Type 1 diabetes mellitus (T1DM) is the most common type of diabetes affecting children.1–3 Despite increasing awareness of early presentation of diabetes, a high number of children newly diagnosed with T1DM still present with diabetic ketoacidosis (DKA).4–7 DKA in children carries higher risk of mortality and morbidity compared to adults.8
Cerebral oedema is the most common cause of acute neurological deterioration, which occurs in 3–10 paediatric patients per 1000 cases of DKA.9,10 Ischaemic and haemorrhagic brain injury, although recognised, is uncommon among paediatric reports, with only 10% of the intracerebral complications post-DKA attributable to ischaemic or haemorrhagic brain infarction.11,12 To our knowledge to date, only 14 patients with haemorrhagic stroke post-DKA were reported.8,12–16
We present the case of a patient newly diagnosed with T1DM with severe DKA who developed an ischaemic haemorrhagic stroke and reiterate the importance of correct management.
Case presentation
A 10-year-old girl presented with polyuria, polydipsia and lethargy for 2 weeks and vomiting for 2 days. There was no significant past medical history. Family history revealed a history of hypothyroidism in the mother who was diagnosed in her 20’s. She was tachycardic with poor peripheral perfusion, but normotensive (blood pressure 117/68 mmHg). Glucometer reading was ‘HI’, which corresponds to glucose level of more than 29 mmol/L, with venous blood pH 7.011 and bicarbonate 6.4 mmol/L. Urinalysis revealed marked ketonuria. Two fast boluses of 20 ml/kg (total 40 ml/kg) normal saline were given each over 20 minutes. She was immediately transferred to another hospital and upon arrival became drowsier, and restless with reduced Glasgow Coma Score (GCS) and hence was intubated. At the second hospital, her fluids and glucose values were corrected gradually with fluid maintenance (0.9% normal saline) and correction based on 7.5% dehydration (minus boluses, given over 48-hour duration). There were no electrolyte abnormalities and potassium supplements were added into the intravenous maintenance fluid to avoid hypokalaemia. Insulin infusion at 0.1 unit/kg/hour was commenced right after the start of fluid maintenance and the intravenous fluids were discontinued 48 hours after admission.
The patient was extubated within 24 hours of admission. Her ketosis and acidosis resolved before conversion to basal bolus subcutaneous insulin at approximately 48 hours of her initial presentation. However, about 48 hours after admission, she had reduced GCS 11/15 (E4M5V2) with an expressive aphasia. All four limbs showed upper motor neuron signs with quadriparesis affecting the lower limbs (Medical Research Council (MRC) power 2/5 bilaterally) more than upper limbs (MRC power of 3/5 bilaterally). Initial computed tomography (CT) brain scan did not show cerebral oedema. In view of the deteriorating GCS, a trial of intravenous mannitol was given but no significant improvement was seen.
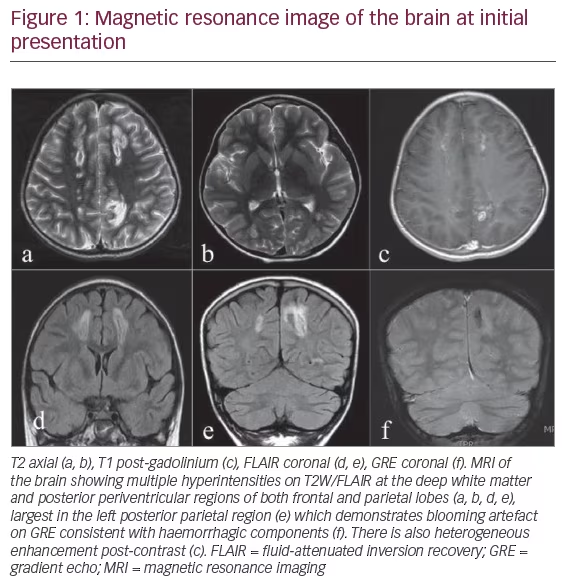
She was transferred to our facility which offers both paediatric endocrinology and paediatric neurology input for further management. Magnetic Resonance Imaging (MRI) of the brain (3T SIGNA™, GE Healthcare, Milwaukee, WI, US) at initial presentation showed multiple heterogeneously enhancing hyperintensities on T2-Weighted/Fluid-attenuated inversion recovery at the posterior periventricular and deep white matter regions of both frontal and parietal lobes consistent with ischaemic haemorrhagic infarction of the deep white matter in the vascular watershed regions (Figure 1). Magnetic Resonance Angiography (MRA) of the intracranial vessels was unremarkable. Her HbA1C at presentation was 11.5% with low c-peptide at one month follow up. Baseline thyroid function, autoimmune, metabolic and thrombophilia screen were all normal. Echocardiogram showed no vegetation or valvular lesions. She was discharged with some residual limb weakness after two weeks of hospitalisation.
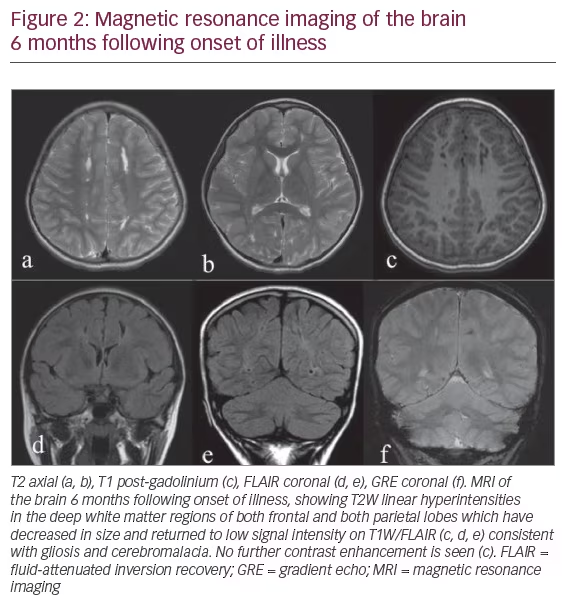
A repeat MRI and MRA 6 months later showed chronic infarcts and residual gliosis at the previously described sites (Figure 2). At the 26-month follow-up, a near-full neurological recovery with residual mild left lower limb weakness (MRC power of grade 4 ± 5) and brisk reflexes were noted. A formal intelligent quotient assessment 1-year post event was normal with no evidence of language, perceptual reasoning, working memory or attention dysfunction.
Discussions
Our case report expands the phenotype of the uncommon manifestation of haemorrhagic stroke associated with DKA. The majority of reports describe haemorrhagic infarction in the basal ganglia. To our knowledge, our case report is the first to show extensive watershed haemorrhagic infarction over the frontal-parietal lobes extending into the deep white matter.
We highlight the importance of monitoring a child for cerebral complications during the period of DKA up to about 48 hours after admission. Cerebral autoregulation is a mechanism that maintains a stable cerebral blood flow for a certain cerebral metabolic rate in spite of cerebral perfusion pressure fluctuation.17 As the cerebral autoregulatory mechanisms may not be well develop in children; this may predispose a child with DKA to cerebral oedema18 and other cerebral complications. Ma et al. reported that impaired cerebral autoregulation was common early during the treatment of DKA. Although the majority improved during treatment, 17% of them still had impairment between 36 to 72 hours after commencement of insulin therapy and the observed impaired cerebral autoregulation appears specific to the DKA process in children with T1DM.19
The mechanism of cerebral haemorrhage is unclear and could be secondary to a combination of intracranial hypertension and systemic hypotension resulting in cerebral infarction usually at the watershed arterial territories. Diabetic ketoacidosis is also pro-inflammatory causing vascular endothelial perturbation and dysfunction of the coagulation system8 predisposing to a higher risk of thrombus and haemorrhage.
This case illustrates the difficulty in differentiating a DKA patient with global neurological impairment due to decompensatory acidosis, cerebral oedema or primary stroke. As the neurological presentation of cerebral oedema and primary stroke can be similar, we recommend that clinicians have a high index of suspicion of acute stroke particularly if brain CT shows no evidence of cerebral oedema. Petzold et al. have recommended neurological monitoring especially in the first 24 hours.20 Our case supports this and also suggests that neurological monitoring should continue for at least 48 hours, especially in severe DKA. In any patients with DKA and neurological impairment, early brain MRI is important to diagnose a primary stroke.
Judicious initial fluid resuscitation and correction of dehydration are also important to ensure optimum DKA management. Too much and too rapid fluid administration may predispose a child to intracerebral complications whereas too little may prolong DKA resolution. Dunger et al. and the International Diabetes Federation (IDF)/International Society for Pediatric and Adolescent Diabetes (ISPAD) 2014 Guidelines outlined the initial fluid resuscitation in patient presenting with shock by giving bolus of 10–20 ml/kg of normal saline over 1 to 2 hours. A repeat bolus is indicated only if the circulation is not restored but should not exceed 30 ml/kg.21,22 However, there are controversies regarding the association between the rate of fluid or sodium administration used in the DKA treatment and the development of cerebral oedema23,24 and other intracerebral complications. The recently completed Pediatric Emergency Care Applied Research Network (PECARN) Fluid Therapies Under Investigation in DKA (FLUID) study is the first prospective randomised trial that evaluated the fluid regimens for DKA in children. This multicentre study, which consisted of four treatment arms, evaluated the effects of rehydration rate and fluid sodium content on neurological status during DKA treatment, the frequency of clinically overt cerebral oedema and long-term neurocognitive outcomes.23
Apart from fluid management, guidelines have also outlined recommendations on insulin therapy as well as electrolyte management to ensure optimum treatment of DKA and reduce the risk of complications. Insulin therapy in DKA should begin with a rate of 0.05–0.1 unit/kg/hour about 1–2 hours after starting fluid replacement therapy.21,25 Hypokalaemia is common in DKA, necessitating potassium replacement irrespective of the serum potassium level unless renal failure is present. 21,25 As for now, the guidelines for patients with DKA and stroke are lacking, including the best rehydration rate, parameters for the use of thrombolytics and other medications and monitoring schedule.26 Thrombolysis for the treatment of paediatric stroke remains controversial, although isolated paediatric cases have reported successful outcomes when administered intravenous tissue plasminogen activator for acute treatment of ischaemic stroke.27 Similarly, there is also no clear guideline on the management of children with haemorrhagic stroke. Guidelines for adults recommend cautious reduction of extremely high blood pressures. Recombinant factor VIIa has shown some benefit in decreasing recurrence but only within clinical trials. These guidelines however refer to different aetiologies of haemorrhage rather than those seen in children or patients with DKA. Surgical decompression may be warranted in large haemorrhages compressing the neurovascular structures.8
In conclusion, our case reiterates the importance of clinicians to be vigilant of cerebral complications including ischaemic haemorrhagic stroke in patients with DKA. We suggest that in severe DKA, close neurological monitoring should be performed for at least 48 hours and prompt brain neuroimaging (MRI) requested in any child with neurological impairment (but normal CT brain) to rule out acute stroke.













