Digestive Neuroendocrine Tumors
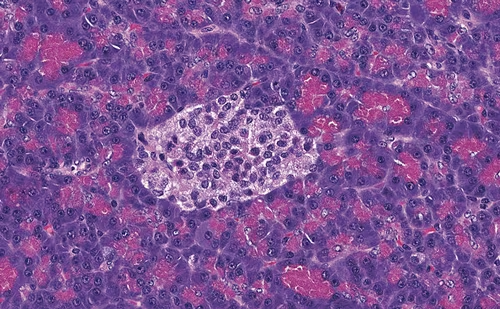
Digestive neuroendocrine tumors (carcinoids) derive from serotonin-producing enterochromaffin cells. The digestive neuroendocrine tumors are classified as:
- foregut—originating from the esophagus to the pancreas;
- midgut—‘classic’; presenting with the carcinoid syndrome that includes flushing, diarrhea and hypotension. They originate from the jejunum to the right colon and gonads; or
- hindgut—‘silent’; originating from the transverse colon to the rectum.
Digestive Neuroendocrine Tumors
Digestive neuroendocrine tumors (carcinoids) derive from serotonin-producing enterochromaffin cells. The digestive neuroendocrine tumors are classified as:
- foregut—originating from the esophagus to the pancreas;
- midgut—‘classic’; presenting with the carcinoid syndrome that includes flushing, diarrhea and hypotension. They originate from the jejunum to the right colon and gonads; or
- hindgut—‘silent’; originating from the transverse colon to the rectum.
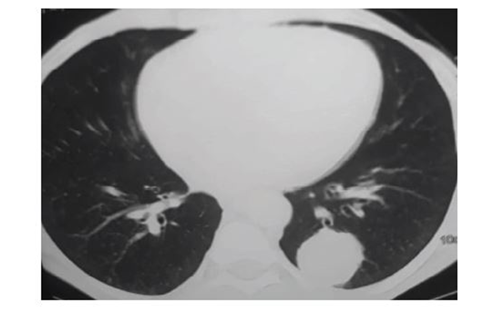
More than half of digestive neuroendocrine tumors originate in the gastrointestinal tract (with half of these in the small intestine), and the remaining from the lungs/bronchi. The overall incidence of digestive neuroendocrine tumors is estimated to be one to five per million population.1 Patients with midgut digestive neuroendocrine tumors may complain of vague abdominal symptoms for a long time (approximately nine years) before classic symptoms and signs, such as flushing, and excess gastrointestinal motility are observed.2,3 At this time, the disease has metastasized in 90 % of symptomatic patients.2,3 More than half of patients with digestive neuroendocrine tumors—via mechanisms that are not clearly understood— suffer from irreversible carcinoid heart disease. The endocardium shows fibrous thickening and the tricuspid and pulmonary valves are fixated.2,4 Genetics
Ten per cent of individuals with multiple endocrine neoplasia (MEN) type 1 have digestive neuroendocrine tumors. MEN1 is an autosomal dominant disorder caused by deletion of the MEN1 suppressor gene on chromosome 11q13. Forty to 80 % of patients with sporadic digestive neuroendocrine tumors also show loss of heterozygozity in chromosome 11 or deletion of the MEN1 gene.2,5 Pulmonary neuroendocrine tumors are associated with mutations in the p53 suppressor gene and variability in B-cell lymphoma 2 (Bcl-2) expression.2 Studies of polymorphisms of the nuclear factor-kappaB (NFκB) transcription factor tentatively point to differences in the genetics of digestive neuroendocrine tumors vis-à-vis pancreatic neuroendocrine tumors.6
Biochemical Diagnosis
Digestive neuroendocrine tumors in the fore- and midgut metabolize tryptophan to 5-hydroxytryptophan and synthesize and secrete neck-to-pelvis distribution and parasympathetic paraganglia are found in the neck and skull base.
Paragangliomas that are localized in the adrenal medulla are called pheochromocytomas (or more uncommonly termed adrenal medullary paragangliomas).54 The term ‘extra-adrenal pheochromocytomas’ is used to describe tumors of the sympathoadrenal system. There are no universally established criteria for defining malignancy in pheochromocytomas/ paragangliomas. However, capsular invasion, large tumor size (>5 cm) and weight (>80 g) may be indicators of malignancy. The clinical course may indicate malignancy, particularly with recurrent or metastatic disease.
Pheochromocytomas (i.e. adrenal medullary paragangliomas) are rare tumors with an annual incidence of one to four per million population.55 Furthermore, 0.5 % of subjects with hypertension and 4 % of those with an incidental adrenal mass have pheochromocytoma.55 The caveat is that these figures are approximate, since until a few years ago 18–60 % of tumors remained undiagnosed.54 The average lag time from the onset of hypertension to the diagnosis of pheochromocytoma is three years.56 Peak age for diagnosis of pheochromocytomas is between 40 and 50 years, with an almost equal female/male ratio. In most cases (downgraded from 90 to 85 % or less with the advent of newer molecular genetics studies, see below for details) these tumors are adrenal, sporadic, and solitary.
The symptoms of pheochromocytomas vary. The triad of tachycardia with diaphoresis and cephalalgia is encountered in 40–80 % of patients and is highly sensitive and specific for a presumptive diagnosis of pheochromocytoma.57,58 Hypertension—newly diagnosed or an exacerbation of known hypertension, most often paroxysmal—is common, occurring in over 90 % of patients, but is non-specific.58 Most paragangliomas are intra-abdominal and adjacent to the adrenals (approximately 85 %). Less than 15 % are intrathoracic and 1–3 % are cervical.59 Chromaffin-negative neuroendocrine tumors in the head and neck that are related to the parasympathetic nervous system, such as those originating from the carotid bodies or jugular bulbs, are also termed paragangliomas.60
Genetics
Familial syndromes with pheochromocytomas/paragangliomas include55 MEN type 2 (MEN 2); von Hippel-Lindau (VHL) syndrome; neuroectodermal dysplasias – neurofibromatosis type 1 (NF-1), tuberous sclerosis and Sturge-Weber syndrome; and other familial paragangliomas, especially those related to succinate dehydrogenase (SDH) gene mutations. In children, familial tumors are found twice as often as in adults.61 Activating germline mutations in the REarranged during Transfection (RET) proto-oncogene, usually in codons 634 or 918 (10q11.2), are implicated in the abnormal cellular proliferation of MEN 2 syndrome. Pheochromocytomas are usually adrenal and benign in MEN 2 and are bilateral in more than 50 % of patients.55
Missense mutations in the VHL tumor suppressor gene, usually in codon 167, 3p25–26, are commonly implicated in the pathogenesis of VHL syndrome. Twenty to 50 % of subjects have mostly benign adrenal pheochromocytomas, and slightly less than 50 % have bilateral disease.62 The genetic background of pheochromocytomas observed in subjects with neuroectodermal dysplasias is yet to be elucidated. Mutations in the NF-1 tumor suppressor gene—associated with von Recklinghausen’s disease—have been observed (17q11.2; in 90 % of cases). The risk of pheochromocytoma in patients with NF-1 is approximately 1–5 %.56,63
Familial pheochromocytomas or head/neck paragangliomas are seen in subjects with germline mutations in subunits B, C and D of the SDH gene. The risk of extra-adrenal and/or malignant disease is high for SDHB mutation carriers.62 SDHB mutations also predispose to head and neck paragangliomas.64 SDHC mutations are a rare cause of head and neck paragangliomas.64 SDHD mutations are associated with benign adrenal and extra-adrenal paragangliomas or multifocal head and neck paragangliomas.64 SDHB/SDHD mutations have been found in patients with Carney-Stratakis syndrome (they also have paragangliomas).65 The former are also associated with renal tumors, gastrointestinal stroma cancer and thyroid cancer.61 Mutations in the SDHA and SDHAF2 (SDH 5) family were recently found and linked to hereditary, but not sporadic, paragangliomas.66–69
It has been suggested that the transmembrane-encoding gene TMEM127 (chromosome 2q11) is a newly discovered pheochromocytoma susceptibility gene. Pheochromocytomas with TMEM127 mutations are transcriptionally related to tumors bearing NF1 mutations.70 Expression of SNAIL (a zinc-finger transcription factor) may predict the metastatic potential of pheochromocytoma.71
Approximately 15 % of all pheochromocytomas/paragangliomas are associated with germline SDH mutations. Immunohistochemistry is apparently the most cost-effective method of genetic testing—particularly if biochemistry is not available or considered, or results are negative.61,72,73 Furthermore, there is sufficient evidence to suggest that genetic testing should be carried out in all patients with pheochromocytomas-paragangliomas. If cost is a concern, then testing should at least be available to those <50 years.61
Biochemical Diagnosis
Chromaffin tumors that are hormonally active may secrete catecholamines episodically, however, they metabolize catecholamines to metanephrines continuously. Free metanephrines in plasma and 24-hour urinary fractionated free metanephrines are the most accurate methods for establishing the diagnosis of pheochromocytoma. Their respective sensitivity ranges from 99–100 (plasma) and 97–100 % (urine) and their specificity is 89–94 (plasma) and 69–95 % (urine).61 Biochemistry is not only useful for establishing the diagnosis of pheochromocytoma/paraganglioma but can also guide further testing (including genetic testing). In subjects with MEN2 or NF1, there is predominantly elevation in metadrenaline, whereas in subjects with VHL there is predominantly elevation in normetadrenaline.61 Care must be taken to normalize metadrenaline levels for populations with normal blood pressure, match them for gender and age,74 and avoid interference from medications.75 Dynamic testing is rarely sought.Gucagon testing is now considered to be obsolete.76 Suppression with clonidine and measurement of plasma-free normetadrenaline is accurate but applies only to normetadrenaline-secreting tumors.77 Head and neck paragangliomas were previously rarely considered to be hormonally active. A substantial number of them (almost one-third) are, however, biochemically active. This is supported by increased excretion of the dopamine metabolite 3-methoxytyramine.78 Most abdominal and thoracic SDHB-paragangliomas hypersecrete either normetadrenaline or normetadrenaline and dopamine. Some only hypersecrete dopamine and are almost silent biochemically.64
Imaging
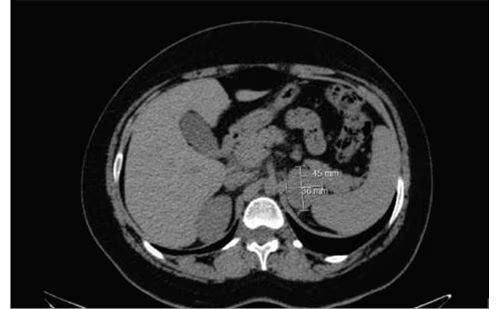
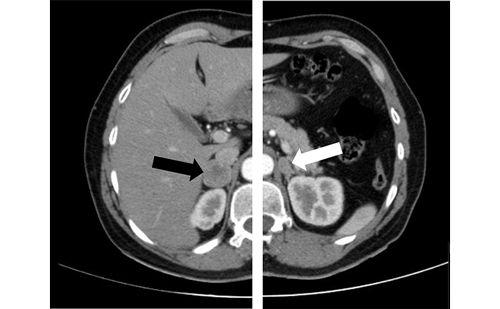
CT imaging has 93–100 % sensitivity for detecting intra-adrenal pheochromocytomas of approximately 0.5 cm in diameter.79 The sensitivity of CT is slightly lower, at 90 %, for localizing extra-adrenal disease of approximately 1 cm in size.79
MRI offers slightly better sensitivity. Pheochromocytomas usually show a characteristic very high T2-weighted signal on MRI unless there is a hemorrhage or intratumoral necrosis. MRI is very good for evaluating the relationship of pheochromocytomas with blood vessels. This is of importance when surgery is planned.
CT/MRI should be used in patients with biochemically proved pheochromocytoma/paraganglioma. For most patients imaging is limited to the adrenals/abdomen, whereas evaluations of the thorax, neck and head are used when there is suspicion of malignant/ metastatic disease. For head and neck paragangliomas, MRI may better explore tumor anatomy vis-à-vis this region’s blood vessels. Conventional or MRI angiography may also be very helpful.80–82 Although positive CT/MRI studies can be diagnostic, their specificity may vary from 50–90 %.55 Thus, negative anatomical imaging studies may not be diagnostic.83 Furthermore in patients with previous surgery poor quality imaging may lessen utility, particularly if recurrence is suspected.79 For such cases and for cases of extra-adrenal or malignant/ metastatic disease, the use of functional methods is preferred. There are two paths for functional imaging of chromaffin tumors.
- Specific methods for these tumors, since chromaffin tumors express the human noradrenaline transporter (hNAT). This permits the use of radiolabelled ligands of molecules that enter the catecholamine synthesis pathway or their analogues and specific vesicular monoamine transporters for storage in intracytoplasmic vesicles.
- Non-specific methods that make use of the high glucose metabolism of tumors or expression of STRs.84
Specific functional imaging methods should be carried out first. If results are negative, non-specific modalities should be sought, particularly if recurrent, metastatic or malignant disease is suspected. MIBG is a catecholamine precursor that is taken into pheochromocytoma cells via hNAT. Nowadays, it is labelled with iodine-123 (123I-MIBG), permitting better quality imaging than 131I-MIBG. CT imaging—standalone or as single-photon emission CT (SPECT)—is also possible.85
Dopamine is a catecholamine precursor. PET with 18F-dopamine is better than 131I-MIBG for imaging adrenal and/or benign pheochromocytomas or localizing metastatic pheochromocytomas.86–88 DOPA is converted into dopamine and then transported into pheochromocytomas by hNAT (the large neutral amino acid transporter may also play a role in this). Standalone PET with 18F-DOPA or combined with CT has been used for localizing benign adrenal pheochromocytomas and head and neck paragangliomas with good results.89–91
PET with 18F-labelled deoxyglucose (FDG) is currently widely available and is used for localizing various tumors and the staging of neoplastic disease. FDG PET is a convenient and accessible modality for localizing pheochromocytomas that are negative with specific functional imaging modalities (particularly metastatic disease).
Pheochromocytomas and paragangliomas express STRs (mostly types 2, 3, and 5), although conflicting results have been presented in the past.92–97 Octreotide is an octapeptidic somatostatin analog that is labelled with 111In for SRS. Despite intense splachnic/renal abdominal accumulation, it is a useful non-specific tool for localizing malignant and/or metastatic pheochromocytomas or paragangliomas with a sensitivity approaching 90 %.98
18F-dopamine PET/CT is the preferred technique for localizing primary pheochromocytomas and paragangliomas and to rule out metastases. 18F-DOPA PET and 123I-MIBG scintigraphy make an equally good second choice. For patients with known metastatic paraganglioma, 18F-dopamine PET is the choice for those with an unknown genotype. 18F-FDG/18Fdopamine PET should be the preferred option in SDHB mutation carriers. 18F-DOPA/18F-dopamine PET is preferable in non-SDHB patients.64,99
Management
The definitive treatment for pheochromocytoma/paraganglioma is surgery. For hormonally active tumors, a pre-operative blood pressure-lowering/normalisation regimen should be followed using selective alpha1 blockers (prazosin, doxazosin and others) or non-selective, non-competitive alpha blockers (phenoxybenzamine). If, despite selectivity tachycardia ensues, beta blockade is given after sufficient alpha blockade has been achieved.56,100,101 Pre-operative management with calcium blockers, nifedipine, angiotensin-converting enzyme (ACE) inhibitors or alpha-methyl-para tyrosine (Demser) have been also used.100,102,103
Laparoscopic surgery is possible for abdominal tumors up to 9 cm in diameter. Partial (cortical-sparing) adrenalectomy is used more often—particularly for small tumors.104–106 A transabdominal approach is reserved for malignant tumors,107 where debulking surgery and/or adrenalectomy is advised.108 Non-competitive alpha blockade with long-acting agents such as phenoybenzamine is preferred for keeping blood pressure under control in patients with symptomatic malignant and/or inoperable disease.56 Demser is also given to block catecholamine synthesis. Biochemical evaluation with plasma and/or urine adrenaline should be carried out two to six weeks post-surgery.53 Annual biochemical work-up for the first five years and once every two years thereafter is the minimum follow-up requirement. In the case of persistence or recurrence, localization studies should be sought. Sixty per cent of malignant pheochromocytoma sites show avid 131I-MIBG uptake.103 In specialized centres such tumors can be treated with therapeutic 131I-BG in single or fractionated doses totaling 200–1,400 mCi. Approximately 30 % of tumors show an objective response to therapy (40 % biochemical response) and 40 % of tumors remain stable (20 % biochemically).108 Radioiodine therapy may lead to serious adverse events, particularly in terms of bone marrow suppression.109–111 Less experience has been obtained with labelled somatostatin analogs.81 Overall, combination chemotherapy with dacarbazine cyclophosphamide and vincristine does not confer any significant survival benefit.112 Other regimens include etoposide plus cisplatin or etoposide plus lomustine with 5-fluorouracil.108 Radiofrequency ablation of metastatic foci can also be used.113 Another experimental modality is sunitinib, a multiple tyrosine kinase inhibitor.114
Prognosis
The life expectancy of patients with benign pheochromocytoma/ paraganglioma that has been successfully excised may not be different from that of the general population. Nevertheless, half of the patients that are successfully operated on have continued hypertension63,103 and overall 16 % of patients operated on for pheochromocytoma/paraganglioma have recurrent disease within 10 years.115 In a recent case series of children with pheochromocytoma/ paraganglioma, all were found to harbor a predisposing mutation but were alive after follow-up of five years.116 In a large cohort of patients with pheochromocytoma, however, mortality from a second neoplasia was four-fold higher compared with that of the general population.117
Recently, levels of the adrenomedullin RDC1 receptor were reported to be four times higher in malignant than in benign pheochromocytomas. Cells expressing SNAIL were frequent in metastatic pheochromocytomas compared to being absent in tumors without metastases. Despite these reports, the use of adrenomedullin RDC1 receptor and SNAIL levels as prognostic factors in pheochromocytoma/paraganglioma is not yet envisaged.71,118 Pheochromocytoma-paraganglioma syndrome can be diagnosed reliably by immunohistochemistry.73 There are no criteria to predict survival following malignant pheochromocytoma. Surprisingly, however, 15-year survival rates of almost 50% have been reported, with a combination of therapeutic modalities.119
Modalities Currently being Evaluated/Introduced into Practice
Quantification of pheochromocytoma/paraganglioma vesicular monoamine transporter content indicates whether the tumors are MIBG-avid.95,96,120 As PET imaging accessibility increases worldwide, more patients with pheochromocytoma/paraganglioma will be evaluated with PET studies. Ultratrace 131I-MIBG has very high specific activity and holds promise for future therapeutic applications.48 New modalities for the medical management of malignant pheochromocytomas are currently being assessed. Among these, the combination of temozoline and thalidomide or therapeutic somatostatin analogues have shown some encouraging results.108