Insulin preparations extracted from bovine or porcine pancreatic tissue have served as the mainstay of diabetes therapy since 1923, when commercial production was established in Europe and the US.1 Animal insulin sources became a limiting factor to provide sufficient supply of insulin for the increasing clinical demand of insulin worldwide. When the molecular structure of human insulin was elucidated, attempts were made at total chemical synthesis but failed to provide a clinically relevant supply.2,3 A next step towards obtaining clinically suitable human insulin was processing of animal insulin by exchange of amino acids and extensive purification.4–6 The modified material was addressed as ‘semisynthetic human insulin’ and all pharmaceutical formulations (regular, neutral protamine Hagedorn [NPH], premixed insulins) were manufactured from such semisynthetic insulin. At the time when semisynthetic human insulin was introduced to the market, there was an intensive and partly acrimonious discussion about this change in insulin source and about the clinical relevance of the need for ‘human insulin’. When clinical studies confirmed the comparable efficacy of this new type of insulin, the discussion subsequently focused on the improvements related to further purification, in particular, in decreasing the formation of insulin-directed antibodies due to therapy, and reducing the risk of local and systemic allergic reactions.
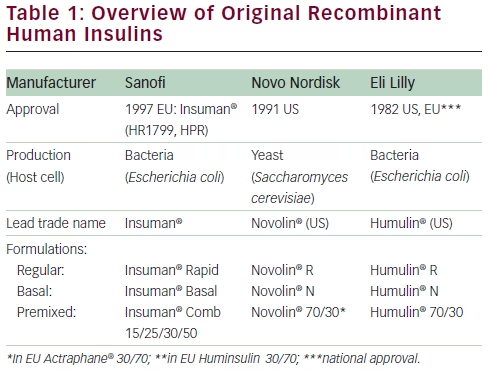
‘Recombinant human insulin’ became available in large amounts by recombinant DNA technology using fermentation in microorganisms (bacteria or yeast). Recombinant insulin has a superior level of purity and consistent quality compared with semisynthetic insulin. The process of biosynthesis was initially developed by Genentech and rapidly applied on an industrial scale by Eli Lilly,2,6 followed by pharmaceutical and clinical process development at Novo Nordisk and Sanofi (formerly Hoechst AG/Hoechst Marion Roussel/Aventis). These companies are the lead manufacturers of recombinant human insulin (see Table 1), the human insulin profiles and clinical aspects have been described and reviewed extensively.7–9 Since its first introduction to clinical therapy in 1982, recombinant human insulin represents the standard of care,10–12 even after the introduction of insulin analogues.12 The standard of care in diabetes therapy is addressed by international treatment guidelines.10–12 Many clinical studies with recombinant human insulins submitted for regulatory approval have not been published in detail. Bioequivalence studies performed with recombinant Insuman® (Sanofi, Paris, France) have been reported recently.13 “Scientific Summaries and Public Assessment Reports” of the European Medicines Agency (EMA) for marketed human insulins including Insuman14 are found at the EMA website, and approval information at the website of the US Food and Drug Administration (FDA).15
In this review, we report on unpublished pivotal clinical studies with recombinant Insuman documenting the efficacy and safety of semisynthetic and recombinant Insuman, and comparing recombinant Insuman with marketed formulations of Humulin® (Eli Lilly, Indianapolis, Indiana, US). Furthermore, the use of insulin formulations in clinical practice is discussed to review the place of recombinant human insulin in routine clinical practice of today.
Clinical Studies with Recombinant Human Insulins
The initial clinical studies with recombinant human insulins (Humulin, Novolin®, Insuman) explored the change from animal insulin to semisynthetic insulin and to recombinant human insulin formulations. Clinical studies in patients with type 1 or type 2 diabetes included paediatric and pregnant subjects.16,17 Clinical pharmacology studies using the euglycaemic clamp technique were performed to demonstrate bioquivalence between the insulin formulations.13 The clinical studies of 6 to 12 months duration focused on clinical efficacy and safety. Safety aspects comprised the incidence of hypoglycaemia, the perception of decreasing glucose levels (hypoglycaemic awareness) and the level of manifestations of antigenicity (hypersensitivity reactions). Special interest was directed at the antigenicity response (insulin-directed antibodies, and antibodies to Escherichia coli or Saccharomcyes cerevisiae proteins) remaining after extensive purification of the preproinsulin.18–23 Clinical study objectives were incidence and severity of hypoglycaemia,24–26 injection-site reactions and adverse events (AEs) profile. Glycaemic targets (glycated haemoglobin [HbA1c], fasting blood glucose [FBG]) were usually defined individually for each subject by the investigators. Insulin dose titration did not yet follow a fasting treat-totarget concept at that time.27
Humulin and Novolin
The pharmaceutical formulations of recombinant human insulins provided by the key manufacturers include soluble regular insulin, crystalline NPH insulin and premixed formulations (soluble insulin and NPH insulin in fixed ratios). The formulations were found to be bioequivalent and similar in efficacy and safety to those of semisynthetic insulin.7–9,13,19 Bioequivalence studies comparing porcine insulin with recombinant human insulin showed small differences in the time–action profile, but were comparable in clinical efficacy.19
Clinical studies with semisynthetic and recombinant insulin derived from baker’s yeast (Novolin, Novo Nordisk, Copenhagen, Denmark) showed similar profiles in efficacy and safety and established that patients with diabetes can be safely and effectively transferred from semisynthetic human insulin to recombinant human insulin with no change expected in the insulin dose.28–31
Clinical pharmacology studies with recombinant human insulin produced by fermentation in E. coli (Humulin, Eli Lilly, Indianapolis) established bioequivalence of semisynthetic and recombinant Humulin formulations.14,32,33 Extensive clinical studies were performed in patients with type 1 and type 2 diabetes14,33–36 to confirm consistent clinical efficacy when transferring patients to the recombinant formulations.14,33,34
Insuman
Recombinant Insuman was approved in Europe in 1997 and launched in 1999. The early clinical studies are summarised in the EMA approval documents.37 The formulations comprise regular soluble insulin (Insuman Rapid), an intermediate-acting insulin suspension that contains isophane
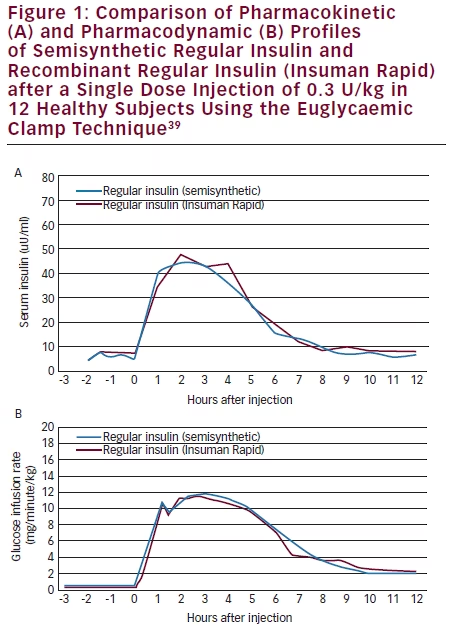
insulin (Insuman Basal), and premixed combinations of regular insulin and intermediate-acting insulins (Insuman Comb).13,38 During early studies, the bioequivalence of formulations based on semisynthetic insulin and recombinant Insuman was established (see Figure 1),39 subsequently bioequivalence studies for comparison with marketed recombinant insulin formulations were performed13 and followed by the clinical studies reviewed here.
Two pivotal clinical studies with recombinant Insuman were conducted in patients with type 1 and type 2 diabetes investigating the efficacy and safety of the change from semisynthetic insulin to recombinant Insuman,40 and in comparison with recombinant insulin formulations of
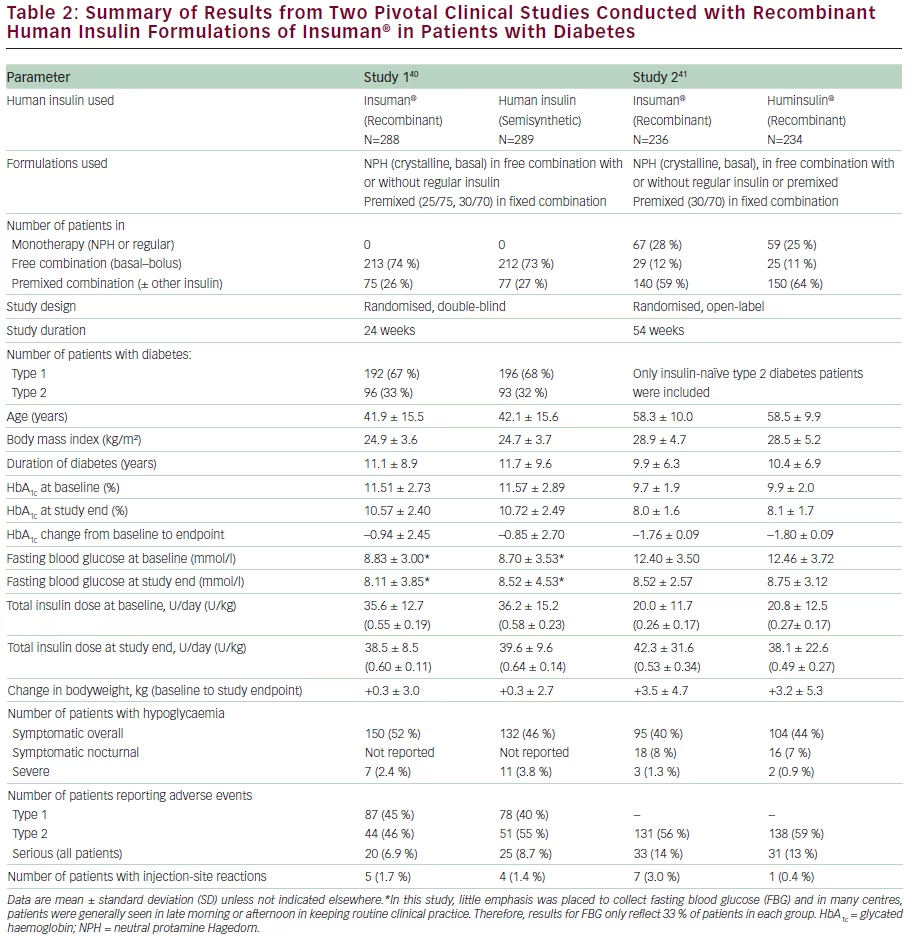
Huminsulin®.41 An overview of the patient characteristics and the key efficacy and safety results of the two studies are provided in Table 2.
In a first multinational, randomised, double-blind 24-week study including 575 adult patients with diabetes (87 % with type 1, 33 % type 2), patients were stratified either to a free combination of NPH insulin (crystalline, basal), with or without regular insulin, or to a fixed combination of Insuman Comb 25/75 and randomised to either recombinant or semisynthetic insulin preparations in each group. Of the randomised patients, 96 % had been treated with insulin prior to the study and 37 % of patients had a history of diabetic late complications, and 42 % had frequent mild hypoglycaemic episodes during the year before start of the study. The glycaemic target was to achieve a FBG value of 140 mg/dl or lower.
Both recombinant and semisynthetic human insulin achieved a similar decrease of HbA1c and FBG after 24 weeks. Subgroups analyses by age, gender, type of diabetes, prior insulin treatment and presence of diabetic late complications demonstrated similar outcomes. There has been an intense discussion about perception of hypoglycaemia in patients previously treated with animal insulins after changing to semisynthetic or recombinant human insulins.24,25 In this study no difference in incidence of symptomatic hypoglycaemia and in calculated episodes per patient-year were found, as well as no change in the perception of hypoglycaemia.
Antigenicity has always been a concern when using animal insulins. However, early studies showed that antigenicity decreased markedly when changing from animal insulins to recombinant insulins. In this study, the level of insulin antibodies related to insulin exposure before treatment was very low, and there was no relevant increase after treatment with semisynthetic insulin or recombinant Insuman. In addition, there was a very low level of antibodies detected to E. coli proteins in patients treated with recombinant insulin. The absence of such proteins is particularly relevant for the pharmaceutical quality of recombinant insulins after intensive purification. The number of patients with AEs, serious AEs and with local and systemic reactions to insulin injection also did not differ between the insulin treatments.
In a second multinational, randomised, open-label 54-week study in 473 insulin-naïve subjects with type 2 diabetes the efficacy and safety of recombinant Insuman was compared with recombinant Huminsulin formulations. Huminsulin formulations were selected as a comparator based on bioequivalence confirmed with Insuman.13 Treatments comprised regular insulin, crystalline NPH insulin and premixed insulins (Insuman Comb 25 and 50, Huminsulin 30/70). Selection of treatment regimen was at the discretion of the investigators and individual dose titration was applied to achieve the best possible glycaemic control for each subject.
The primary study objective was an evaluation of antigenicity and measurement of antibodies to human insulin and E. coli proteins.20–23 Further safety aspects included hypoglycaemia assessment, local or general manifestations of insulin allergy and clinical AEs during treatment.
As expected for insulin-naïve type 2 subjects, the insulin antibody binding increased in both treatment groups while on insulin treatment, with no relevant difference between groups. In both groups, increased insulin antibody binding was not associated with deterioration of metabolic control or a marked increase on the insulin dose or hypoglycaemia incidence. At study endpoint, 52 % and 49 % of Insuman- and Huminsulin-treated subjects, respectively, had detectable insulin antibody binding. Similar results were found for E. coli antibody binding status. Only two Insuman and eight Huminsulin subjects had an increase in their E. coli protein antibody titre from baseline to endpoint.
Randomised patients had a poor glycaemic control at baseline. As a result of insulin treatment, a clinically relevant decrease from baseline to endpoint was observed in HbA1c and FBG in both treatment groups, with no statistically significant difference (see Table 2). Throughout the entire treatment phase, 40 % and 44 % of Insuman and Huminsulin patients reported at least one episode of symptomatic hypoglycaemia, respectively, and only a few subjects in both treatment groups reported moderate or severe hypoglycaemia during the study. The frequency and spectrum of non-serious and serious AEs were comparable in both treatment groups. Hypersensitivity events of mild or moderate intensity were reported in 12 Insuman and in one Huminsulin subject, respectively. These events were associated with pre-existing skin disorders, allergic reactions to concomitant medication or allergic diathesis. None of the 12 Insuman subjects discontinued treatment because of a hypersensitivity event. Injection-site haemorrhage occurred occasionally and was attributed to poor injection technique. Injection-site reactions42 were reduced dramatically when educational training for regular changes in injection sites along with improved injection techniques were initiated during the study. None of the subjects in either treatment group discontinued treatment because of injection site reactions.
In summary, both studies demonstrated improvements in glycaemic control and good tolerability with Insuman in type 1 and type 2 diabetes patients comparable to comparator treatment. In addition, no difference in immunogenicity between Insuman and Huminsulin or semisynthetic insulin was found, an important characteristic of recombinant insulin formulations.20–23
Clinical Use of Recombinant Human
Insulin Formulations
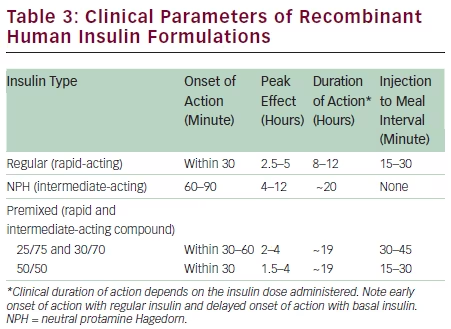
The change from semisynthetic synthesis to recombinant rDNA technology1,2 has enabled a worldwide human insulin supply of consistent high quality. The range of different insulin formulations derived from recombinant human insulin allows for an individual patient’s tailored treatment using different regimens that have been proved effective and safe in the long term (see Table 3). Hypoglycaemia associated with insulin treatment remains one of the major challenges during therapy; to minimise the risk, close monitoring and guidance for the patient is recommended, particularly during initial and any later dose titration. Self-monitoring of fasting and post-prandial blood glucose are helpful tools to avoid or reduce hypoglycaemia and to maintain blood glucose values in the target range. Therefore, patient education and guidance is a general task of insulin therapy to ensure a continued adherence to therapy and good metabolic control.
Regular Human Insulin
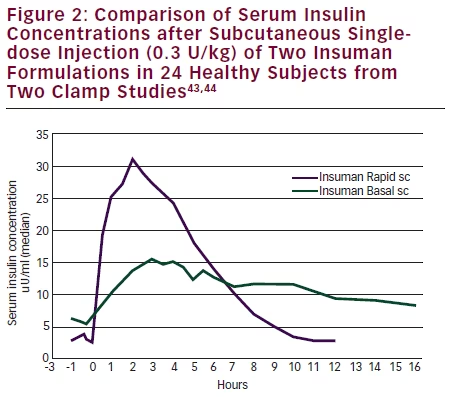
In this review, the use of formulations of recombinant insulin, in particular that of Insuman, is considered with references to daily clinical practice, in diabetes therapy of today. The clinical evidence for an injection-to-meal interval of about 30 minutes (prandial insulin) is based on the time–action profile of regular insulin,13,39 to match subcutaneous insulin absorption with ingestion of carbohydrates (see Figure 2).43,44 This ensures efficacy, albeit at the disadvantage of having to follow a more restrictive lifestyle. Subsequent studies have shown some advantage for insulin analogues in reducing the injection-tomeal interval, at the expense of increasing the cost of therapy.
In clinical emergency, Insuman Rapid may be injected or infused intravenously under strict glucose control. When using continuous subcutaneous insulin infusion (insulin pumps), there is a clear clinical preference for fast-acting insulin analogues in the paediatric population. Studies with a specific formulation (Insuman Infusat) in external portable insulin pumps have shown improved stability to minimise loss of efficacy, which may result from mechanical and thermal stress. A limited number of studies have been performed for the use of Insuman Infusat in external insulin pumps, and with Insuman Implantable in intraperitoneal insulin pumps.45,46
Neutral Protamine Hagedorn Insulin
Intermediate-acting NPH insulin has been used extensively for basal insulin supply, the clinical efficacy has been well documented47,48 and the associated quality of life has not been found to be worse when compared with long-acting insulin glargine.49 There has been a discussion about once- or twice-daily injections, in the morning and at dinner time/bedtime.50 Limitations of clinical utility when using NPH insulin are the duration of action and more frequent hypoglycaemia episodes than with long-acting insulin analogues. Another limitation is the need for re-suspension immediately before each injection.
In several clinical trials, where human NPH insulin was used as the comparator for insulin glargine47,45,51,52 comparable glycaemic control was found, whereas the incidence of nocturnal hypoglycaemia was reduced with insulin glargine. Decreased incidence of hypoglycaemia was also described with other long-acting analogue insulins (detemir, degludec). NPH insulin in vials or insulin pens needs to be re-suspended immediately before the injection. This requires patient guidance and instruction to ensure consistent adherence to this procedure. Twice-daily injections of NPH insulin, in the morning and at dinner time/bedtime, are recommended by some clinicians because the time–action profile of NPH insulin does not adequately cover the 24-hour period (see Figure 2). The recommendation for twice-daily injection is valid for premixed insulins, which contain a 70–75 % fraction of NPH insulin.
Premixed Insulins
In the early clinical period of using semisynthetic insulins from vials, patients used to perform the mixing themselves using two separate vials of regular insulin and NPH insulin. In several studies, premixed insulins were compared with self-mixed insulins, and formulations were developed for the use in cartridges containing a ratio of soluble to NPH insulin over a range which varied from 15/85 to 50/50.
Today, the ratio of 30/70 is most frequently used both in pens with cartridges and disposable insulin pens.38 Premixed insulins are recommended for patients with a regular lifestyle and consistent insulin requirement. When compared with premixed insulin analogues, they retain the advantages of low cost and established efficacy. The availability of reliable and affordable insulin pens has contributed markedly to patient convenience in countries with limited resources.53
Use in Pregnancy and Gestational Diabetes
Human insulin is the standard of care in pregnant women.17,54 In the early clinical studies in pregnancy, the change from animal insulins to recombinant insulin was addressed and subsequently implemented.17 Consistent glucose monitoring and dose adaptation is important throughout pregnancy and counselling needs to be established within the programme of pregnancy care for mothers with diabetes. Gestational diabetes develops during pregnancy and may disappear after parturition. The condition of gestational diabetes has received much attention, because there are established treatment options with insulin during pregnancy, which have considerable efficacy in preventing foetal macrosomia,55 in a similar manner as for women with established diabetes prior to pregnancy. The use of human insulin and Insuman formulations during pregnancy has been monitored in pharmacovigilance programmes (periodic safety updates, riskmanagement plan) and found to be safe.
Use in Paediatrics
The change from animal insulins to recombinant human insulin is well documented in the paediatric population7,16 and is found to be an advantage because the decrease in manifestations of antigenicity is particularly relevant in children. The preference for use in children has been included in guidelines.10 Consistent glucose monitoring is required because of the widely varying dose requirement and distinct changes in insulin requirement during the growth period of children.
The Place of Recombinant Human Insulin in Diabetes Therapy
When considering efficacy, there is clearly an established place for human insulin formulations in the therapy of type 1 (multiple daily injections) and type 2 diabetes. This is clearly addressed in current guidelines.10–12 The need for action is particularly urgent in type 2 diabetes.10 When comparing cost of therapies, recombinant human insulin formulations are the choice for countries in patients with limited resources. In countries with more ample resources, combination therapy is now extensively investigated, e.g. adding glucagon-like peptide 1 agonists or dipeptidyl peptidase 4 inhibitors,56,57 and by oncedaily injection of prandial insulin.27,56–58
Convenience of using insulins analogue is well established, and there is a certain advantage in reducing hypoglycaemic episodes.24,25,48 The established regiments of basal, premixed and basal–bolus therapy can be implemented with the available range of human insulin formulations when access to insulin analogues and reimbursement are not available
The essential conditions for improving therapy are glucose monitoring, its frequent implementation, continuing patient education about insulin injection technique42 and how to re-suspend NPH premixed insulins before each injection. Although adherence to recommendations for storage conditions is helpful, there is, however, no difference from the analogue insulins in this respect. In light of worldwide awareness that early implementation of insulin therapy can prevent or delay diabetes complications, access to affordable insulin therapy is the predominant factor when considering recombinant human insulin formulations.
Conclusions
As the burden of diabetes is predicted to increase dramatically in the next decades, the demand of insulin in sufficient amounts and at affordable costs remains a challenge, particularly in developing countries. For that reason, recombinant human insulin formulations are considered to be effective alternatives to insulin analogues in countries with limited healthcare systems and limited resources. Continuing patient education support programmes on disease management and correct use of human insulins are essential (e.g. re-suspension of NPH and premixed formulations, injection technique, adequate storage) for a key role of recombinant human insulins in diabetes treatment. In developing countries, improving access to human insulin can support initiatives for earlier insulin therapy, to improve glycaemic control in the communities, and finally to delay or reduce diabetes complications in the long term.







