Type 1 diabetes is the most common metabolic disorder in children. Worldwide, there are approximately 490,000 children with type 1 diabetes, and 78,000 new cases are diagnosed each year.1 As of today, the incidence of type 1 diabetes in children younger than 15 years old is increasing. If this trend continues, new cases in European children less than 5 years are predicted to double between 2005 and 2020.2 Type 1 diabetes is a lifelong condition with short- and long-term implications.
Type 1 diabetes is the most common metabolic disorder in children. Worldwide, there are approximately 490,000 children with type 1 diabetes, and 78,000 new cases are diagnosed each year.1 As of today, the incidence of type 1 diabetes in children younger than 15 years old is increasing. If this trend continues, new cases in European children less than 5 years are predicted to double between 2005 and 2020.2 Type 1 diabetes is a lifelong condition with short- and long-term implications. Recommendations by the American Diabetes Association (ADA) support the use of an intensive insulin regimen that involves a ‘basal/bolus’ pattern of insulin administration to maintain blood glucose levels as close to normal as possible, with a target glycated haemoglobin (HbA1c) of 7.5 % to 8.5 % in children aged younger than 6 years, less than 8 % in children aged 6–13 years and less than 7.5 % in those aged 13–18 years.3 The recommendation of the International Diabetes Federation (IDF) and the International Society for Paediatric and Adolescent Diabetes (ISPAD) is to reach a target of less than 7.5 % in all age groups (children and adolescent).4 These targets can be achieved by intensive management of the condition, involving multiple insulin injections, blood glucose monitoring, nutrition planning and detection and treatment of hypoglycaemia.
5 The medical benefits of insulin regimes in type 1 diabetes are well established.6–8 However, there is a danger that metabolic targets may be attained at the expense of the psychological wellbeing of children and their families. Children and adolescents with diabetes are still developing cognitively and emotionally, therefore self-management is challenging,9 particularly when acknowledging or adapting to the disease conflicts with their lifestyles.5,10 In adolescence, these challenges may result in conscious behaviours (e.g. choosing not to inject at a social event) that may be mistaken for simple non-compliance.10 With increasing age, autonomy in relation to disease management becomes important.11 Selfmanagement presents different challenges to younger patients: children frequently make mistakes in self-administering insulin but increasing age is associated with improved insulin administration skills.12 There is therefore a need to make the process of insulin administration as simple and convenient as possible to avoid errors, particularly in relation to adjusting doses of insulin.
Insulin pens, comprising an insulin cartridge, a dial button to set the dose and disposable needles, have facilitated insulin delivery for young people.13 Compared with syringes, pen devices lead to better compliance, because a pen is easier to carry around, are quicker to inject, give more accurate dosing and are more cost-effective.14 To cope with the needs of an increasingly young user base, pens have become more sophisticated with higher technology, easier to use and are able to dose in smaller increments. Half-unit dose increment insulin pens
have been shown to be more accurate than syringes for the delivery of low insulin doses.15 This provides greater flexibility to achieve target insulin doses for younger children and adolescents with type 1 diabetes. Half-unit dose accuracy is particularly important in this patient population because studies have shown a positive correlation between the percentage of hypoglycaemic events in children and the errors in the accuracy of a regular insulin dose.13 JuniorSTAR® (Sanofi) is a reusable, half-unit pen weighing ~34 g ± 10 % (with outer body made of aluminium material) existing in three colours (blue, red and silver) to allow differentiation between insulins and allowing dialling by half-unit increment, up to 30 units per injection. It was developed for young people with diabetes. The JuniorSTAR is pending CE mark (under the responsibility of Haselmeier) and is planned to be used with insulin glargine (Lantus™), insulin glulisine (Apidra™) and human insulin (Insuman™). This article describes a survey whose objective was to assess the major features and usability of JuniorSTAR pen through individual, parent and diabetes specialist nurse ratings.
Materials and Methods
The survey was a non-comparative assessment of JuniorSTAR in insulin pen users from five European countries (France, UK, Germany, Italy and Spain). Performance was assessed through individual, parent and diabetes specialist nurse ratings of the attributes of this pen, given as responses to a questionnaire. Participants were interviewed on a face-to-face basis. The study enrolled: 1) nurses who were working with children with type 1 diabetes (n=109); 2) parents of children with type 1 diabetes aged less than 5 years (n=16); 3) children aged 6–12 years (n=8); 4) parents of children aged 6-12 (n=12); and 5) adolescents with type 1 diabetes aged 13–18 years (n=22). Only diabetes specialist nurses who teach at least five children a week on how to use a reusable pen were enrolled. All participants signed a consent form. All patients were already using an insulin pen: either disposable (18.3 %), reusable (57.3 %), a combination of both reusable and disposable (23.2 %) or type of pen was not recorded (1.2 %). JuniorSTAR was rated on a five-point scale on 3 scales as follows: when asked to rate the product, 1 = very poor; 2 = somewhat poor; 3 = neither poor nor good; 4 = somewhat good; 5 = very good or 1 = very difficult; 2 = somewhat difficult; 3 = neither easy nor difficult; 4 = somewhat easy; 5 = very easy. When asked to agree/disagree with a statement, 1 = completely disagree; 2 = somewhat disagree; 3 = not sure; 4 = somewhat agree; 5 = completely agree. We defined a positive response as the percentage of the total respondents (answers of parents and children were pooled) who responded with either a 4 or a 5 score.
Results
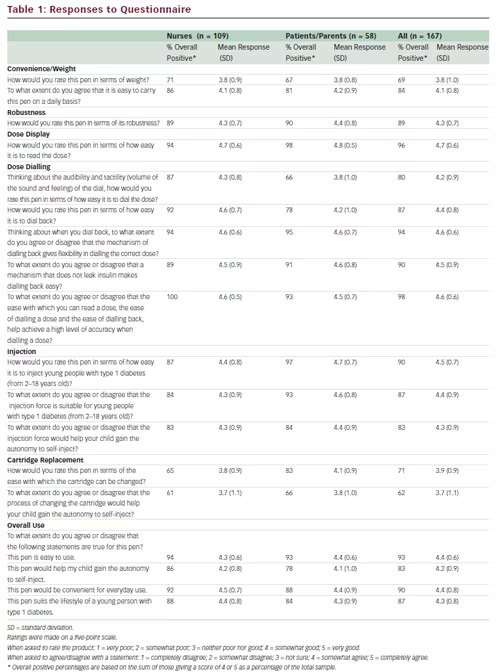
The responses of all 167 participants, as total study population and patients/parents and nurse subgroups, are presented in Table 1. Participants rated JuniorSTAR highly (min–max standard deviation [SD]: score: 3.7 (1.1)–4.7 (0.6)) across all attributes tested.
In terms of practicality, JuniorSTAR was found to be easy to carry in daily life by 84 % of all participants (81 % of patients/parents; 86 % of nurses) with a weight rated good or very good by 69 % of participants and sufficiently robust to withstand the daily demands of children by 89 % of participants.
In terms of usability, 96 % agreed that the dose display was easy to read (by children 98 %; by nurses, 94 %). When assessing the dose dialling, 80 % agreed that the audibility and tactility of the clicks made dialling a dose easy (66 % of children; 87 % of nurses). Furthermore, 87 % agreed that the pen is easy to dial back in case of accidentally dialling a dose larger than required (78 % of children/parents; 92 % of nurses), and 94 % found that the dial-back mechanism of JuniorSTAR permitted flexibility in dialling the correct dose. Of the participants, 90 % considered that the dial back mechanism, which does not leak insulin, increases the ease of dial back. Given the ease of reading, dialling and dialling back the dose, 98 % of all participants found that JuniorSTAR helped patients achieve a high level of dose dialling accuracy (with 93 % in children/parents and 100 % in the nurses’ population).
Regarding suitability for young patients, 90 % of all participants reported that the JuniorSTAR is easy to inject for young patients (with 97 % in children/parents; 87 % in nurses), and 87 % found the injection force to be suited to the ability of young patients with type 1 diabetes (93 % in children/parents; 84 % in nurses). Regarding the ease of changing the cartridge, 71 % of the total population (83 % of patients; 65 % in nurses) found it easy to change the cartridge.
Overall, 93 % of participants found JuniorSTAR half-unit pen to be easy to use, 90 % considered JuniorSTAR convenient for everyday use (88 % by children/parents; 92 % by nurses). JuniorSTAR half-unit pen was considered as suitable to the lifestyle of a young patient with type 1 diabetes by 87 % of the total population (84 % by children/parents; 88 % by nurses), with 83 % of all participants considering that JuniorSTAR would help a child gain the autonomy to self-inject (78 % by children/parents; 86 % by nurses). The profile of responders and their concerns differed, and this was reflected in the difference in responses between nurses and children/parents. In some cases, the question was more related to the patient’s personal preference (e.g. injection force) but other questions were of more concern to nurses (e.g. changing cartridges).
When the scores were below 4 (non-positive responses to the questions), the answers were mostly scored as 3 (neutral responses). Complete disagreement (which was a score of 1) was never reported by more than 2 % of respondents for any question. When asked the question, “can you give me one word that best describes how you feel about this pen”, the most common replies were practical, easy and simple.
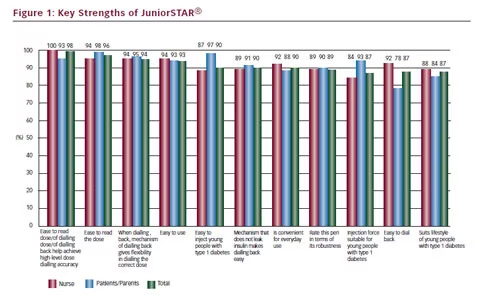
In summary the key strengths of the half-unit insulin pen, JuniorSTAR, found in at least 84 % of the total population, are its practicality, its ease of carrying (84 %), ease of reading the dose (96 %), ease of dialling back (87 %) and a suitable injection force for young people (87 %).
This ease of use should make it easier to teach patients how to perform dose adjustments, particularly in terms of accurate dose dialling at halfunit increments and dialling back. In the qualitative overall assessment, only a minority have identified some points that could be improved such as the dial is too stiff and not sufficiently smooth and the cap is too stiff to remove. The adolescents would prefer a quieter dial to assure discretion.
Conclusions
Children and adolescents are faced with many challenges in managing their condition. It is important for them to have access to insulin delivery technology that can permit adjustment of their insulin doses to be as easy and accurate as possible. In our survey, the JuniorSTAR half-unit insulin pen was well received by patients with type 1 diabetes and their caregivers. JuniorSTAR was found to be easy to carry, easy to read for accurate dose dialling and easy to dial back so mistakes could be corrected without any insulin penalty, with an injection force suited to the ability of young patients with type 1 diabetes. Considering these advantages, the JuniorSTAR half-unit insulin pen is likely to be easy to handle and suitable for the lifestyle of the young type 1 diabetes population.







