In recent years, a variety of innovative solutions have been introduced that are designed to improve adherence to blood sugar testing among patients with diabetes, lower glycated Hemoglobin (HbA1c), and decrease complications associated with diabetes mellitus. The value of lowering HbA1c in preventing long-term complications of diabetes is broadly recognized. The purpose of this review is to provide an overview of the peer-reviewed literature documenting both the efficacy of mobile health (mHealth) solutions in improving adherence and lowering HbA1c, along with the impact of lowering HbA1c on nearterm costs and complications of diabetes. There are multiple variables to be considered when estimating the financial impact of an mHealth solution on preventing complications of diabetes and lowering medical costs within a healthcare organization. Those variables include, but are not limited to:
- An organization’s current population, diabetes prevalence, and overall medical costs;
- An organization’s current population with diabetes compliance with treatment protocols at baseline;
- An organization’s current diabetes-management programs;
- The percentage of the population with diabetes willing to participate in the program; and
- The proposed treatment interventions associated with the glucose monitoring data that will be generated by the mHealth system.
However, no estimate of cost-effectiveness for a proposed model can be generated without supportable assumptions on efficacy of such interventions in lowering HbA1c and, hence, near-term costs.
mHealth Solutions for Improving Control of Diabetes
Concommitant with the introduction of the first data-capable cell phones, innovators have sought to connect physicians and patients around the measurement and control of blood glucose. Initial solutions were based around connecting cellular radio devices to traditional blood glucose meters,1 fashioning blood glucose meters that could attach directly to early cell phones (typically called feature-phones as distinguished from smartphones),2 and relying on the patient to manually enter data via a cell phone application.3 Other mHealth programs have relied on home telemonitoring devices4,5 or web-based solutions.6 The most recent approach to mHealth for Diabetes has implemented cellular data communication capability within a glucose meter.7 This has the dual advantages of not imposing extra actions or cost on the patient, beyond those already associated with fingerstick glucose monitoring on the one hand, and providing the patient with immediate caregiver feedback on the other.
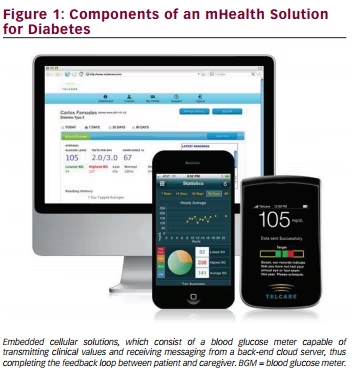
Embedded cellular solutions typically consist of a blood glucose meter capable of cellular data transmission, a back-end cloud server that is capable of receiving data, interpreting and displaying it to patients and caregivers, and ancillary mobile apps that may be used by authorized friends and relatives to assist the patient in managing his or her condition (see Figure 1). Although the US Food and Drug Administration (FDA) has recently relaxed its degree of regulation around mobile medical apps, mHealth systems that connect to regulated medical devices, such as blood glucose meters, and provide clinical guidance to patients remain regulated by FDA
Studies on the Impact of mHealth Solutions on Glycated Hemoglobin Reduction
The published studies that measure the feasibility and efficacy of diabetes blood glucose telemonitoring on H b A1c results are primarily small, randomized control trials (RCTs), which vary based on participant selection criteria (population age, gender, diabetes type, and baseline HbA1c), study duration, and intensity of treatment interventions. For example, telemedicine interventions that resulted in real-time modifications to a patient’s diabetes medications were associated with higher HbA1c reductions.
The following table summarizes recently published studies regarding the efficacy of tele-monitoring on reducing HbA1c results.
The mean decline in H b A1c based on the above studies varied from –0.35–1.9 percentage points. As indicated, study variations such as diabetes type, baseline HbA1c, patient age, and the intensity of the associated treatment interventions may have an impact on the results.
Studies Evaluating the Impact of Reduction in Glycated Hemoglobin on Medical Costs
There are a number of studies that evaluate the association between diabetes costs and glycemic control. Many of these studies compare the medical costs of the population with diabetes with poor glycemic control to those with sustained glycemic control. There is a sizable body of research evaluating the long-term impact of controlled HbA1c on medical costs; however, this model addresses the near-term medical cost impact.
Table 2 summarizes published studies that have evaluated the impact of improved HbA1c control on medical costs.
The studies above reflect evidence that lower HbA1c and diabetic medication adherence are associated with reduced inpatient and overall medical costs in the short term, with the savings timeframe varying from 1–3 years. The studies included in this review did not distinguish the extent to which the decrease in HbA1c was associated with better testing adherence (such as via an mHealth intervention) versus better medication adherence. As indicated above, this research did not include studies that evaluate the long-term impact of sustained HbA1c compliance on reductions in diabetic complications and healthcare costs. The long-term
Diabetes Control and Complications Trial (DCCT) and the Epidemiology of Diabetes Intervention and Complications (EDIC) studies identified that interventions aimed at achieving glycemic control as close to nondiabetic range as safely as possible reduced all of the microvascular and cardiovascular complications of diabetes.1,17 In researching the estimated cost savings, we have assumed that there is a direct correlation between improved blood glucose monitoring and improvement in medication adherence and HbA1c results. The studies differ in the assumptions regarding starting HbA1c levels or medication adherence levels, diabetes type, study duration, service types measured, and the population base (e.g., staff model Managed Care Organization, employer group, large payer). As a result, the medical cost savings estimates for these studies vary from approximately 3–17 % of total medical costs for diabetes patients. (In some studies, for extreme changes, such as for those patients with the highest baseline blood glucose level, e.g., over 10 %, showing sustained improvement, the medical cost savings were measured to be well over 20 %.) The midrange of the studies estimated the savings for patients with diabetes’ total medical costs to be within the 7–13 % range. This includes the sometimes increased drug cost of improved medication adherence.
Savings associated with deployment of an mHealth program are likely to be higher if the population is relatively higher cost; for example, if the program targeted patients with diabetes with the largest potential savings. Also, the savings would be higher for more aggressive monitoring and intervention programs. Several of the analyses were retrospective summaries of costs for patients with better versus worse levels of HbA1c or medication adherence, without a specific diabetes program involved. Their results could be exceeded by an effective, targeted program.
Based on our reviewof the studies described above, a reasonable midpoint assumption of medical cost savings associated with meaningful HbA1c reduction might be 10 % of medical cost for a commercial population and 7 % for a Medicare population. Again, these should be adjusted to reflect the population being analyzed. Lower and higher savings assumptions are reasonable. For example, one analysis measuring one deployment of Telcare’s system resulted in a 20 % reduction in the first year of use compared to the claim costs incurred in the base period.
9
Additional Components of Savings
Aside from direct medical savings associated with improved blood glucose monitoring and lower HbA1c, Medicare Advantage insurance plans should also consider the potential impact of such interventions on their star quality ratings. Under current Medicare regulations, improved quality ratings under this system trigger direct financial benefits through rebates and bonuses from the Medicare program. Higher star ratings and resulting revenue allow the plan to either decrease member premiums or provide additional supplemental benefits. Additionally, if a plan achieves a five-star rating, it permits them to market year round as opposed to only during open enrollment and special election periods.
Employers who are considering the implementation of mHealth programs for diabetes should also consider the economic impact of decreased worker absenteeism and increased worker productivity that may be driven by reduced complications of diabetes. In some employed populations, these factors may be as important as the projected savings in direct medical cost.
In summary, although the impact of mHealth solutions on lowering HbA1c is widely assumed to reduce only long-term complications of diabetes, a rapidly emerging literature suggests that meaningful financial and medical impact may be realized in the short term as well.







