Non-alcoholic fatty liver disease (NAFLD) consists of non-alcoholic fatty liver (NAFL) and non-alcoholic steatohepatitis (NASH). It is unclear which specific patients progress from NAFL to NASH and, ultimately, to cirrhosis. However, there is general consensus that, for those patients who do progress to cirrhosis (fibrosis stage 4), there is an increased risk of liver-related complications (liver failure, liver cancer) and cardiovascular disease.1,2
The global prevalence of NAFLD is estimated to be approximately 25% of the population with an estimate of NASH of between 1.5% and 6.45%.3 Reports state that the progression of NAFL to NASH occurs in approximately 20–25% of cases, and that 20% of those patients will ultimately develop cirrhosis.4 Current published data suggest that the incidence of NAFLD is greatest in Hispanics, and lowest in African Americans.5 No clear consensus has emerged regarding the factors that promote the progression of patients from NAFLD to NASH. What is clear, is that the development of liver fat content of >6% leads to metabolic changes in humans, including insulin resistance and hypertriglyceridaemia.6
NASH is a large global disease burden; however, the reality is that the at-risk patient population remains largely undiagnosed. Much of this revolves around limited physician awareness of the disease outside of hepatologists, a relatively small specialty group of physicians. Physician groups that are poised to diagnose and manage these patients are endocrinologists, internists and primary care physicians. These clinicians see many patients with comorbid risk factors associated with NASH.
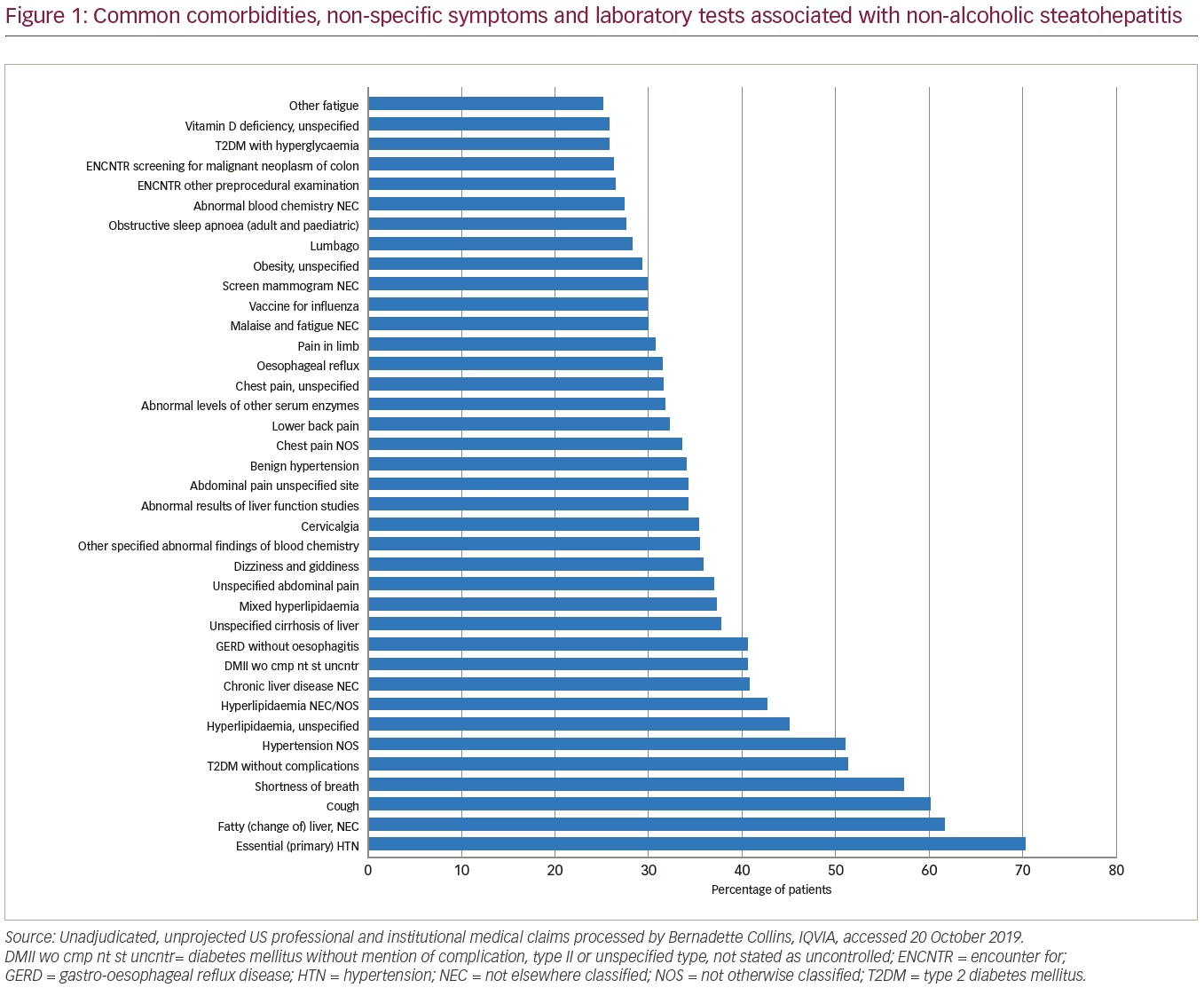
The IQVIA proprietary P360 database in the USA (as accessed by Bernadette Collins, 20 October 2019), contains 421,000 patient records; when reviewed, using the diagnosis of NASH with the presence of a liver biopsy, it notes that the median age for diagnosis is 56–57 years, and that 62% of the patients are female. An analysis of comorbidities in the same claims database notes common comorbidities of type 2 diabetes mellitus (T2DM), hypertension, hyperlipidaemia and obesity, amongst other more non-specific symptoms and laboratory tests (Figure 1).
The clinical development space in NASH is very competitive, globally. Recruitment rates for NASH clinical trials have been low, and many trials have been delayed in their completion. The majority of principal investigators, to date, have been hepatologists. There remains tremendous opportunity for endocrinologists, internists and primary care physicians to assume the role of the principal investigator in NASH clinical trials, in addition to the diagnosis and management of these patients.
The objective of this literature review and assessment of IQVIA’s proprietary claims-based database of ICD-10 codes, patient encounters and treatments, is to demonstrate how this disease fits squarely into the clinical realm of the endocrinologist, internist and primary care physicians, based on disease pathophysiology, current off-label treatments and comorbid disease states. The review also will present current professional endocrinology guidelines related to NAFLD, a proposed patient screening algorithm, suggestions for the operational incorporation of NASH into daily clinical practice, and a review of the opportunities in clinical research for many physician specialties.
Non-alcoholic steatohepatitis pathophysiology
The exact pathophysiology of NASH remains in question. Some believe that the disease process is a ‘two-hit’ insult to the liver, while others tout a ‘multiple parallel hit’ pathway. The two-hit process states that there is an initial accumulation of free fatty acids in the liver, which are derived from visceral adipose tissue.7 Visceral adipose tissue accounts for approximately 6–20% of human adipose tissue; subcutaneous adipose tissue accounts for approximately 80–90% of whole body-fat tissue.8 Within the subcutaneous adipose tissue compartment is a superficial subcutaneous compartment and a deep subcutaneous compartment. The accumulation of fatty acids in the deep subcutaneous compartment also shows a similar positive association with insulin resistance in NASH as the visceral adipose tissue compartment.9
The accumulation of free fatty acids leads to insulin resistance. Loss of adipose tissue responsiveness to insulin plays a major role in the pathophysiology of NASH. Failure of insulin to inhibit triglyceride lipolysis in insulin-resistant states leads to an oversupply of free fatty acids to the liver, excess hepatic triglyceride synthesis, and intracellular accumulation of toxic lipid products that impair insulin signalling and activate inflammatory pathways.10 This is followed by progression to hepatic inflammation (steatohepatitis), leading to an accumulation of oxygen free radicals, mitochondrial dysfunction and formation of adipokines, all of which result in hepatic tissue damage and fibrosis. Recent data suggest that adipose-based insulin resistance is responsible for the activation of hepatic macrophages and the inflammatory process in the liver. This process is independent of a patient’s comorbid disease states of diabetes and/or obesity.11
The multiple-hit pathway also includes the free fatty-acid accumulation and inflammation described in the two-hit hypothesis, but believes that the gut produces factors that are important in initiating and advancing hepatic inflammation. The gut-related damage to the liver is derived from cytokine injury and physiologic stress on the hepatic cellular endoplasmic reticulum.12 This multiple-hit hypothesis stresses the alterations in the gut microbiome as important in the NASH injury process.
These hypotheses are not all inclusive as to the explanation of NASH pathophysiology. Recent work has confirmed that there is a predisposition to NASH and to significant hepatic fibrosis in people with alterations in the PNPLA3 and TM6SF2 genes.13 Although the exact mechanism of this increased predisposition and severity is unknown, it is believed to centre around the packaging and export of triglycerides from the hepatocyte. Interestingly, these effects are not related to the presence of insulin resistance or obesity.13
The concern with NASH is that it may progress to cirrhosis with the complications of liver failure, including the risk for developing hepatocellular cancer. However, liver dysfunction, failure and cancer are not the leading cause of death for patients with NASH; the leading cause of death is cardiovascular disease. People with NAFLD have a higher risk of developing severe coronary artery disease compared with those who do not have NAFLD.14 The presence of fibrosis in patients with NASH is predictive of the occurrence of cardiovascular events.15 High calcium scores have been identified in the coronary arteries of patients with NAFLD, independent of metabolic syndrome or obesity.16 Furthermore, medical complications associated with T2DM are also higher in patients with NAFLD. In a study of 2,100 patients with T2DM, there were increased rates of chronic kidney disease (odds ratio [OR] 1.87) and retinopathy (OR 1.75) in those with T2DM and NAFLD, compared with those with T2DM without NAFLD.17
Non-alcoholic steatohepatitis and the endocrinologist, internist and primary care physician
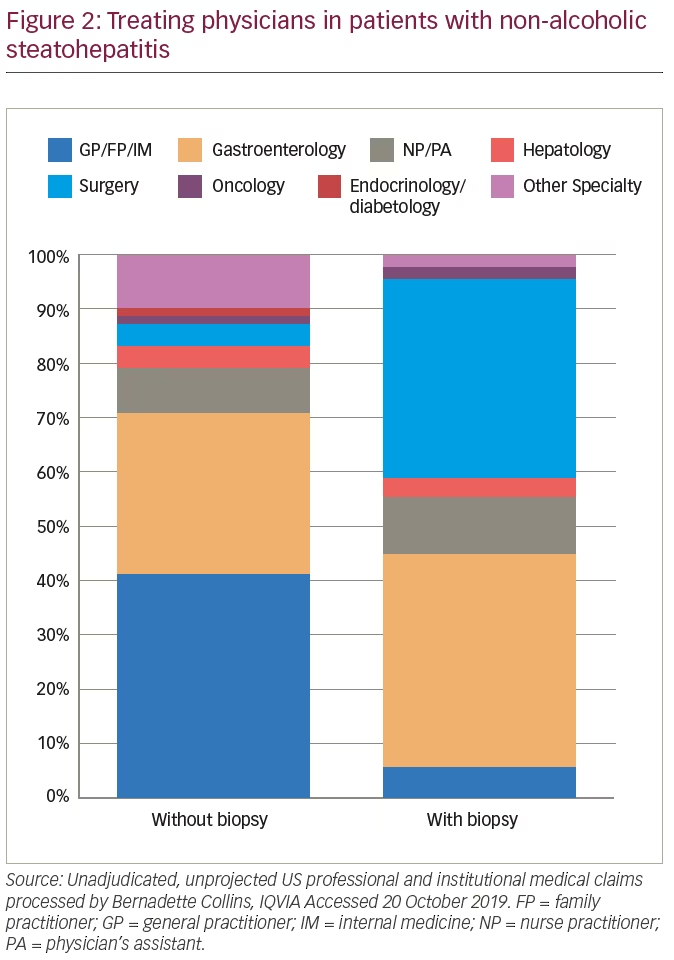
Hepatologists commonly diagnose and treat patients with NASH. However, endocrinologists, internists and primary care physicians are specialties that, in general, often see patients with many of the comorbidities associated with NASH (hyperlipidaemia, obesity, T2DM). These physician groups have recently become aware of NASH as a potential common disease entity in their practice setting. Figure 2 depicts which physician specialities are involved in the diagnosis of NASH, based on a large ICD-10 claims database in the USA.
It is becoming increasingly clear that endocrinologists, internists and primary care physicians are making the link between commonly seen disease states and NAFLD, as understanding of NAFLD and its disease history increases. The best-known link is between T2DM and NAFLD. Insulin resistance leads to decreased suppression of gluconeogenesis, a reduction in glycogenesis, and a higher percentage of liver and peripheral tissue fat accumulation.18 There is an almost two-fold increased risk of incident T2DM in patients with NAFLD.19 In a prospective observational study of patients with T2DM, there was a 69% prevalence of NAFLD when using ultrasound of the liver to determine the presence of steatosis.20 A separate systemic review noted the presence of NAFLD in 50–75% of patients with T2DM.21 In people with T2DM, higher glycated haemoglobin (HbA1c) is associated with a higher incidence of hepatic steatosis.22 When evaluating the progression to hepatic fibrosis in patients with NASH, T2DM and hypertension are the two most powerful independently associated risk factors.23,24 Even in patients without a diagnosis of diabetes, but who demonstrate insulin resistance, there is a higher risk for developing fibrosis of the liver.25 Compared with the healthy population, it has been reported that people with T2DM have 2.5-fold increase in the risk of death from cirrhosis.26 Chronic liver disease and/or liver cancer are the fourth leading cause of death in patients with T2DM.26
Non-alcoholic steatohepatitis and commonly associated co-morbidities
Obesity is a very common comorbidity in patients with T2DM. Studies have shown that the median prevalence of NASH in patients who are obese is approximately 33%.27 Conversely it has been reported that 51% of patients with NAFLD and 82% of patients with NASH are obese.28 A study from France in 109 patients with NASH noted that gastric bypass surgery and weight loss led to a disappearance of histologic NASH in 85% of patients.29 A study from Cuba in patients diagnosed with NASH, evaluated the impact of weight loss by altering the patients’ diets. Thirty percent of patients lost ≥5% of their bodyweight. Of those who lost ≥5% bodyweight, a higher proportion experienced NASH resolution and a reduction in disease scores, compared with those who lost <5% bodyweight. Patients who lost ≥10% bodyweight were associated with even greater rates of improvement or resolution of steatohepatitis, based on histologically analysed biopsies.30
Hyperlipidaemia is associated with NAFLD and is common in patients with T2DM and/or obesity. In the Dallas Heart Study, magnetic resonance spectroscopy was used to measure liver steatosis. By this method, NAFLD was present in 45% of the Hispanic, 33% of the Caucasian, and 24% of the African American patients.31
Sex steroids have an impact on the development of NAFLD. Overall, the liver has a major impact on the biological actions of sex steroids. Testosterone and oestrogen, and their derivatives, are metabolized through the liver, which is also where sex hormone binding globulin is produced. The NHANES II study reported that NAFLD was twice as common in post-menopausal women compared with pre-menopausal women. In post-menopausal women receiving oestrogen treatment, there was a reduced incidence of NAFLD compared with post-menopausal women not receiving oestrogen therapy (OR 0.69).32 In women diagnosed with NASH, the severity of fibrosis was not only associated with being post-menopausal, but also with the number of years a woman had been post-menopausal.33
Polycystic ovary syndrome (PCOS) is a disease associated with insulin resistance and obesity.34 It clinically presents with increased serum androgen levels, amenorrhoea and multiple ovarian cysts. It is believed that 50% of women with PCOS have insulin resistance.35 A meta-analysis noted that there is a higher risk of NAFLD in patients with PCOS compared with controls (OR 3.93). From a pathophysiologic standpoint, insulin resistance seems to be the major risk factor for developing NAFLD in PCOS by stimulating the release of androgens.36 In a retrospective study of 63,000 women with PCOS compared with 121,000 age and body mass index-matched controls, there was a significant increase in the prevalence of NAFLD in the PCOS diagnosed group (OR 2.23, p<0.001), even when controlling for additional risk factors, such as the presence of diabetes or pre-diabetes.37
Testosterone plays a major role in insulin sensitivity and lipid metabolism.38 Low testosterone levels are commonly associated with men who have T2DM and/or are obese.39 Furthermore, men with low testosterone have a higher percentage of visceral fat.40 In a study of 495 men, those determined to have steatosis by liver ultrasound had lower serum testosterone levels.41 In a meta-analysis of almost 14,000 men, serum testosterone was lower in men with NAFLD, compared with men without NAFLD.42 In this same study, 5,840 women with higher serum testosterone levels were associated with a higher incidence of fatty liver disease. Studies with hypogonadal males using testosterone replacement therapy have noted a reduction in waist circumference, a reduction in body mass index and an improvement in insulin sensitivity.43
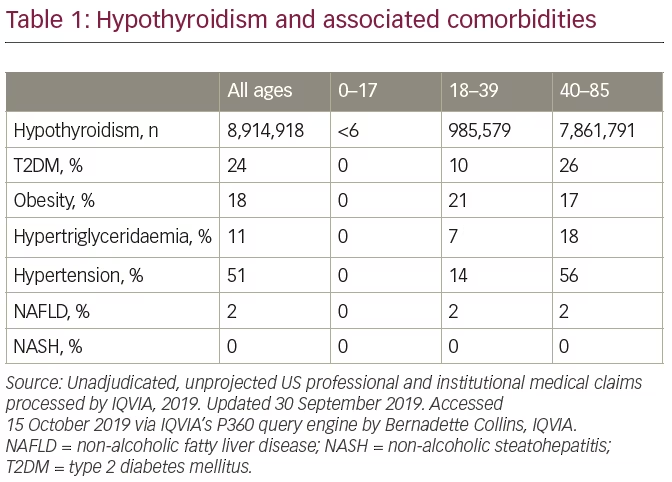
Disorders of the pituitary gland also have an association with NAFLD, specifically NASH. Growth hormone deficiency is associated with an increased risk of NAFLD, and is known to cause an increase in visceral fat content and insulin resistance.44 In a study of 160 obese patients with liver histology demonstrating NASH and a fibrosis score of ≥2, low growth hormone levels of <0.45 ng/mL were reported.45 Growth hormone deficiencies are more commonly treated by paediatric endocrinologists. Although the focus of the current review is adult NAFLD, paediatric NAFLD is also becoming a well-recognized disease entity.46 The thyroid gland plays an important role in the occurrence of hepatic lipogenesis. The effect is manifested through thyroid hormone receptors. Hypothyroidism decreases the uptake of free fatty acids from triglycerides.47 In some studies, hypothyroidism has been associated with NAFLD.48 Table 1 is an audit of a large, claims-based patient database evaluating the comorbidities associated with the diagnosis of hypothyroidism. Approximately one-fifth of patients with hypothyroidism are obese, and T2DM and hypertension become more common with advancing age. This underscores the number of comorbid metabolic-associated diseases in the hypothyroid patient population. However, the diagnosis of NAFLD and NASH was low, perhaps demonstrating that these diseases are under-recognized in patients with hypothyroidism.
Currently available treatment for non-alcoholic steatohepatitis
There are no approved pharmacologic therapies for NAFLD or NASH outside of India, where saroglitazar is approved for the treatment of NASH. Weight loss of >5% is associated with an approximately 30% reduction in liver fat content,49 and has also been shown to be associated with improvement or resolution of steatohepatitis.50 Other studies have shown that weight loss approaching 10% can improve the NASH Activity Score (steatosis, inflammation and hepatocyte ballooning) in liver histology, but has no impact on existing liver fibrosis.51 The biggest challenge with dietary therapy in clinical practice is the ability of patients to comply with dietary changes over a prolonged period of time.
It would be intuitive for clinicians to consider prescribing currently commercialized medications for the treatment of T2DM, obesity and or hypertriglyceridemia as a potential treatment for NASH. Potential T2DM medications that may be considered as candidates to treat NASH would include metformin, thiazolidinediones, glucagon-like peptide 1 (GLP-1) receptor agonists, dipeptidyl peptidase 4 (DPP-4) inhibitors and sodium–glucose co-transporter 2 (SGLT2) inhibitors. However, the data supporting the use of currently commercialized medications are limited.
To date, studies with metformin, DPP-4 inhibitors and SGLT2 inhibitors have shown no hepatic histologic improvement in patients with NAFLD.52–54 In the drug category of thiazolidinediones, there are a few prospective, randomized trials that have been published. A study with rosiglitazone in patients with biopsy-proven NASH demonstrated an improvement in hepatic steatosis but none of the other histologic features of NASH.55 A meta-analysis of randomized clinical trials using pioglitazone showed a benefit for patients with advanced NASH (F3, F4 fibrosis).56 Pioglitazone has been shown to reduce cardiovascular risk in patients with metabolic syndrome and T2DM.57 There is potential risk, however, as pioglitazone is associated with peripheral oedema, and may worsen heart failure. The American Association for the Study of Liver Disease (AASLD) notes pioglitazone may be a viable option for the treatment of NASH, but only after the risks and benefits of treatment are explained to the patient.58
GLP-1 inhibitors have been shown to reduce liver enzymes (aminotransferases) and steatosis.59 In a phase II clinical study of patients with NASH treated with liraglutide for 48 weeks, there were significant reductions of hepatic steatosis, hepatic cell ballooning and liver enzymes compared with patients who received placebo.60 A meta-analysis of six randomized trials in 4,442 patients with diabetes and NAFLD treated with liraglutide noted an improvement alanine aminotransferase (ALT) and a trend towards improvement in steatosis versus placebo, but no significant changes in inflammation and fibrosis in patients with available liver histology.61 Saroglitazar, a peroxisome proliferator-activated receptor agonist, has been approved in India for the treatment of NASH and for the treatment of dyslipidaemia in patients with diabetes.62
No improvement in liver histology has been reported with the use of statins compared with placebo in a randomized clinical trial.63 Oxidative stress, and more specifically, lipid peroxidation, is believed to play a large role on the pathophysiology of NASH. Antioxidant therapy has been considered as a potential treatment. A meta-analysis of clinical trials evaluating various antioxidant interventions, such as vitamins C and E, showed no benefit of these interventions in patients with NAFLD.64 The AASLD suggests that vitamin E may be used in patients with NASH who do not have diabetes.58
Obesity surgery has been reported as a viable option for the treatment of NASH in appropriately selected patients. In a retrospective analysis of 64 patients with biopsy-confirmed NASH who received bariatric surgery, 84% of patients revealed resolution of steatohepatits and 72% experienced fibrosis regression at follow-up liver biopsy 5 years later.65 Bariatric surgery has also been shown to reduce overall cardiovascular mortality in obese patients, compared with usual care.66
To date, four global phase III trials have been completed, or are in process, for the treatment of NASH (ClinicalTrials.gov Identifiers: NCT02548351, NCT03053063, NCT03053050, NCT02704403).67–70 These drug trials were on an accelerated pathway for approval based on liver histologic outcomes, with the caveat that any drug approved on this pathway for the USA and Europe will require an additional trial to evaluate long-term outcomes (liver outcomes, such as cancer, hepatic failure, liver transplant) and all-cause mortality. Of the completed phase III trials, selonsertib failed its primary outcome for both F3 and F4 fibrosis (ClinicalTrials.gov Identifiers: NCT03053063, NCT03053050), elafibranor failed its primary outcome (ClinicalTrials.gov Identifier: NCT02704403), and obeticholic acid met one of its two primary outcomes (ClinicalTrials.gov Identifier: NCT02548351); however, the FDA did not approve this medication for the treatment of NASH due to a variety of concerns.67–70 Resmetirom remains in a phase III trial.
Screening for non-alcoholic fatty liver disease
In the practice setting, screening patients at high-risk for NASH is an important process. Ultimately, the diagnosis can currently only be achieved by liver biopsy. Despite the fact that there is no currently approved pharmacologic treatment for NASH outside of India, there is still an opportunity for patient education and awareness of available clinical trials.
Some clinicians use elevated liver function tests (LFTs) as a method of screening for patients at risk for NASH. Published data report a rise in the number of LFTs performed in primary care physician practices.71 Elevated LFT can be associated with numerous potential diagnoses. In a clinical research setting of 1,118 patients with documented LFT abnormalities, the aetiology of the abnormal LFT was identified in 55% (614) of these patients. Interestingly, 24.3% of this group was diagnosed with NAFLD because there was evidence of steatosis on ultrasound examination of the liver, and there were no other identified possible causes for the elevated LFT.72 Another research group in a similar setting aimed to determine the degree of fibrosis in their patients with NAFLD, as this would be consistent with a high risk of NASH diagnosis. In this study, the NAFLD Fibrosis Score was used to determine the severity of fibrosis. Of the subjects with NAFLD, 7.6% had advanced fibrosis, 35.2% may have had fibrosis and 57.2% had no fibrosis.73 NAFLD is recognized globally as the most common reason a patient presents to their physician with an elevated LFT.74
Ultimately, it would be ideal to have a validated screening algorithm that could be used to identify patients at high risk for NASH. Figure 3 is a proposed algorithm for screening for patients with NAFLD who are at high risk of having NASH, and who should have a confirmatory liver biopsy. This algorithm was conceived after interrogation of a large USA claims and treatment database (IQVIA P360 database), in conjunction with a separate interrogation of an electronic medical record (EMR) of an endocrinology practice in the USA containing patients with both biopsy-positive and biopsy-negative NASH (Allscripts Professional EMR version 17.3.1, as accessed by Luke Snedacker, Lucas Research, November 2019).
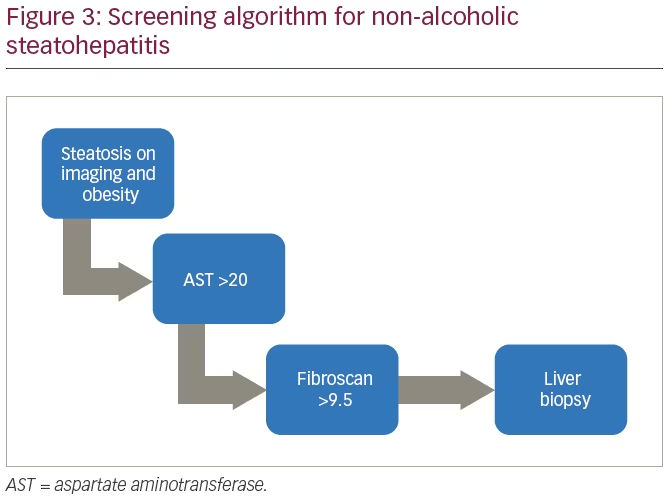
There are peer-reviewed publications which have reviewed the use of non-invasive biomarkers for the diagnosis of NAFLD.75 There are a number of commercialized assays for detecting NAFLD with varying sensitivity and specificity. These tests have not gained much popularity due to cost and the inability to confirm the diagnosis of NASH. A more economical method is scoring systems, which are based on commonly available laboratory and demographic information in the patient’s chart. These scoring systems (e.g. Fib-4 and NASH Fibrosis Score) are focused on determining whether a patient has liver fibrosis, a pathological finding in NASH. These scoring systems are better able to determine if a patient has no fibrosis or severe fibrosis, compared with mild or moderate fibrosis. A bedside medical device is available for measuring the degree of liver stiffness (fibrosis) or liver fat content; this is known as transient elastography. This device has good sensitivity and specificity for determining the absence or presence of extensive liver fat or fibrosis. It does not allow accurate specific fibrosis or steatosis grading and cannot substitute for liver biopsy for the diagnosis of NASH.
Endocrine/diabetes societies and non-alcoholic fatty liver disease
Globally, endocrine societies are developing recommendations for identifying patients with NASH in the endocrinologist’s practice. The Chinese Society of Endocrinology recently published guidelines which advocate ultrasound for the screening of patients at high risk for NAFLD, and the use of the NASH Fibrosis Score to determine which patients should be sent for liver biopsy.76 The increased prevalence of NAFLD prompted the American Diabetes Association to revise its 2019 recommendations for standard of medical care. In adults, adolescents and younger children, the recommendations are to conduct liver enzyme (aspartate aminotransferase [AST] and ALT) testing at the initial visit, and annually thereafter.77 In 2016, the European Association for the Study of the Liver, the European Association for the Study of Diabetes and the European Association for the Study of Obesity (EASO) published clinical practice guidelines for the management of NAFLD. Box 1 summarizes the major recommendations.78

Referral to gastroenterologist/hepatologist is recommended for persistently elevated or worsening transaminases in all age groups. These elevated enzymes should be closely monitored in patients with higher body mass index, higher waist circumference, elevated triglyceride levels and lower high-density lipoprotein cholesterol levels. Even before referral to gastroenterology/hepatology, the endocrinologist should maximize glycaemic, lipid and weight-loss therapies. In appropriate patients, glycaemic therapy should consider treatment with liraglutide or thiazolidinediones as an off-label treatment for NAFLD, as they have been shown to have some promise in preliminary studies.79 Published data in a broad population of patients at high risk of NAFLD have demonstrated that 72% of patients are either counselled on weight loss, or attempt weight loss on their own. Twenty percent of these patients were able to obtain a weight loss of 5% or greater at 1 year.80
As discussed previously, the aetiology of NASH is thought to stem from visceral adiposity and insulin resistance. Morbidity in this disease is related to both liver decompensation and heart disease. This points to NASH being a systemic disease. A study by Targher et al. evaluated three groups of patients, each including 45 males who were either healthy, overweight with biopsy-proven NASH, or overweight without ultrasound diagnosed hepatic steatosis. Patients with NASH had the highest levels of C-reactive protein, PAI-1 activity, triglycerides and HOMA level (indicator of insulin resistance), and the lowest adiponectin level.81 Patients with NASH in endocrinology practices who are the most insulin resistant, also have the worst cardiac risk factors and the highest ALT levels. The association between insulin resistance and obesity explains why these patients with liver disease have a high degree of cardiac disease. Before referral to the gastroenterologist/hepatologist for elevated or worsening levels of liver enzymes, simple scoring algorithms, such as the Fib-4 and AST to Platelet Ratio Index (APRI), can be used to predict the presence of hepatic fibrosis. A Fib-4 score of <1.45 has a 90% negative predictive value for advanced fibrosis, whereas a score >3.25 would have a 97% specificity and a positive predictive value of 65% for advanced fibrosis.82 For APRI, scores >0.7 have a sensitivity of 77% and specificity of 72% for predicting significant hepatic fibrosis.83
Because of the rising incidence of diabetes and obesity, NASH-related disease morbidity will be almost as common as the cardiac problems seen in many routine clinical practices. Therefore, it will be important in the non-gastroenterology practice to become versed in the diagnosis and care of patients with NASH. In the future, as with cardiac disease and referrals to cardiologists, referrals to hepatologists for NASH will occur when disease presentation is unusual or the patient needs an invasive procedure.
Non-invasive biomarkers will be critical for the awareness and diagnosis of NAFLD by endocrinologists. At present, research is looking at promising tests, such as plasma cytokeratin 18, oxidized low-density lipoprotein, interleukin-17 and others.84 Most endocrine, internal medicine and primary care practices will need to have access to a transient elastography device, which will give an estimate of hepatic fat and fibrosis presence at the bedside. This device, in combination with predictive algorithms or serum or imaging biomarkers, will assist these physician specialties in determining which patients are at risk for NAFLD, and which patients will require a liver biopsy for diagnosis and staging of disease.
Clinical research in non-alcoholic steatohepatitis
Patients with risk factors for NASH should be followed closely with management of associated metabolic abnormalities, and should receive a referral to a dietician and education regarding exercise. In a meta-analysis of clinical trials evaluating the efficacy of exercise in NAFLD, moderate-intensity exercise demonstrated a beneficial effect on liver fat content, independent of its impact on body weight.85 Screening for NAFLD should be part of the routine care for these patients in order to identify and educate patients with a diagnosis of NASH. In a population-based study in Europe, one in six patients with T2DM were non-invasively determined to have liver fibrosis using a combination of liver ultrasound and transient elastography.86 Once a diagnosis of NASH has been made, consideration for enrolment into clinical trials should also be considered.
Over the past 10 years, the number of clinical trials focusing on patients with NASH has increased dramatically. The current regulatory pathway allows approval of a drug to treat NASH based on very specific histologic improvement over a 52–72-week interval. However, longer-term data from liver outcome studies (carcinoma, liver failure, transplant) and all-cause mortality data will need to be collected over a longer period of time (3–5 years) to allow a drug to maintain its approved status, and to demonstrate true clinical efficacy outcomes to payers, regulatory agencies and clinicians. Patients entering a phase III trial may need to remain in that clinical study for a prolonged period of time. Between the increasing number of clinical trials and the length of time of phase III trials, there will be a continued high demand for subjects to enrol in these trials.
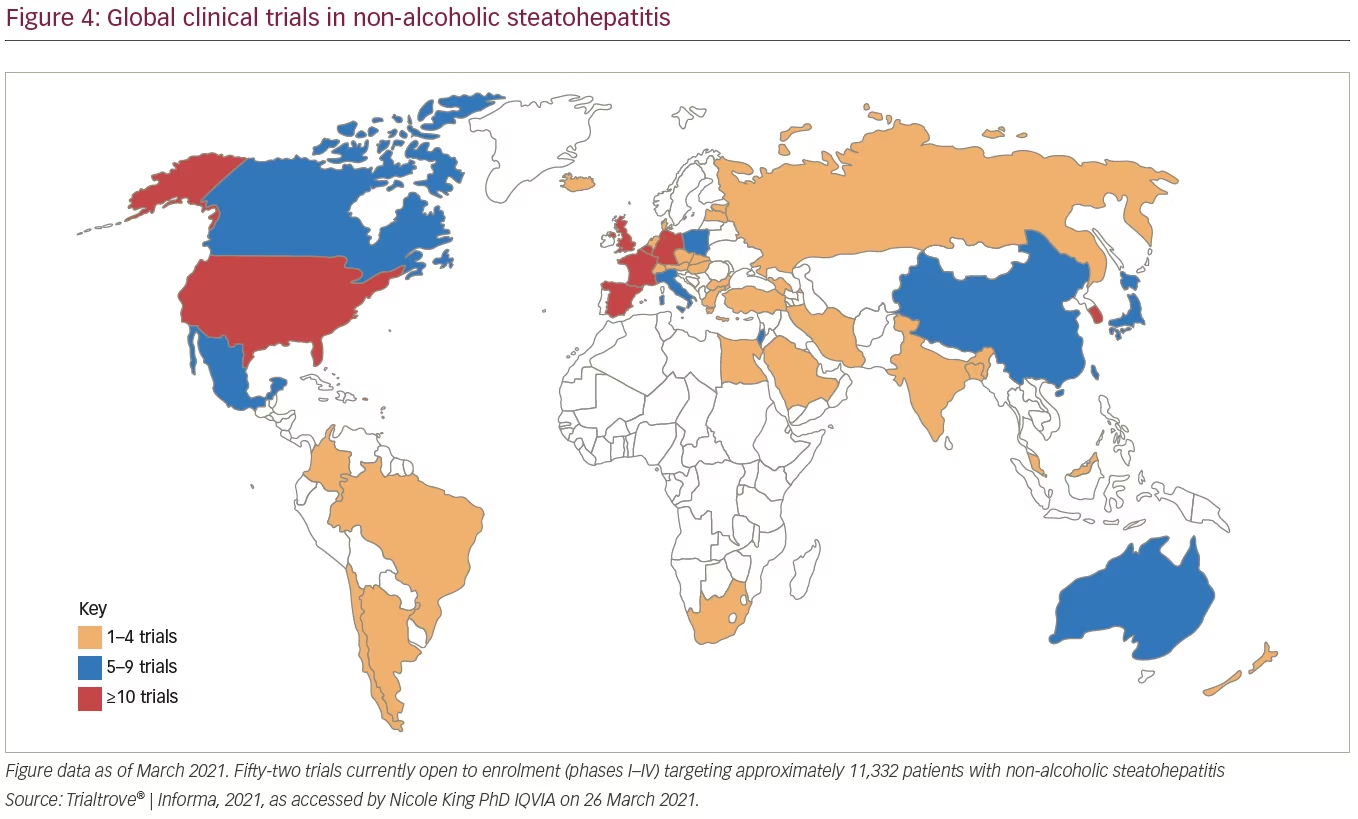
Currently, there are 52 NAFLD pharmaceutical trials underway globally. Figure 4 demonstrates the current status of pharmaceutical trials being performed in NAFLD as of 26 March 2021. Based on the data captured in Figure 4, the current volume of NAFLD studies will require 12,085 patients to fulfil their patient enrolment requirements.
Introduction of non-alcoholic steatohepatitis into clinical practice
Incorporation of the identification and care of patients with NASH into a clinical practice will be a shift for many clinicians, irrespective of their location at an academic medical centre or in the community. There is already a multitude of care issues in specific patient groups, such as those with T2DM or hyperlipidaemia, that must be addressed by physicians. This includes monitoring for the development of associated complications by providing routine cardiac evaluation, renal function assessment and ophthalmologic care. A focus on weight loss and control of HbA1c and plasma lipids is already the standard of care. Attention to the liver and the development of NASH will now need to be considered an important end-organ complication for many of the patients commonly seen in the endocrinology, internal medicine or primary care practice.
The ability to identify patients at risk for NASH, and to decide who may need to be referred to a hepatologist, will be an important component of each clinical practice’s standard of care. There is no one serum blood test or a radiograph that can identify a patient with NASH. However, physicians can stratify patients for further evaluation based on several factors including:
- treatment of patients with multiple metabolic-related disease states including obesity, T2DM, hypertension, hyperlipidaemia, hypothyroidism or PCOS
- elevated abdominal waist circumference
- platelet count <200,000
- abnormal LFT
- steatosis determined on imaging (ultrasound, computerized tomography or magnetic resonance imaging).
These patients should have an assessment of their hepatic fibrosis risk using an algorithm, such as the Fib-4 score or NASH Fibrosis Score. In some practices, the use of bedside transient elastography can be employed for further determination of hepatic steatosis and fibrosis. The current device for performing transient elastography is expensive, and reimbursement for performing the procedure is low. Some practices may elect to refer patients for transient elastography to a hepatologist, or to defray the cost of the transient elastography device by enrolling patients in NASH clinical research trials, where transient elastography has proven useful in the screening process for identifying patients who may be candidates for a given trial.
In the USA, liver biopsies are now often performed by interventional radiologists, and the tissue sample is read by a pathologist. A clinician faced with the possible diagnosis of NASH in a patient with presumptive liver fibrosis, especially moderate to severe fibrosis, may elect to send them for liver biopsy, especially given the fact that there is currently no commercialized pharmaceutical treatment option. Alternatively, they may elect to refer these patients to a hepatologist to make this decision. In either case, the focus is on the patient, the diagnosis of NASH, and the current treatment options, which include aggressive weight loss, control of hypertension and hyperlipidaemia, education on alcohol intake, and optimization of blood sugar control. Additionally, these patients can be considered for inclusion into a clinical trial.
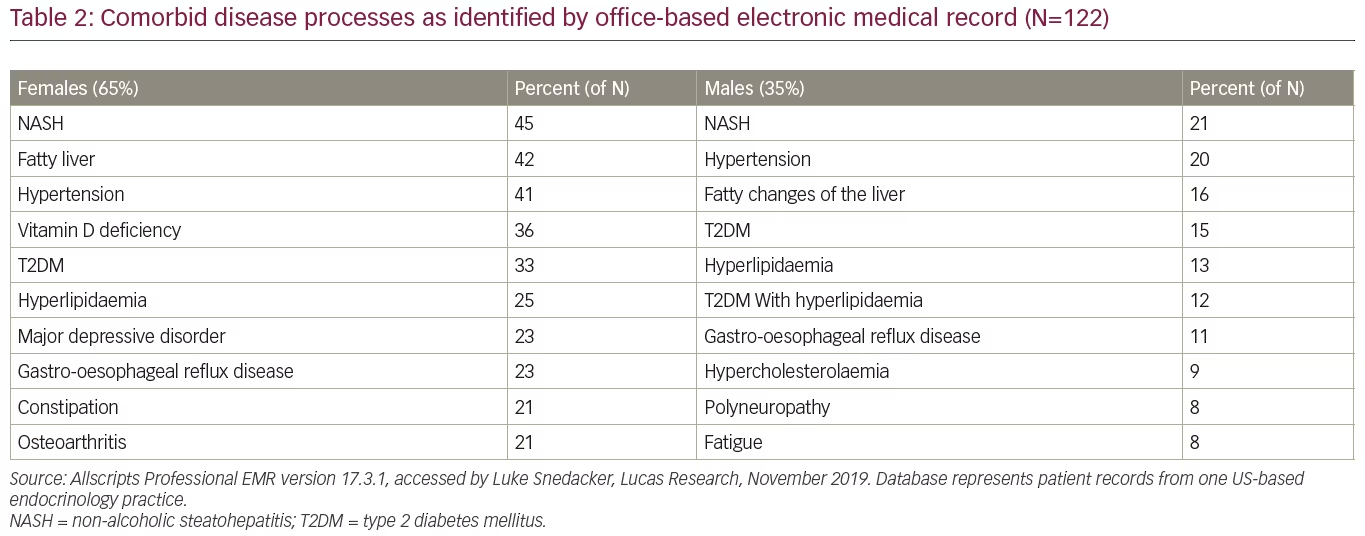
Using claims data from a large USA database, we have presented a snapshot of the comorbidities, non-specific symptoms and laboratory tests associated with NASH (Figure 1). A further evaluation of a community-based endocrinology practice electronic medical records of 122 biopsied patients with NASH revealed associated comorbidities, as seen in Table 2. Comparing the claims-based data with a community-based endocrinology practice electronic medical records revealed the same female predominance of the disease. Hypertension, T2DM and hyperlipidaemia were common comorbidities, and were numerically more common in females. In the office-based EMR analysis, fatty liver disease was a common comorbidity. Surprisingly, obesity was not a common comorbidity in the office-based EMR analysis; this could be the result of the office coding practice, where the presence of obesity is often under-recognized and under coded.
Conclusion
NAFLD, and specifically NASH, is becoming a growing healthcare concern. A recent healthcare economic model forecasted that NASH has become the fastest-growing category of liver disease requiring transplant over the past 20 years.87 The endocrinologist, internist and primary care physician stand at a pivotal position in the healthcare delivery system, as many of the diseases they commonly treat are associated with a higher risk of developing NASH. Currently there is only one drug approved for NASH (saroglitazar), and this is only approved in India. Pioglitazone and vitamin E are being used off-label for the treatment of NASH by some clinicians. Practice guidelines for endocrinologists are evolving by bringing into focus the identification and care of patients with NASH in their daily clinical practice. The endocrinologist, internist and primary care physician will play an increasingly important role in the clinical care and clinical research of the NASH patient population.