‘We are what we think. All that we are arises with our thoughts… Be the witness of your thoughts.’ – Gautama Buddha1
The biomedical approach in modern medicine focuses on disease as a deviation from the norm of measurable biological variables. The social, psychological and emotional dimensions of health are largely ignored. However, it is not appropriate to designate diseases into distinct categories of physical or mental ailments. A patient’s perception of disease does not follow this clear divide between the mind and the body.2 Most physical disorders have a strong psychological, emotional and mental impact which determines patient experience and his/her reaction to it. Similarly, most mental ailments have a strong somatic component that needs to be paid attention to.3 Holistic care, therefore, must focus on both physical as well as psychosocial health.
The biomedical model has since been replaced by the more humanistic and patient-centred ‘biopsychosocial’ model in the 21st century, with a focus on the patient at each level – biological, psychological and social.3 It involves the integration of disease pathology with the patient’s experiences and perceptions, social interactions and patient-doctor communication. An understanding of this biopsychosocial model and its implementation is particularly relevant in the management of chronic metabolic disorders such as obesity, diabetes, hypertension, metabolic syndrome, polycystic ovary syndrome, non-alcoholic fatty liver disease and cardiovascular disorders, where patient attitude and behaviour, lifestyle modification, stress management and long-term adherence to therapy hold the key to successful outcomes.
Stress has been defined as any uncomfortable emotional experience accompanied by predictable biochemical, psychological and behavioural changes directed towards adaptation to or removal of the stressor.4 While positive psychological stress or eustress can lead to motivation and appropriate action, negative psychological stress or distress can have significant impact on neuroendocrine, cardiovascular, immune and central nervous systems.4 Indeed, diabetes and its comorbidities are associated with significant psychological distress.5 On one hand, chronic stress, negative mood and cognition are strong risk factors for development of obesity, diabetes, hypertension and cardiovascular disease.6 At the same time, living with diabetes requires significant adaptation and excellent coping skills. There is a high prevalence of anxiety and depression in diabetic individuals and depression often tends to be severe but ignored, unrecognised and unaddressed.7 Using the Diabetes Distress Scale, Fischer et al. reported a high prevalence of diabetes distress among adults with type 2 diabetes and this was associated with poorer outcomes in relation to lifestyle modification, self-efficacy and glycaemic control.8 Additionally, there may be associated eating disorders and substance abuse. Diabetic individuals often report disease-related stigmatisation, in both personal and professional domains.9 Hence, mind–body therapies that aim at physical, mental and emotional wellbeing may have a significant role in reduction of diabetes distress, improvement of health behaviours and overall wellbeing of individuals living with diabetes.
We performed a PubMed search for the terms ‘meditation’, ‘mindfulness meditation’, ‘mindfulness’, ‘mindfulness-based stress reduction’ or ‘mindfulness-based intervention’ and ‘diabetes’ from January 1984 to November 2017. The search revealed 154 articles. After reading through the abstracts, we selected controlled trials of mindfulness-based interventions in diabetes for the purpose of this review.
Meditation – historical perspectives
Meditation has been practiced since ancient times, with the earliest references going back to the Vedas. It has formed an integral part of Eastern religions including Buddhism, Hinduism, Jainism and Sikhism.10 Meditation has had varied interpretations in different cultures and includes a wide range of different techniques and practices that ultimately involve self-regulation of the mind.11 Transcendental meditation constitutes an important component of several Eastern religions such as Hinduism, Buddhism and Jainism. Meditation practices such as mindfulness, loving kindness and insight form the fundamentals of Buddhist meditation. The ancient Indian science of yoga, the Chinese arts of qigong and tai chi and the Japanese art of reiki are meditation-based movement therapies. Western religions have also incorporated meditation into their practices, such as hesychasm, Western Christian meditation and the Islamic practice of Dhikr.
Meditation was primarily considered a tool for the attainment of spiritual salvation and practised by saints and ascetics. However, scientific enquiry into meditation began in the early 1900s and the approach focused on secular meditation techniques as a strategy for stress reduction, mental relaxation and self-improvement. Meditation is a state of contemplation, focused attention and reflection aimed at improving spiritual, mental and emotional wellbeing. While there has been no uniformly accepted definition and the term ‘meditation’ may have different interpretations, the following definition proposed by Walsh and Shapiro has been widely accepted in clinical psychology:
‘[M]editation refers to a family of self-regulation practices that focus on training attention and awareness in order to bring mental processes under greater voluntary control and thereby foster general mental well-being and development and/or specific capacities such as calm, clarity, and concentration.’11
The core components of meditation practice include focused attention, self-regulation of emotions and self-awareness.
Over the decades, several meditation-based techniques have been developed and incorporated into cognitive and psychological therapies. These include mindfulness-based stress reduction (MBSR), mindfulness-based cognitive therapy (MBCT), mindfulness-based art therapy (MBAT), acceptance and commitment therapy (ACT), dialectical behaviour therapy (DBT) and mode deactivation therapy (MDT), among others. Mindfulness-based stress reduction is a well-developed, 8-week program that incorporates mindfulness meditation and yoga.12–14
Mindfulness meditation
Mindfulness is the psychological process of bringing one’s attention to the present moment. Mindfulness meditation refers to the state of awareness that arises through paying attention, on purpose, in the present moment, non-judgementally.12 ‘Mindfulness of breathing’ is a simple practice where the practitioner can sit in any position and focus on the breath as he/she inhales and exhales. Steady attention is paid to the breath coming in and out, and if the mind drifts away to any sensation, thought or emotion, it is gently brought back to the observation of breath. The awareness can, similarly, be focused on body parts and sensations, physical functions such as walking or internal experiences such as thoughts, feelings and emotions.14 The practitioner simply observes all feelings/thoughts/sensations that arise, both pleasant and unpleasant, without dwelling on them or judging them. Transcendental meditation involves focusing the mind silently on a specific mantra (repetition of words, syllables or phrases). Loving kindness or equanimity meditation involves the cultivation of compassion for self and others.
The mind is thus trained in meditation to become aware of the outer world and the inner mental and emotional state, in the present moment, without attempts to control or suppress it or respond to it.15 Mindfulness meditation, transcendental meditation and meditative movement therapies such as yoga, tai chi and qigong have received the greatest attention in clinical psychology and healthcare.16,17 Mindfulness meditation has been incorporated into psychology and psychiatry practices for several chronic disorders pertaining to both mental and physical domains. Benefits have been demonstrated in depression, anxiety, eating disorders, sleep disorders, fibromyalgia, chronic pain syndrome, rheumatoid arthritis, cancer, HIV/AIDS, diabetes, hypertension, cardiovascular diseases and substance abuse.18–23
Role of mindfulness meditation in diabetes care – the evidence
The practice of meditation is associated with greater voluntary control of the mind and emotions and cultivation of positive mental attributes such as calmness, serenity, concentration, joy and love and reduction of negative emotions such as anxiety, depression, anger, fear or hatred.11 Thus, it can reduce reaction to stress and improve coping skills, attention, awareness, memory, sensory perception and cognitive regulation of emotions and help develop a more coherent sense of self and identity.24 In a Swedish population-based study, the practice of mindfulness in general was associated with an improved perception of wellbeing among individuals.25
Evidence – basic science
Meditation seems to have effects on multiple regions of the brain, involving large-scale neural networks in the cortex, subcortical grey and white matter, cerebellum and brainstem. These have been extensively reviewed by Tang et al.26 Several cross-sectional studies and short-term longitudinal studies using structural and functional magnetic resonance imaging (MRI) have reported both functional and structural changes in brain in long-term meditators as well as beginners of meditation practice. Such neuroplasticity changes have been reported in the frontopolar cortex, sensory cortices, anterior cingulate cortex, midcingulate cortex, orbitofrontal cortex, insula, superior longitudinal fasciculus, corpus callosum, hippocampus, temporoparietal junction, frontolimbic network and default mode network structures.26–27 The neuroplasticity changes reported include increased activation of certain regions and reduced activation of others, increase in cortical thickness and grey matter density and volume.26 However, it is not clearly understood how these functional and structural changes relate to improvements in cognitive, affective and social functions and overall wellbeing. Some of the neuroplasticity changes that have been related to improved attention regulation, emotional regulation and self-awareness include:
- Attention regulation: anterior cingulate cortex and fronto-insular cortex are involved in attention regulation and cognitive processing. Enhanced activation of the anterior cingulate cortex has been reported in long-term meditators during focused attention.28 Other regions demonstrating enhanced activation in relation to attention include the prefrontal cortex and parietal attention regions. Mindfulness meditation has also been associated with greater cortical thickness and decreased age-related decline in grey matter volume of putamen.26
- Emotion regulation: meditation is associated with reduced emotional reaction and negative affect to stressors, reduced physiological reactivity and faster return to positive mood state. Mindfulness results in decreased activation of amygdala in response to emotional stimuli and has been associated with greater activation of dorsomedial and dorsolateral prefrontal cortex in beginners, but the reverse is seen in experienced meditators. This may be because beginners need to overcome habitual ways of reacting to emotions and therefore exhibit greater activation of prefrontal cortex.26 Functional alterations have also been demonstrated in regions involved in motivation and reward process, including increased activity in the putamen and caudate during resting state.
- Self-awareness: mindfulness is associated with a more positive representation of self. The default mode network which involves midline structures, including medial prefrontal cortex, posterior cingulate cortex, anterior precuneus and inferior parietal lobule, is widely believed to be involved in self-referential processing. Functional MRI has demonstrated reduced activity of the default mode network in meditators.28 Increased connectivity of default mode network with ventromedial prefrontal cortex has been seen in experienced meditators and this may be involved in greater cognitive control. Mindfulness is also associated with increased awareness of the present moment. Insula has been shown to be strongly activated following mindfulness training and experienced meditators have increased cortical thickness of insula.26
- Stress reduction: a potential mediator of the benefits of mindfulness on brain function seems to be stress reduction.26 Increased brain activity in the prefrontal cortical regions involved in stress regulation and decreased activity in regions involved in fight-or-flight response, such as the amygdala and anterior cingulate cortex, has been demonstrated after short-term meditation sessions. Several studies have also demonstrated a positive effect of mindfulness on biomarkers of stress such as serum cortisol.29 Cortisol and brain-derived neurotrophic factor may be the facilitators of these functional and morphological changes. The prefrontal cortex, hippocampus, amygdala and other areas are vulnerable to stress-induced functional and structural remodelling. Meditation is associated with reduced sympathoadrenal activity and an increase in parasympathetic tone and reduced secretion of stress hormones. There is also reduced secretion of inflammatory markers such as interleukin-6, C-reactive protein and tumour necrosis factor α.27,30
It remains to be determined how the neuroplasticity changes seen in long-term meditators differ from beginners. Using functional near-infrared spectroscopy, Gundel et al. demonstrated that meditation experts had different lateralisation patterns in resting state, which associated with amplified left hemisphere and in response to the sound of a meditation bowl, which was associated with amplified right hemisphere. Even beyond the meditative task, areas including Brodman’s area 39, 40, 44 and 45, had increased brain activity, thus suggesting that meditation induced possible long-term changes in brain, explaining its positive effect on health.31
Evidence – clinical science
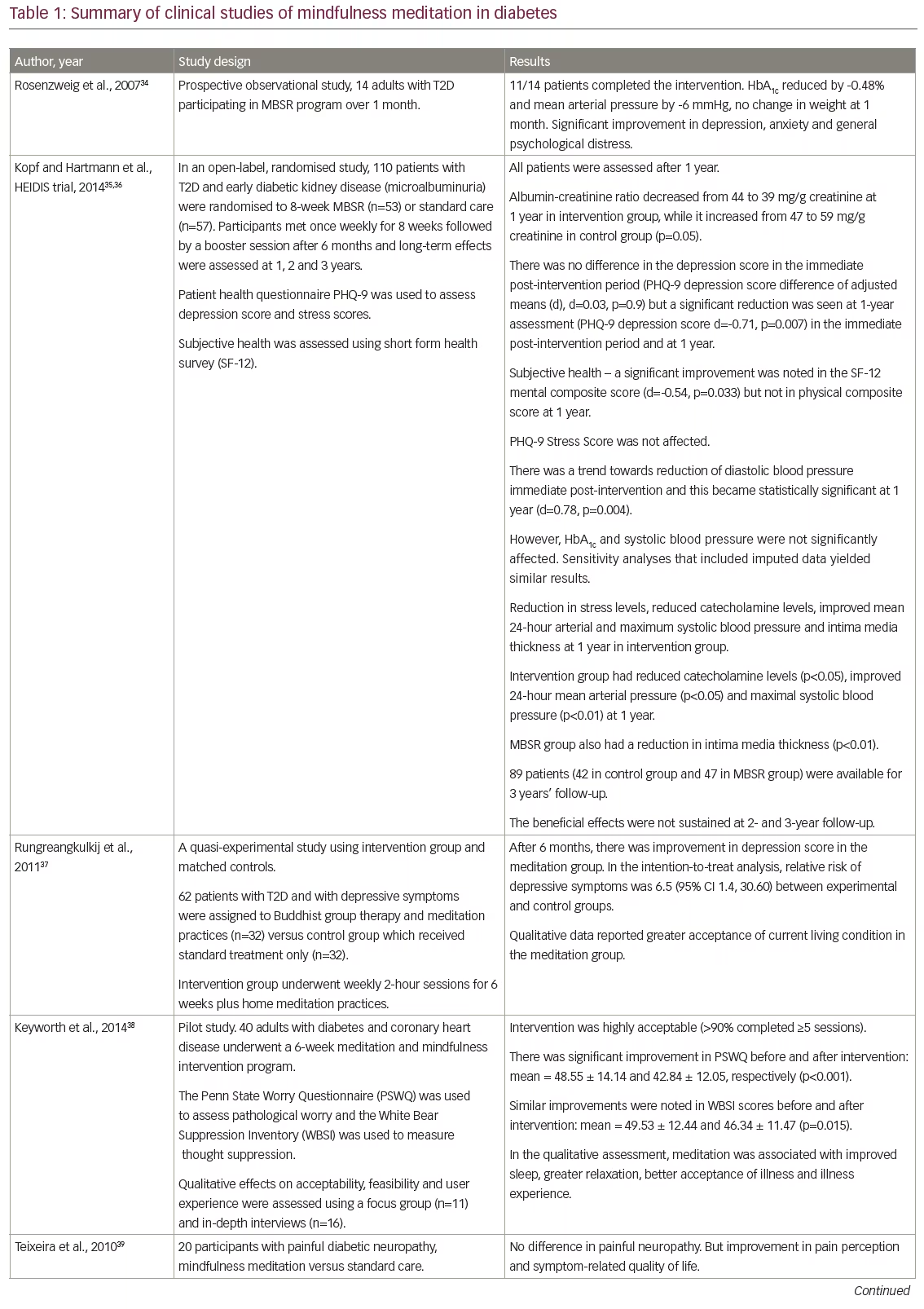
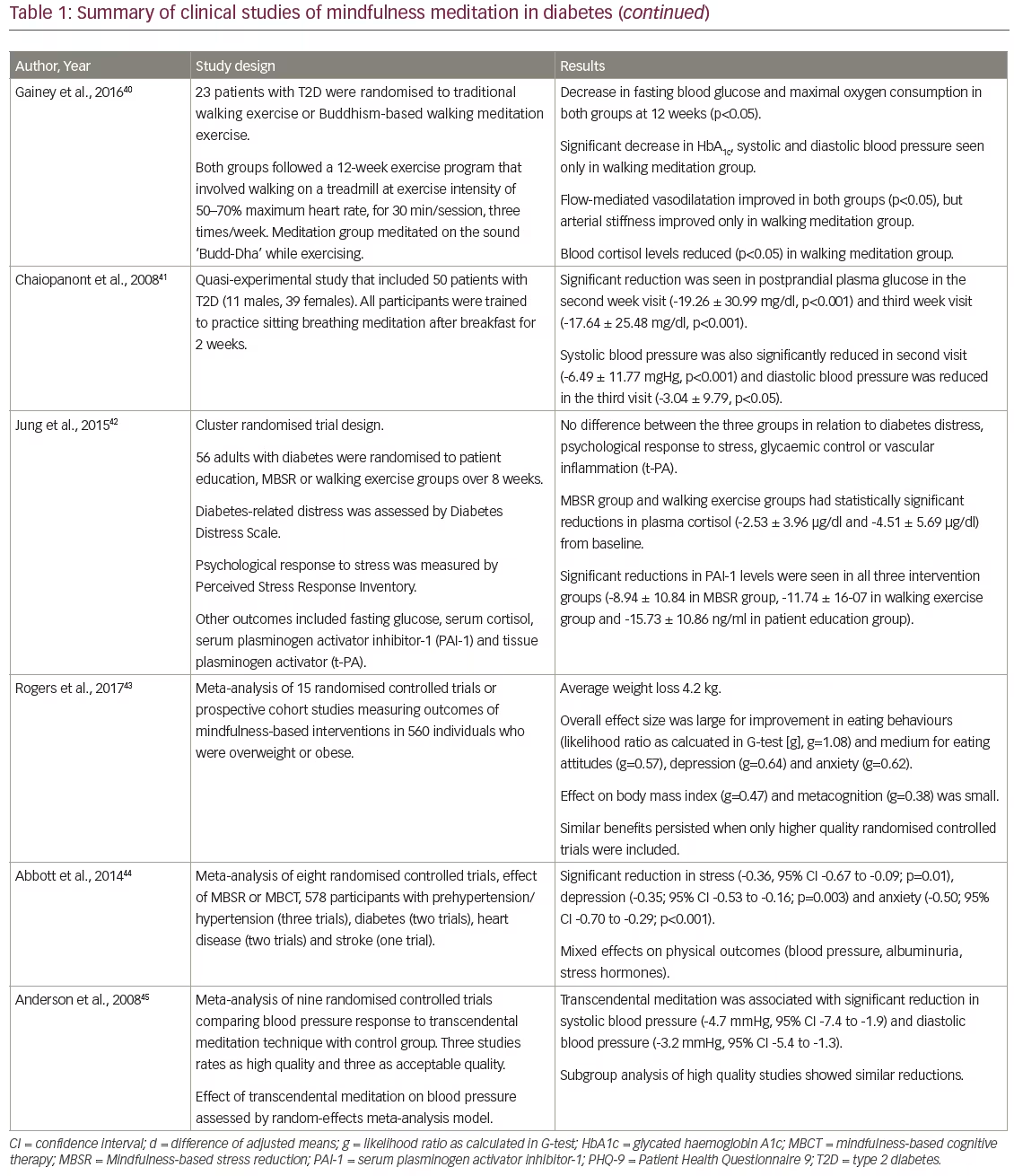
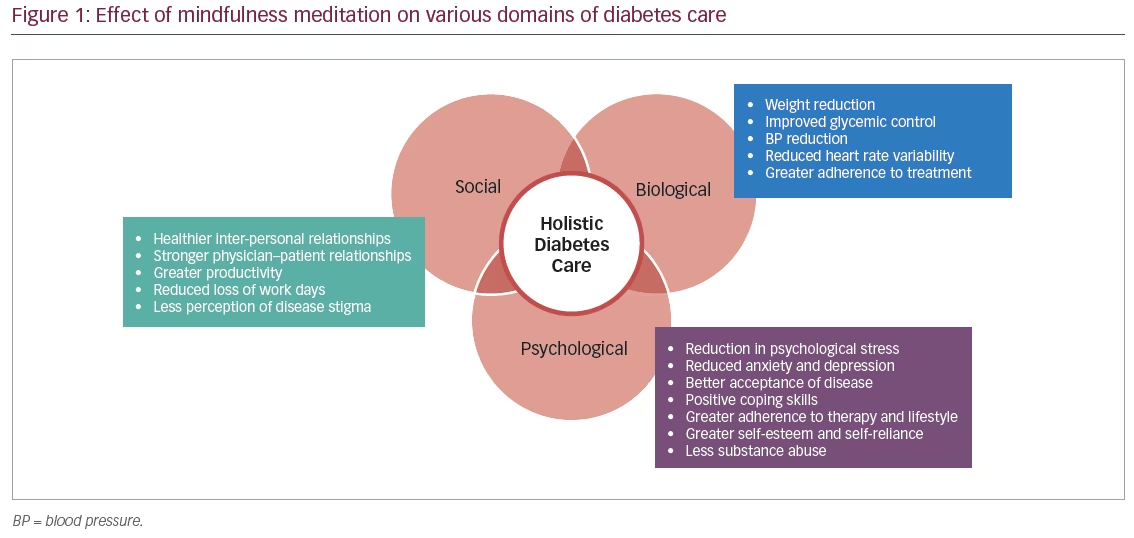
Meditation practices such as MBSR can be an important group intervention in patients with diabetes to reduce psychological distress, improve mood and develop positive coping skills.32 They have the potential to influence the patient experience and perception of the burden of diabetes and can help encourage health behaviours related to primary, secondary and tertiary prevention.33 Randomised studies have demonstrated that MBSR resulted in significant improvements in depression and anxiety and improved self-care behaviour. In Table 1, we enumerate the effects of mindfulness-based strategies on diabetes and related outcomes reported in various studies. Mindfulness-based stress reduction was associated with significant improvements in diabetes distress, weight, glycaemic control and blood pressure control. Thus, it results in reduced heart rate variability, vascular resistance and ventricular workload.46,47 Loving kindness meditation can lead to improvements in relationship satisfaction and prosocial behaviour. A recent systematic review evaluated the evidence from clinical trials examining the effect of mind-body therapies as adjunctive complementary strategies in metabolic syndrome. Meditation-based therapies were associated with significant improvements in blood pressure, glycaemic control, body weight and waist circumference.48 In a meta-analysis of eight randomised controlled trials involving hypertensive subjects, transcendental meditation was associated with a reduction in systolic blood pressure of 4.7 mmHg and diastolic blood pressure of 3.2 mmHg compared to control groups.45 Significant reductions in body weight have been reported in a meta-analysis of mindfulness-based interventions for weight loss and this may have clinical relevance in diabetes care.49 To summarise, mindfulness interventions have demonstrated impact on a broad range of outcomes relating to all domains of holistic care in diabetes – biological, psychological and also social, as depicted in Figure 1.
An important question that needs to be addressed is the amount of mindfulness intervention necessary to experience benefits. Even three to four brief sessions of 5–10 minutes of guided meditation have been shown to reduce negative affect, but most studies have been conducted over 4–8-week programs.18 Moreover, most studies are limited by small sample size, short duration and a lack of adequate control group. Therefore, these studies carry a high risk of bias. In a meta-analysis, it was demonstrated that there existed a strong bias towards publication of positive results in meditation studies.28 Additionally, it can be argued that several trials of physical activity and lifestyle intervention are themselves associated with significant improvements in metabolic parameters and overall wellbeing.
Unwanted effects of meditation
It is important to evaluate the possible negative effects of mindfulness practices and identify individuals who may succumb to such unwanted effects before recommending widespread use of mindfulness meditation in diabetes. Some studies have evaluated the unwanted effects of meditation.50,51 These included emotional pain, self-criticism, fear, anxiety, lack of motivation, boredom, disorientation, insomnia, feeling of alienation or lacking something.50 Most investigators have suggested that these adverse effects are mild and transitory and did not lead to discontinuation of meditation and may be a part of the psychotherapeutic effect.50 Rarely, individuals may experience more severe adverse reactions with more intensive mindfulness training such as the triggering of major depressive episode or psychosis,52 post-traumatic stress disorder,53 and epileptic attacks.54 Hence, caution is needed when initiating people with psychosis, seizures, post-traumatic stress or severe depression into mindfulness.27 However, most clinical studies involve low intensity meditation practices and such adverse effects are not often reported unlike with more intensive traditional meditation techniques which can be psychologically challenging. Future interventional studies should carefully assess the negative effects of meditation and identify individuals who are more likely to benefit from mindfulness interventions.
Meditation in modern medicine – eminence
Mind and body practices including meditation are being used by a large number of diabetic patients in many countries of South East Asia as complementary strategies.55 The Indian national guidelines for management of diabetes recommend yoga as complimentary therapy which has beneficial effects on various metabolic parameters.55 WHO categorises ‘mind–body medicine’ which includes meditation, prayer, mental healing, yoga, tai chi, art therapy, music therapy and dance therapy as Complementary and Alternative Medicine. In a scientific statement issued in 2013, the American Heart Association recognised that there was Class II B (Level of Evidence B) evidence for recommending transcendental meditation and biofeedback approaches as adjunct to pharmacological therapy of hypertension. The evidence for other meditation techniques and yoga was rated as Class III (Level of Evidence C).56 In a recent position statement, the American Heart Association acknowledges that meditation may be considered as an adjunct to lifestyle modification and pharmacological treatment in cardiovascular risk reduction.57
Conclusion
Mindfulness meditation-based strategies are simple, easy to grasp and practice and do not incur additional cost. Moreover, many individuals may not be able to engage in moderate to vigorous physical activity. This may be due to physical limitations such as osteoarthritis, morbid obesity, cardiovascular or respiratory disease. Meditation-based therapies may offer immediate positive benefits in such individuals. It may also help improve self-care behaviour, self-reliance and self-control. This would result in better quality of life. Therefore, the role of mindfulness meditation needs to be evaluated further in well-conducted studies.
‘If you meditate earnestly, pure in mind and kind in deeds, leading a disciplined life in harmony with the dharma, you will grow in glory. If you meditate earnestly, through spiritual disciplines you can make an island for yourself that no flood can overwhelm.’ – Guatama Buddha1







