The prevalence of diabetes is on the rise globally, and with one in two adults remaining undiagnosed,1 there is an urgency to broaden our services to include community partnerships. Extreme poverty is often found in remote areas where people are hard to reach, and have limited access to schools, healthcare, safe drinking water, and electricity. In 2016, the World Bank declared, “nearly 385 million children live in extreme poverty”.2 In 2018, the realization occurred that although “fewer people are living in extreme poverty globally, the decline in poverty rates has slowed”.3 According to the World Bank, the slowing decline in poverty is possibly due to the “falling commodity prices, conflict, and economic challenges for developing countries”.3
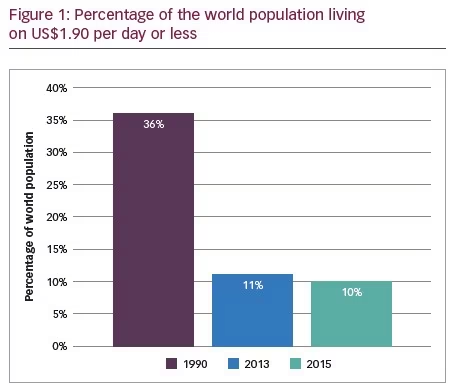
In 1990, 36% of the world’s population (1.85 billion people) lived on approximately US$1.90 per day; in 2013, it was 11% of the world’s population; and in 2015, it dropped to 10% of the world’s population (736 million people) (Figure 1). Approximately 1.1 billion fewer people are living in extreme poverty than in 1990;4 however, the progress in poverty rates has been erratic throughout the world. There are 47 million people living in the East Asia and Pacific region that are extremely poor, whereas in Europe, and Central Asia there are 7 million people who are experiencing poverty.4 With regards to sub-Saharan Africa, >50% of the population are extremely poor.4 In 2015, 413 million people were living on less than US$1.90 per day.4 According to the World Bank, it is possible that 9 out of 10 people living in sub-Saharan Africa will be extremely poor by 2030 if these trends continue.4 The continual rise of poverty in many sub-Saharan African countries is related to several factors, such as corruption and poor governance, unemployment; poor infrastructure; limited resources; longterm conflicts; poor health policies; cultural factors; limited influence upon social and public policies, limited skills, knowledge, and education; and personal development.5
Data from the World Bank from 1960 to 2017 reveal a relocation of the world population to more urban areas, with the exception of Antigua and Barbuda, Armenia, Aruba, Austria, Barbados, Belize, Channel Islands, Guyana, Liechtenstein, Samoa, St. Lucia, and Tajikistan, where more of the population still reside in rural areas.6,7 Countries where the majority of the population live in rural areas, have an elevated prevalence of diabetes as compared to those which have transitioned to urban areas.
Diabetes—data and healthcare
Diabetes is the leading cause of blindness, kidney failure, amputations, heart failure, and stroke.8 According to the Diabetes Research Institute Foundation, more than 30 million Americans have diabetes, and worldwide, diabetes affects more than 422 million people.9 There are about 60 million people with diabetes in Europe.10 The prevalence of diabetes is increasing among all age groups through Europe,10 possibly due to obesity, inactivity, and limited consumption of nutrient-dense foods. Worldwide, elevated blood sugar is the cause of death for 3.4 million people annually.10 Approximately 80% of these deaths occur in low- and middle-income countries, and approximately 50% are in those under 70 years of age.10 The World Health Organization projects that by 2030, mortality from diabetes will be double what it was in 2005.10
The terms “health disparity” and “health inequalities” are usually used interchangeably; however, for the purpose of this article, the term health disparity will be used and is defined by the Centers for Disease Control and Prevention as “gaps in health between segments of the population”.11 Healthcare disparity occurs among race/ethnicity, socioeconomic status, age, location, gender, disability status, and sexual orientation.12 Health and healthcare disparities affect groups of people that limit their quality of healthcare which results in unnecessary costs. Multiple social determinants, such as, economic stability, neighborhood and physical environment, education, food security, community and social context, and the healthcare system, affect health and healthcare disparities.
In the USA, approximately 15–20% of the population reside in rural areas and experience suboptimal healthcare compared to those living in urban and suburban areas.13 Health disparities are established economically, socially, geographically, and racially, and are rooted in ethnicity. All of these factors limit access to quality healthcare; hence, solutions are challenging and people with diabetes present with significant complications that could be preventable. Those who live in remote areas such as distant ranches, reservations, or the frontiers must travel long distances to reach a healthcare provider making access challenging; therefore, they may avoid seeking healthcare, resulting in co-morbidities.13 The lower the person’s economic status, the greater risk of poor health outcomes.14 Health disparity is systemic and affects the health status of all population groups, which inevitably affects societies economically and socially.
Shifting to nutrient-dense foods
The dramatic shift in global food consumption to non-nutrient-dense foods is threatening the world’s most vulnerable populations, such as, children, pregnant women, and the ill, hence increasing the prevalence of malnutrition and non-communicable diseases (NCDs), such as, heart disease, type 2 diabetes, and cancers.15,16 As incomes rise among populations living in low- and middle-income countries (LMICs), there is an adoption of a Western life-style that includes non-nutrient-dense foods and processed foods. Additionally, our current food system has developed environmental stressors, such as greenhouse gas emissions and biodiversity loss. There is a need to increase nutrient-dense foods that are sustainable to ensure a healthier future for the planet and consequently have a healthier outcome among all populations.
Poor-quality diets are at the foundation of all forms of malnutrition, and directly contribute to undernutrition, over nutrition, and diet-related NCDs.17 Globally, one in five deaths (11 million) in 2017 were associated with a poor diet.18 Cardiovascular disease was the largest cause of mortality, followed by cancer and type 2 diabetes.19 As the global food system becomes increasingly calorie rich and nutrient poor, mortality rates rise. A major contributor to poor health is food that has been processed, resulting in loss of micronutrients and added salt, fats and sugars. Consequently, the shift from nutrient-dense foods to non-nutrient dense foods as a major source of nutrition is raising the rates of NCDs among both, high-income countries and LMICs. 20 This transition began in the 1990s among the LMICs; however, was not recognized until NCD rates began increasing globally.21 As malnutrition and NCDs continue, the production of food is impacting the environment and jeopardizing the security of food on the planet with agricultural production being the primary force of biodiversity loss, climate change, and environmental pollution.22
Plant-based diets
The Food and Agriculture Organization of the United Nations (UN) defines sustainable diets as “those with low environmental impacts which contribute to food and nutrition security and to healthy life for present and future generations”.23 In 2015, the UN, along with 193 member states, created 17 sustainable development goals to build a healthier and more sustainable future for all. There is an association between what is healthy for people and what is sustainable for the planet.24,25 This association can been seen in populations that consume a high amount of processed meat and non-nutrient-dense foods; this type of food pattern results in increased risk of heart disease and type 2 diabetes.25 In addition, the methods of food production associated with raising cattle increases the levels of greenhouse gases, and uses more fresh water and land than plant-based foods.27
Plant-based diets include fruits, vegetables, whole grains, legumes, nuts, and seeds that contain a diverse range of micronutrients, fiber, and phytonutrients. The position paper of The Academy of Nutrition and Dietetics states that those who consume a predominately plant-based diet are at a reduced risk of ischemic heart disease, type 2 diabetes, hypertension, certain types of cancer, and obesity.28 Eating more plant-based foods can help lower total and low-density lipoprotein (LDL) cholesterol levels and blood pressure,29 which is significant for people with diabetes. The fiber in plant-based foods helps control blood sugars, and plant-based foods are lower in saturated fats.30 Saturated and trans-fats have been shown to cause insulin resistance, whereas mono-, poly- and omega-3 fatty acids do not have an adverse effect.31,32
Foods that promote personal and planetary health include legumes (pulses), soybeans, nuts, seeds, and green leafy vegetables. Legumes are a rich source of soluble fiber, essential vitamins and minerals, and contribute to planetary health through their ability to fix nitrogen from the air and supplement into the surrounding soils, as well being an affordable source of nutrition.33 However some legumes, such as soybeans, are being industrially produced to satiate the growing demand of animal feed, which are often grown in fragile ecosystems such as The Amazon Rainforest.34 Understanding the context of where and how foods are grown is an important aspect of ensuring sustainable food systems.
Conclusion
The factors associated with living in poverty include being uneducated, living in a remote rural area, working in agriculture, and being <18 years of age. The consequences of poverty include food insecurity and limited access to education, healthcare, safe drinking water, electricity, and medication. The combination of poverty and the prevalence of global diabetes on the rise, with one in two adults remaining undiagnosed,1 reflects an urgency to broaden our services to include community partnerships. Poor heath is a vicious cycle, and incurs increasing employment instability and food insecurity, the latter of which may cause multiple deficiencies in various vitamins, minerals and macronutrients. It is, therefore, critical for the medical community to explore, embrace, and implement solutions to improve food systems globally which will reduce the occurrence of NCDs. We need to align agricultural policies with nutrition goals; improve access to, and utilization of, nutrient-dense foods; increase the availability of nutrition education; and include telehealth among clinics and/or hospitals.
Telehealth is a vehicle that can provide diabetes self-management education in hard-to-reach locations through live presentations, recorded webinars, and podcasts. In addition, clinical assessments can be conducted via telehealth, eliminating the transportation barrier, and can possibly address the psychosocial needs of families with diabetes. Partnering with local, state, and federal organizations, as well as with local community gardens in urban areas, enhances shared information and prevents working alone.
Paying more attention to our food supply and nutrient-dense foods, we can thrive on a sustainable lifestyle, especially those living with diabetes. Nutrient-dense foods, such as fruits, vegetables, whole grains, seeds, and legumes can help prevent nutrient deficiencies related to inadequate intake of essential nutrients, like zinc, selenium, and vitamins A, C, and E. Whole grains, seeds, and legumes are of particular interest because they are more sustainable to produce, budget-friendly, and have a high-quality nutrition profile often missing in the diets of lower-income populations. In contrast, processed foods high in sugar and salt are low in essential nutrients and contribute to the rising rates of non-communicable diseases. Sustainable and healthy foods can be budget-friendly by including a diversity of items such as dried whole grains (barley, sorghum, wheat), fruits and vegetables, canned legumes (beans and lentils), and seasonal produce. Health programs and public health policies can help promote the consumption of nutrient-dense foods in low-income areas. For example, doctor-prescribed produce programs (produce Rx), Supplemental Nutrition Assistance Program (SNAP) incentives at farmers markets (Health-Bucks), and nutrition education courses targeting low-income communities. Nutrition education can address food accessibility, affordability, utilization, sustainability, business and gardening skills, which help promote healthier diet patterns for low-income families.
The evidence for nutrient-dense foods, a change in farming practices, and the implementation a food system that balances a plant-based diet with very lean protein sources, continues to grow and promote personal and planetary wellbeing. Sustainable foods are those that are nutritionally adequate, economically affordable, culturally acceptable, and environmentally friendly. All global populations have the right to good health, happiness, and prosperity which can transform people’s mental health and coping skills. Having sustainable, nutrient-dense, and affordable foods will significantly reduce rates of malnutrition among children and adults and decrease the incidence and prevalence of diabetes.34 Sustainable nutrition, medication security, blood sugar control, and well-being for all are the desired and appropriate outcomes among those with diabetes living under the limitations of socioeconomic situations.







