a possible diagnosis of GAD. For this study, Hindi version of GAD-7 was used, which has been shown to have to acceptable level of diagnostic concordance with the diagnosis made for a psychiatric disorder by psychiatrist.14 It has also been used in the elderly clinic population in an Indian setting.15
Analysis and statistics
Quantitative data were double-entered and validated using EpiData entry version 3.1 and subsequently analysed using EpiData analysis version 2.2.2.182 (EpiData Association, Odense, Denmark). The key outcome variables were the prevalence of depression and GAD, which were expressed in percentages. Multivariable logistic regression was carried out to explore factors associated with depression and GAD. Variables with a p-value <0.2 in the univariable analysis were included in the regression model after ruling out collinearity. Odds ratios with 95% confidence interval (CI) were used to measure the strength of the association.
Ethics approval
Ethics approval was obtained from the Institutional Ethics Committee of Post Graduate Institute of Medical Education and Research, Chandigarh, India, and The Union Ethics Advisory Group, Paris, France. Written informed consent was obtained from the participants before the interview.
Results
Socio-demographic and behavioural characteristics
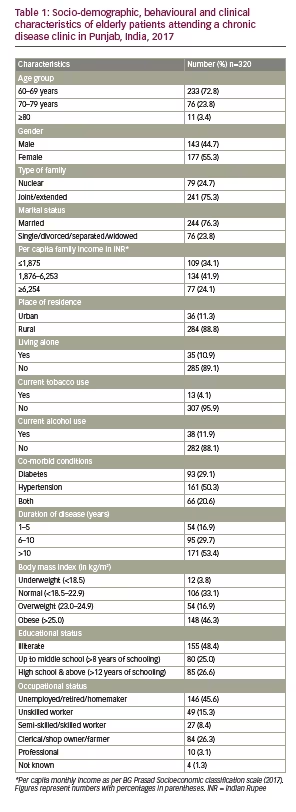
Out of a total of 330 patients who attended the clinic during the study period, 320 gave consent for the interview (response rate of 97%). Table 1 shows the socio-demographic, behavioural and clinical characteristics of the respondents in the study. The majority of respondents were females (55.3%; n=177), between 60–69 years of age (72.8%; n=233), residing in rural areas (88.8%; n=284) and living in joint families (75.3%; n=241); and nearly half were illiterate (48.4%; n=155) and unemployed (45.6%; n=146). Fifty percent (n=161) of them were suffering from hypertension, 29.1% (n=93) had diabetes, 20.6% (n=66) were suffering from both the diseases, and 63.1% (n=202) were overweight/obese (BMI >23.0 kg/m2).
Depression and generalised anxiety disorder
Overall depression was found in 58.2% (95% CI 52.6–63.4%) of the study participants; of which 34.1% had severe depression. Among females, both depression and severe depression were found to be significantly higher with 72.4% and 49.2%, respectively (p<0.001; Figure 1A).
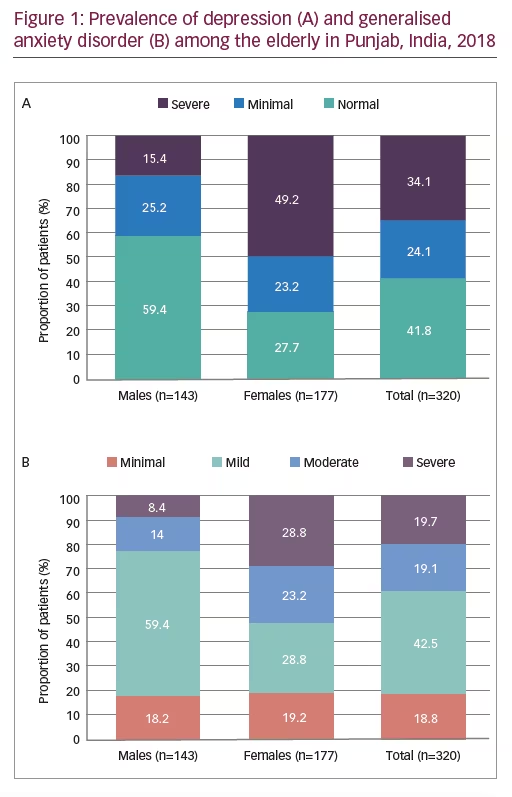
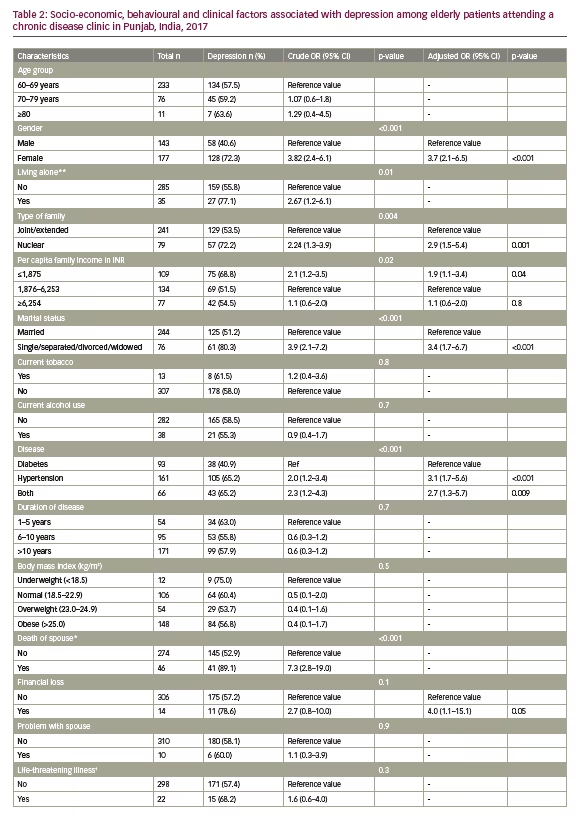
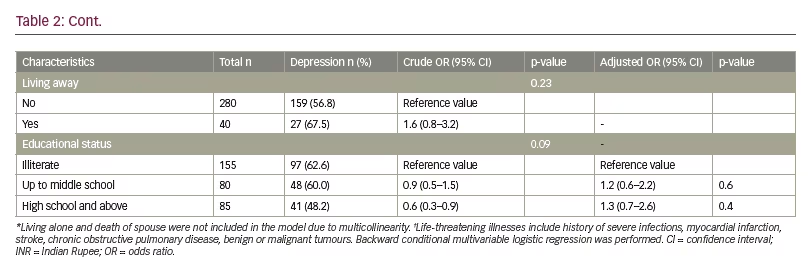
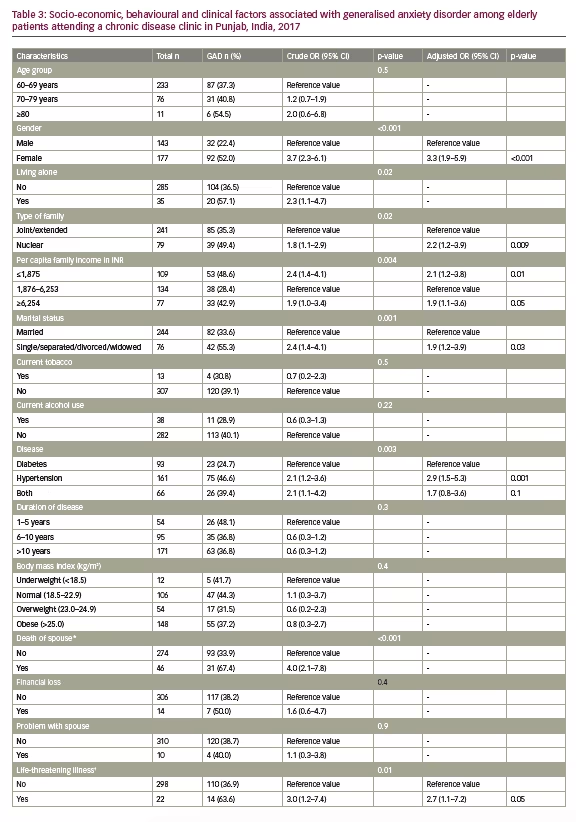
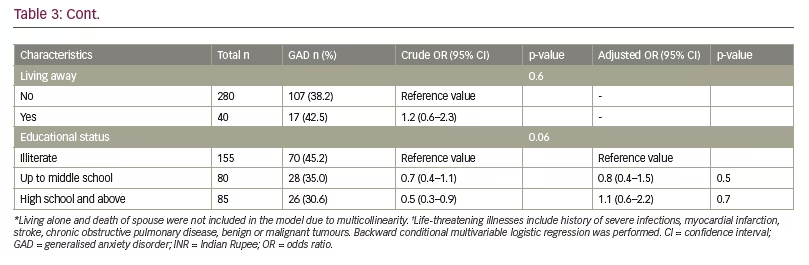
Similarly, the proportion of GAD among the elderly was found to be 38.8% (95% CI 33.6–44.2%); while 19.7% had severe GAD. GAD and severe GAD were higher among females with 52.0% and 28.8%, respectively (p<0.001). (Figure 1B). The risk factors associated with GAD and depression are shown in Tables 2 and 3. Female gender, nuclear family, being single/separated/divorced/widowed, low-income status and comorbid NCDs especially hypertension emerged as the risk factors associated with depression (Table 2) and GAD (Table 3) in the study population. Ironically, stressful factors like financial loss, problems with spouse, life-threatening illness (such as history of severe infections, myocardial infarction, stroke, chronic obstructive pulmonary disease, benign or malignant tumours) and living away from the family did not emerge significantly in multinomial logistic regression; while factors like living alone and death of spouse were not included in the model due to multicollinearity.
Discussion
This is one of the first studies conducted in India looking at the co-morbidity of mental illnesses among patients with NCDs in the elderly age group. The study findings suggest that one in two elderly people with existent NCDs, such as hypertension and diabetes, suffer from depression and one in three have GAD. The majority (55%) of the respondents were female and mostly residing in rural areas and in joint families, and about half of them were illiterate and unemployed. Females outnumber males probably because the study population (elderly with NCDs) is markedly different from the general population. The following reasons could explain the high female:male ratio in the study population: i) higher life expectancy of females in the elderly age group; ii) better health-seeking behaviour among females, this being a hospital-based sample. It is also well known that undiagnosed cases of diabetes/hypertension are higher among males because of their poor health seeking.16,17
We believe that the high burden of comorbid NCDs and mental illnesses could be due to psychological co-morbidities leading to hypertension, diabetes and other cardiovascular events; and chronic diseases leading to psychological co-morbidities such as stress, anxiety, and depression. This has important public-health implications. Major modifiable risk factors for NCDs such as poor diet, physical inactivity, tobacco use and harmful alcohol use, are exacerbated by poor mental health. Thus, mental illness is a key risk factor for NCD. In addition, individuals with mental health conditions are less likely to seek help for NCD and symptoms may affect adherence to treatment as well as prognosis.18
There is considerable evidence showing that psychological factors including depression and anxiety predict the onset and severity of cardiovascular morbidities such as hypertension, metabolic syndrome and diabetes, which contribute to higher morbidity and mortality.19 On the other hand, chronic diseases such as diabetes and hypertension also lead to depression, anxiety, and stress as reported in the present study. Similar findings have been presented in the previous literature where patients have reported poor psychological health due to the disease itself and have expressed concerns about the chronic and potential long-term complications of the disease.20,21
In diabetes, there is evidence of decreased quality of life and poor mental well-being because of fear and distress associated with the disease that is difficult to distinguish from other common mental disorders.22 Future studies should focus on measuring these aspects related to diabetes. One such instrument is the Problem Areas In Diabetes questionnaire which covers a wide variety of emotional concerns that are associated with depressive symptoms and undesirable coping styles.23 Female gender, residing in a nuclear family, being separated/widowed/divorced and the presence of other chronic diseases was significantly associated with depression and anxiety in the present study population. Female gender is a predominant risk factor for psychological morbidities probably due to hormonal fluctuations and societal driven discriminatory attitudes both within and outside the family.24–27 The present study found that elderly people living in a nuclear family system were more likely to suffer from depression and anxiety as supported by other studies.28–30 This could be due to the higher level of support that a joint family offers to the elderly than a nuclear family system, especially physical, social and emotional support. Mental illnesses are also common among those who are separated/divorced/widowed.29,31–34 This could be due to mental stress, loneliness and lack of support as a result of the loss of the partner/spouse.
The findings or the present study have the following programmatic implications: first, given the high burden of anxiety and depression among elderly patients who attend the NCD clinics, all elderly patients should be formally and regularly assessed for depression and anxiety disorders, at least once a year, using simple validated tools. Second, considering the co-existence of mental illness and NCDs, WHO has recommended an integrated approach to manage mental illnesses among persons with NCDs and reducing the risk of NCDs among people with mental illnesses. This model of care will improve patient satisfaction, adherence to treatment and health outcomes, and it is proven to be cost-effective as well.35
Third, primary healthcare physicians and physicians in charge of NCD clinics need to be trained to identify common psychological morbidities such as depression and anxiety, and take appropriate action. All the physicians at the primary health centres need to be trained under the District Mental Health Programme of the National Mental Health Programme (NMHP) of the Government of India to manage them, and should also have access to effective evidence-based interventions.36 Fourth, special counselling and follow-up services should be offered to those with anxiety and depression. Fifth, the burden of comorbid NCDs and mental illness among the elderly presents a strong rationale for integration of the NMHP; the National Program for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke; and the National Programme for Health Care of the Elderly to provide mental-health care to this vulnerable population at public health facilities. Sixth, it is prudent to include mental disorders in the broad rubric of NCDs which is currently missing.
The study had some strengths. It was conducted at a rural government health centre undertaking mental health screening among elderly with comorbid chronic diseases in operational settings and thus, it reflects the ground reality of the situation. This model of healthcare can be replicated elsewhere across the country in similar settings. The tools used to screen mental illness were standard validated tools and therefore have the least chance of a false diagnosis. The data were double entered and validated using EpiData software to minimise data entry errors. There were some limitations to the study. The study was carried out in a single rural health clinic, raising questions on the generalisability of the findings in other settings. The study is a cross-sectional design, causal pathways underlying the reported associations cannot be ascertained. This was a clinic-based study, so referral bias could have affected the results.
There was no control group, so we do not know whether the prevalence of psychological morbidities, such as anxiety and depression, is similar in the general population. Finally, the patients were evaluated on questionnaires and not assessed by a specialist psychiatrist, which is considered as the gold standard for making a psychiatric diagnosis.
Conclusion
To conclude, there is a huge burden of comorbid NCDs with mental illness among the elderly population in India. There is a need to develop an integrated care model to manage this comorbidity to this vulnerable population at all levels of health care facilities.







